Pathological causes.
B- Causes due to injury: Falling with bent or crossed legs...
Pathological causes.
C- Direct cause: Due to falling with bent or crossed legs...
Indirect causes: Due to traffic accidents, work accidents... D- Direct causes: Due to traffic accidents, work accidents...
Maybe you are interested!
-
 Describe the clinical symptoms of acute appendicitis.
Describe the clinical symptoms of acute appendicitis. -
 Present the Causes, Epidemiology, Clinical Symptoms, Treatment and Prevention of Japanese Encephalitis.
Present the Causes, Epidemiology, Clinical Symptoms, Treatment and Prevention of Japanese Encephalitis. -
 Study on clinical features, pathology and treatment results of non-epithelial gastrointestinal cancer at Viet Duc Hospital - 17
Study on clinical features, pathology and treatment results of non-epithelial gastrointestinal cancer at Viet Duc Hospital - 17 -
 Basic electronic engineering - City College of Construction. HCM Part 1 - 1
Basic electronic engineering - City College of Construction. HCM Part 1 - 1 -
 Basic Burn Rate Experimental Formulas
Basic Burn Rate Experimental Formulas
Indirect cause: Due to falling with bent or crossed legs...
Question 2 : Functional symptoms of fracture of both tibia bones:
A- Pain: Pain after injury for a few hours, then gradually decreases.
Partial loss of function: Patient has difficulty standing.
B- Pain: Pain a few hours after injury, there are cases of shock due to pain.
Partial loss of function: Patient has difficulty standing.
C- Pain: Pain a few hours after injury, there are cases of shock due to pain. Complete loss of function: Patient cannot stand.
D- Pain: Pain after injury for a few hours, then gradually decreases.
Complete loss of function: Patient cannot stand.
Question 3 : Late complications of fracture of both tibiae:
A- Neurovascular injury. Secondary displacement, nutritional disorder. B- Nutritional disorder. Secondary displacement.
C- Dislocation. Pseudarthrosis. Nutritional disorders. Secondary displacement. D- Dislocation. Pseudarthrosis. Nutritional disorders. Delayed bone healing.
Question 4 : First aid for a patient with a broken leg at a primary health care facility: A- Let the patient rest until the shock is gone.
Pain relief injection.
Temporary immobilization according to principles. Transfer patient to higher level.
B- Shock room.
Correctly immobilize the limb with a splint. Inject reinforcement and cardiac support.
Explain to the patient and then transfer to a higher level. C- Shock prevention. Immobilize the limb with a splint according to the principles.
Cardiac support injection.
Real immobilization with thigh-leg-foot casts.
D- Let the patient rest until the shock is gone. Give pain relief injections.
Fixed temporarily according to the principle.
Lesson 58
BROKEN CLAVULA
TARGET
1. Describe the cause of clavicle fracture
2. Describe the clinical symptoms of clavicle fracture
3. Describe the initial first aid method for clavicle fractures at the primary health care level.
office
CONTENT
Clavicle fractures account for about 10% of all fractures. They are common because the bone is shallow and curved in an S-shape. Diagnosis is easy, treatment is simple, and prognosis is good.
1. Cause
- Direct cause: Due to direct impact on the bone (rare).
- Indirect cause: Falling and hitting the shoulder on the ground (common).
2. Anatomy and pathophysiology
2.1. Fracture line: Most fractures are in the shaft of the bone, the fracture line is diagonal downward, inward and backward.
Under the bone there is a neurovascular bundle under the clavicle that can be damaged.
2.2. Displacement
- The inner end is pulled upward by the sternocleidomastoid muscle.
- The outer end is pulled downward, forward and inward by the Deltoid muscle, the pectoralis major and the strength of the upper limbs. Therefore, the two ends of the bone overlap and the shaft is shortened.
3. Clinical symptoms
3.1. Mechanical energy
3.1.1. Pain: Pain immediately after injury, healthy arm supporting injured arm, head tilted towards fracture.
3.1.2 .Reduced motor function: The affected limb has limited movement.
3.2. Physical symptoms
3.2.1. Look
- The fracture site is swollen and raised.
- There are bruises on the skin.
- The shoulders are pulled down and further away from the spine.
3.2.2. Palpation: Feel the bone head protruding under the skin and painful.
3.2.3. Measurement: The sacro-scapular-sternal segment on the broken side is shortened.
3.2.4. X-ray: Determine location and type of fracture.
4. Treatment
4.1. Treatment at primary health care facilities
Warming, pain relief, injection of stimulants, cardiac stimulants.
Temporary immobilization with figure 8 bandage then transfer to higher level for treatment.
4.2. Treatment methods at the upper level
- Pull and straighten. Fix with figure 8 tape.
- Chest - shoulder - wing - leg - hand plaster cast.
- Bone fusion surgery (in cases of difficult reduction or complex fractures)
VALUATION
Please choose the best answer for the following questions: Question 1: The collarbone is easily broken because:
A- Curved bones. B- Small bones. C- Skin-like bones. D- Brittle bones.
Question 2: The main cause of clavicle fracture: A- Falling on hands.
B- Fall on shoulder.
C- Direct hit.
D- Due to illness.
Question 3: Common combined injuries in clavicle fractures: A- Injury to the acromioclavicular joint.
B- Radial nerve injury.
C- Subclavian nerve and blood vessel damage. D- Soft tissue damage.
Lesson 59
Fracture of the humerus
TARGET
1. Describe the symptoms of a fracture of the humerus shaft.
2. Describe the treatment of humeral shaft fractures at primary health care facilities.
CONTENT
1. General
Fractures of the humeral shaft include fractures of the humerus from the lower border of the pectoralis major muscle to about 4 finger widths above the elbow crease.
This is a common fracture caused by direct trauma to the bone or by falling on the hand or elbow.
Fractures of the humeral shaft are simple to treat, but can cause two complications: radial nerve palsy and pseudoarthrosis.
2. Pathology
2.1. Broken line
Fractures in the middle and lower thirds of the humerus. The fracture line may be oblique, spiral, or transverse.
2.2. Displacement
- Fracture of the upper third of the bone: More displaced, the upper segment is abducted and pulled forward by the Denta muscle and the pectoralis major muscle, the lower segment is displaced inward.
- Fracture of the lower third of the bone: less displacement.
3. Symptoms
3.1. Functional symptoms
3.1.1 .Pain: After injury, pain increases with movement.
3.1.2. Complete loss of motor function: The patient cannot lift his arm.
3.2. Physical symptoms
3.2.1. The arm is swollen, round, and loses the folds between the muscles. The limb is short.
3.2.2. Manual manipulation of the fracture site causes sharp pain. A “crackling” sound may be heard (Do not do this).
- If you come late and see a bruise on your arm, you need to check if the radial nerve is paralyzed. If paralyzed, the wrist cannot be extended (stork neck deformity).
- Check the pulse to see if there is a broken blood vessel?
3.3. X-ray : Straight and oblique X-rays detect the fracture and the degree of displacement of the two ends of the bone.
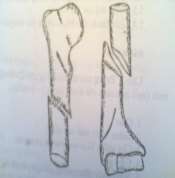

Figure 59.1. Fracture of the humerus. Figure 59.2. Image of a drooping hand with a stork's neck.
4. Complications
4.1. Radial nerve palsy
Because it is located in the spiral groove, close to the bone, when the shaft of the humerus is broken, the radial nerve is easily damaged, can be cut or clamped between the two ends of the broken bone.
4.2. Prosthetic joints
Common, usually due to improper treatment.
5. Treatment at primary health care facilities
- Local pain relief by injecting 0.5 - 1% Novocaine into the fracture site.
- Place temporary splint, properly.
- Heart and strength injections.
- Explain to the patient and family, transfer the patient to a higher level.
VALUATION
Please choose the best answer for the following questions: Question 1 : Functional symptoms of humeral shaft fracture:
A- Pain: Pain after injury, pain increases with movement.
Complete loss of motor function: The patient cannot lift his arm.
B- Pain: Pain after injury, pain gradually increases.
Complete loss of motor function: The patient cannot lift his arm.
C- Pain: Pain after injury, pain increases with movement.
Partial loss of function: Patient has pain when lifting arm.
D- Pain: Pain after injury, pain gradually increases.
Partial loss of function: Patient has pain when lifting arm.
Question 2 : Physical symptoms of a fracture of the humerus with radial nerve damage: A- The hand cannot be flexed, called stork neck deformity.
B- The hand and wrist cannot be extended, called stork neck deformity. C- The fingers cannot be extended, called stork neck deformity.
D- Fingers I, II, II contract; fingers IV, V extend, called stork neck deformity.
Question 3 : Common complications of humeral shaft fractures: A- Closed fracture becomes open fracture. Secondary displacement.
B- Closed fracture becomes open fracture. Radial nerve palsy. C- Pseudo-joint. Dislocation.
D- Pseudo-arthritis. Radial nerve palsy.
Question 4 : Complications of radial nerve palsy in humeral shaft fracture:
A- Because the radial nerve lies outside the spiral groove, close to the bone, when the shaft of the humerus is broken, it is easily damaged. It can be cut or caught between the two ends of the broken bone.
B- Because the radial nerve lies outside the spiral groove, on the outside of the bone, when the shaft of the humerus is broken, it is easily damaged. It can be cut or caught between the two ends of the broken bone.
C- Because the radial nerve is located in the spiral groove, close to the bone, when the shaft of the humerus is broken, it is easily damaged. It can be cut or caught between the two ends of the broken bone.
D- Because the radial nerve is located in the spiral groove, on the outside of the bone, when the shaft of the humerus is broken, it is easily damaged. It can be cut or caught between the two ends of the broken bone.
Question 5: Treatment of humeral shaft fractures in primary health care:
A- Local pain relief by local injection of 0.5 - 1% Novocain.
Traction, temporary fixation with splint according to principles. Antibiotic injection.
Explain to the family and transfer the patient to a higher level. B- Local pain relief by local injection of Novocain 0.5 - 1%.
Apply temporary splint, according to principles. Inject cardiac and strength support.
Explain to the family and transfer the patient to a higher level. C- Local pain relief by local injection of 0.5 - 1% Novocain.
Correct traction and fixation. Cardiac and power injections.
Explain to the family and transfer the patient to a higher level. D- Local pain relief by local injection of 0.5 - 1% Novocain.
Place temporary splint, according to principles. Inject antibiotics.
Explain to the family and transfer the patient to a higher level.
Lesson 60
Fracture of the 2nd Bone of the Forearm
TARGET
1. Describe the clinical symptoms of a fracture of the 2nd shaft of the forearm.
2. Describe the method of treating fractures of the two forearm bones at the primary health care level.
office
CONTENT
1. General
Fractures of the shafts of the forearm occur at any age. They can be caused by direct trauma to the forearm. They are more common due to indirect trauma, such as falling on your hand, causing the forearm to bend and break. This is an important fracture because the bones are displaced, affecting the precise movements that the radius and ulna bones coordinate to create.
2. Pathology
2.1. Broken line
- Transverse fracture
- Oblique fracture
- Torsion fracture.
2.2. Displacement

Figure 60.1. Common displacement positions in forearm fractures
a. High fracture (above the pronator teres muscle)
b,c. Middle and low fracture (below the pronator teres muscle )
Displaced fractures of the two forearm bones are complicated because the broken bones are pulled by many muscles from the arm, forearm and hand. In addition, the interosseous membrane of the two bone shafts pulls, causing the two broken ends to be displaced a lot.
2.2.1. Two broken bones overlap each other.
2.2.2. Two broken bones displaced to the side.
2.2.3. Torsional displacement along the bone axis.
2.2.4. Fold the angle at one or two bones.
3. Clinical symptoms
3.1. Functional symptoms
3.1.1. Pain: Pain in the forearm, especially when doing pronation or supination movements.
3.1.2. Complete loss of function: The healthy arm supports the injured arm.
3.2. Physical symptoms
3.2.1. Look: Deformed limb.
- The forearm is swollen and round like a tube, the folds are no longer clear.
- The bruise spread.
- Bend the angle causing the forearm to bend.
- Lateral displacement causes the forearm to bulge, the front of the wrist turns inward (pronator), because the pronator muscles pull in the lower segment, the upper part of the forearm turns outward.
3.2.2. Palpation: Touch the patient's painful fracture site.
Check for associated injuries: Check radial pulse, check movement and sensation in the extremities to prevent complications of vascular and nerve compression or rupture, especially Volkman syndrome.
3.2.3. X-ray: Take 2 straight and oblique films to determine the location of the injury and the displacement of the 2 ends of the broken bone.
4. Complications
4.1. Early complications
4.1.1. Converting closed fracture to open fracture.
4.1.2. Damage to surrounding tissues: Damage to blood vessels and nerves.
4.2. Late complications
4.2.1. Deviation
4.2.2. Prosthetic joints
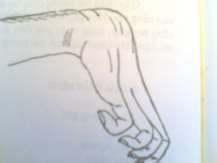

Figure 60.2. Volkman syndrome Figure 60.3. Proper immobilization
5. Treatment at primary health care facilities
- Local pain relief with Novocain 0.5 - 1% injection.
- Temporary fixation with splint according to principles.
- Injection of stimulants and cardiac stimulants.
- Explain to the patient and then transfer to a higher level for treatment.
VALUATION
Please choose the best answer for the following questions: Question 1 : Functional symptoms of a fracture of both forearm bones:
A- Pain: Pain in the forearm, especially when moving.
Complete loss of function: The healthy arm always supports the injured arm.
B- Pain: Pain in the forearm, especially when moving.
Partial reduction of mechanical energy.
C- Pain: Pain in the forearm, especially when doing pronation and supination movements.





