According to author Nguyen Phuoc Hiep in 2017 [13], each pharmacy has an average of 2 salespeople, with about 70 customers/day. With such a small number of customers, pharmacy staff have a lot of free time and need to take advantage of that time to apply measures to improve the quality of consultation for each patient.
4.2. Drug use consultation situation of pharmacy pharmacists
4.2.1. Consulting rate
Medication consultation not only helps patients use medications safely, appropriately, and effectively, but also helps patients understand the treatment method and the medications they are using. This helps patients have more confidence in health care, increases treatment compliance, and can bring about better treatment results.
Maybe you are interested!
-
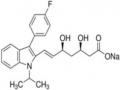
 Draw the Frame or General Formula of Each Drug Group (If Any); Structural Formula of Substances in the Chapter.
Draw the Frame or General Formula of Each Drug Group (If Any); Structural Formula of Substances in the Chapter. -
 Some Equipment In Injection Drug Production
Some Equipment In Injection Drug Production -
 Overview of the Department of Pharmacy, Drug and Therapeutics Committee
Overview of the Department of Pharmacy, Drug and Therapeutics Committee -
 Research on extraction and purification of conessin, kaempferol, nuciferin from medicinal herbs as reference standards in drug testing - Hoang Thi Tuyet Nhung - 30
Research on extraction and purification of conessin, kaempferol, nuciferin from medicinal herbs as reference standards in drug testing - Hoang Thi Tuyet Nhung - 30 -
 Motives for drug trafficking of prisoners at Z30D prison - Department V26 - Ministry of Public Security - 1
Motives for drug trafficking of prisoners at Z30D prison - Department V26 - Ministry of Public Security - 1
A study directly observing 269 cases of customers buying OTC drugs at 21 pharmacies in Hue city showed that 61.0% of customers received advice from pharmacists when buying drugs and 39.0% of customers did not receive any advice. Of the consultation cases, 59.2% were proactively consulted by pharmacists and 40.8% were requested by customers.
These results are different and discrepant when compared with the research results: Pham Tuyen in Hanoi in 2011 [28]: only 18.7% of customers did not receive advice. However, another study by Tran Thi Phuong conducted in Hanoi in 2016 [20] showed that 43% of customers did not receive any advice from pharmacists. A customer role-playing study in Germany in 2003 [34] showed that 98% of pharmacies provided advice to customers. However, 36% of pharmacies only provided advice when requested by customers. The percentage of pharmacies that only care about selling and pay little attention to ensuring safe, effective, and reasonable use of drugs is still quite high.

Our research team conducted an educational intervention with the aim of not only improving the skills and knowledge of drug use counseling but also the awareness of pharmacy pharmacists about the implementation of counseling. The post-intervention role-play study to evaluate the quality of the intervention recorded the following results: 100% of pharmacies provided drug use counseling to customers, with 80% being provided by pharmacists.
proactively and only 20% of cases were asked and requested by the pharmacist in advance. Thus, the consultation rate has increased significantly, demonstrating the effectiveness of educational intervention on the awareness of drug use consultation of pharmacy pharmacists. There is a need for more in-depth research and long-term intervention, contributing to improving the quality of safe, rational and effective drug use in the community.
4.2.2. Qualifications of the consulting pharmacist and consultation time
The results recorded through direct observation showed that only about 20.73% of the consultations were provided by university pharmacists, the majority of the remaining cases were provided by college pharmacists (42.1%) and secondary pharmacists (37.2%). The results showed that the presence of university pharmacists in pharmacies, although not in the majority of cases.
Our role-playing study was conducted at the same pharmacies that participated in the training. Through the survey at the training session, 5.3% of the participating pharmacists were pharmacists with university degrees, 2.6% with community pharmacists, and 92.1% with pharmacists with general practice out of a total of 38 pharmacists. In the role-playing study, for objective reasons, we could only complete it at 30 pharmacies, and to ensure the objectivity of the study, we could not confirm the professional qualifications of the consulting pharmacists.
A study in Hanoi [20] showed that there was no university pharmacist in the pharmacy, all the drug sellers were college or high school pharmacists. Besides the awareness of the importance of drug counseling, the lack of skills and professional knowledge of clinical pharmacy of drug sellers may be the reason for the low rate of drug counseling.
The consultation time was short, most of the communication time between pharmacists and customers lasted no more than 3 minutes (64.0%) and rarely lasted more than 5 minutes (0.6%). The average consultation time observed through role-playing research was nearly 4 minutes, and up to 20% of consultations lasted >5 minutes. The reason may be that pharmacists conduct more questions and answers with pharmacists than with actual customers.
This result is consistent with a survey in Korea in 2016 [52] where the consultation time at the pharmacy was greater than 5 minutes, accounting for only 6.8% and up to 51.2% of patients were dissatisfied because the consultation time was too short. Even in developed countries, the consultation activity
Pharmacy consultations are also not routine, recorded at only 62.2% in the US, 25% in the UK and over 50% in Canada [30]. However, a study in Tuyen Quang [2] showed that consultation times of more than 5 minutes were quite high (57.5%).
4.2.3. Consulting steps
4.2.3.1. Information collection
Collecting patient information is necessary for customers buying medicine, this contributes to showing concern and sharing with the patient's health condition, on the other hand, helps pharmacists exploit the most basic information about the subject using the medicine, symptoms, medical history, etc. thereby accurately identifying the disease and selling the right medicine as well as giving reasonable advice.
The results before and after the intervention were significantly different, information about drug users, age and symptoms were the three most exploited information by pharmacists from customers. The rate of collecting information about users increased from 52.4% to 93.3%, age increased significantly from 46.9% to 80.0%, and information about symptoms was also more focused, increasing from 63.4% to 80%. This shows an improvement in pharmacists' information exploitation skills after the educational intervention.
The results we recorded through direct observation are similar when compared with the research results: Nguyen Minh Tam in Hanoi in 2009 [23]; Nguyen Van Phuong in 2013 in Nghe An [17]; and Dinh Thu Trang, in 2012 in Binh Duong [27] pharmacists selling drugs asked about the users and symptoms accounting for 66.0 - 70.0% and were the information with the highest proportion.
At the same time, our research results, as well as results from other studies, show that the content on time of symptom onset, medical history, medication history, and drug allergies has not received much attention (<30%).
Lack of interest in exploiting information from customers by pharmacists can lead to unreasonable drug sales, causing unsafe and ineffective drug use for patients.
4.2.3.2. Providing information
In addition to selling drugs, pharmacists are also responsible for providing drug use advice to customers, understanding how to use drugs safely, appropriately, and effectively, which affects the treatment effectiveness of patients. Drug use advice also demonstrates the skills and qualifications of pharmacists, creating trust in customers, making patients feel secure in using drugs during treatment.
After the intervention, the rate of drug information provided to customers increased, specifically, the rate of consultation on drug indications increased from 46.7% to 65.8%, on dosage increased significantly from 52.4% to 94.7%, on number of doses/interval of doses increased from 61.0% to 100.0%. The rate of consultation on time of use compared to meals also increased significantly from 38.4% to 60%. However, information on adverse effects and contraindications was rarely provided to customers and it is noteworthy that information on handling missed doses, overdoses and storage was not consulted at all. The reason for this lack of advice may be that in direct observation and role-play situations, no drugs require special storage, but in actual practice, pharmacists will encounter cases where drugs are sold in suppository dosage forms, drugs with temperature-sensitive active ingredients, etc., so information on storage must be advised to customers.
These figures are quite similar to other studies on the following counseling contents: dosage, frequency of use (>60%), time of use (>26%), adverse effects (2 – 16%), drug interactions (2 – 5%) [1], [10], [17], [23].
Before the intervention, 18.9% of cases where pharmacists gave information reminding patients in which cases they should go to a medical facility were recorded during observation, but in the role-play study after the intervention, no advice was recorded. Compared with the study in Hanoi in 2016 [20], 13.3% of cases where pharmacists reminded customers to go to a medical facility. The reason may be that we created a role-play scenario, from the characteristics stated in the scenario, customers do not need to go to a medical facility but can self-treat, so information about which cases should go to a medical facility is easily overlooked by the pharmacists.
In addition to verbal consultation, pharmacists need to provide additional written data to help customers retain information, helping patients use drugs safely and appropriately. Research shows that 38% - 40% of drugs with drug information are sold to customers. However, this result is quite low when compared to some other role-playing studies in Hanoi that showed results of 46 - 58% [18], [20], [23].
In general, after training, pharmacists paid more attention to providing drug use advice to users, and the advice provided was more complete.
4.2.3.3. End of consultation
In order to ensure effective consultation, it is necessary for the pharmacy pharmacist to check the customer's level of understanding, as well as check if the customer has any questions or concerns about any problems that may occur when taking the medicine and answer those questions.
However, it can be seen that this issue has not received the proper attention of pharmacy pharmacists when in the observational study, only about 20% of cases summarized the consultation and checked the level of understanding and memory of the customer, and only 12.8% of cases pharmacists were interested in whether the customer had any further questions. These results were even lower when in the role-play study, there was no checking of the buyer's level of understanding, summarizing information was done at a very low rate (6.7%) and in 16.7% of cases pharmacists confirmed whether the buyer had any further questions or concerns.
However, the results obtained from direct observation in our study were higher than the study from customer feedback at Tran Thi Phuong's pharmacy, Hanoi 2016 [20] when it showed that all the consulting information was not checked by the drug seller.
4.3. Evaluation of the effectiveness of interventions to improve the quality of cold management advice
4.3.1. Evaluation of the effectiveness of cold management counseling knowledge
Drug sales and drug use consultation are professional activities that demonstrate the quality of pharmaceutical practice at pharmacies.
community health care. If this activity is not appropriate, it can lead to various consequences such as direct impact on the health, safety of patients, costs for patients and society. Therefore, DSNT not only need to have proficient counseling skills but also must have solid professional knowledge to provide quality counseling to patients.
Most pharmacists have intermediate pharmacy qualifications, they have not been fully educated in clinical pharmacy, professional knowledge plus lack of updating professional knowledge [13] and rarely use reference documents to guide drug use [24], so intervention to improve knowledge for pharmacists is very necessary.
Within the scope of the topic, we only conducted training on knowledge of cold management. The purpose of the study is to evaluate the effectiveness of the intervention, as a basis for further research, and to intervene to improve the quality of consultation. However, we also provided a "Medication consultation handbook for pharmacy pharmacists" including 30 common symptoms/diseases often encountered in pharmacies, as a consulting support tool for pharmacists.
The training session was conducted in 3 hours and 30 minutes, in the form of presentations, knowledge assessment was conducted based on pre- and post-training assessment forms, the content of assessment questions was built closely following the training content. The results showed a statistically significant difference (p <0.05) between the rate of correct answers to questions related to cold management before and after training. Specifically, the sharpest increase was in knowledge about precautions when using H1 antihistamines, from 15.8% to 86.8%, OTC analgesics and antipyretics, from 21.1% to 84.2% and causes of colds, from 39.5% to 94.7%. The content about the contagiousness of colds increased from 63.2% to 97.4%, typical symptoms of colds increased from 36.8% to 71.1%. The number of patient referrals to medical facilities also increased from 1.89 ± 1.06 to 4.97 ± 2.64.
An educational intervention study conducted in 2013 [50] to improve knowledge of diarrhea management in children in 5 localities across the country also showed improvement in pharmacists' knowledge after 3.5 hours of training. An intervention study
Another educational study conducted in Ba Vi district in 2012 [14] also demonstrated the effectiveness of the intervention to improve health workers' knowledge in antibiotic use for children under 5 years old.
This result shows that the training intervention has had a certain effect on the knowledge of participating pharmacists, thereby contributing to improving the quality of practice in the community.
4.3.2. Evaluation of the effectiveness of cold medicine sales practices
Results from the knowledge assessment showed an increase in knowledge of cold management advice before and after training. Of note was the application of the training knowledge to the practice of dispensing medicines to patients. We conducted a study and evaluated the medicines sold for the common cold in adults and common cold in children.
In cases where customers come to the pharmacy to buy medicine for self-treatment without a prescription, pharmacists are only allowed to sell OTC drugs.
The average number of drugs sold per patient when coming to the pharmacy to buy cold medicine was 5 drugs - the situation of buying medicine for adults and 4 drugs - the situation of buying medicine for children.
Cold treatment groups include: antipyretic analgesics, cough suppressants, decongestants, and sedative H1 antihistamines.
The most sold drugs are analgesics and antipyretics with the active ingredient paracetamol (100% for adults with colds and 87.5% for children with colds). Paracetamol is sold as a single-ingredient drug and a combination drug containing paracetamol with other cold-treating active ingredients. Among the cases of paracetamol being sold, there were 2 cases where NDV received ≥ 2 drugs containing the same active ingredient paracetamol. Currently, there are many drugs containing paracetamol on the market (only in the period from 2016 to February 2017, 214 drugs containing paracetamol were granted circulation registration numbers [26]) and there are many drugs containing paracetamol alone combined with other active ingredients to increase treatment effectiveness. These two characteristics make overdose cases more likely to occur.
Paracetamol due to duplicate active ingredients. Although paracetamol is considered a relatively safe active ingredient, it can easily cause liver toxicity if used in high doses for a long time.
Cough medications for cold management include cough suppressants and mucolytics. Combination medications containing the cough suppressants codeine and terpin are among the most common combinations on the market. 28.9% of NDV cases were sold this type of medication for colds in adults. While none were sold for children. This is entirely appropriate because the Ministry of Health recommends not using cough medications containing codeine for children under 12 years old. Another cough suppressant, dextromethorphan, was sold quite a lot in our study cases (57.1% of adult cases and 31.3% of children's cases). However, dextromethorphan is not an OTC drug according to the latest List of Non-Prescription Drugs (issued with Circular 07/2017 - TT/BYT issued by the Ministry of Health on May 3, 2017 [4]). This active ingredient is still considered an OTC active ingredient according to the US Food and Drug Administration (FDA) and has just been removed from the OTC drug list in our country since 2014. Pharmacists may not have been aware of the latest OTC drug list issued by the Ministry of Health because the percentage of pharmacies with OTC drug lists is also very low [24].
H1 antihistamines are a class of drugs commonly used in the treatment of colds, including sedative H1 antihistamines (including active ingredients such as chlorpheniramine, diphenhydramine, doxylamine, etc.) and non-sedative H1 antihistamines (including active ingredients such as cetirizine, loratadine, fexofenadine, etc.). However, studies have shown that non-sedative H1 antihistamines are not effective in the treatment of colds [47], and this knowledge was provided by the research team to pharmacy pharmacists during an educational intervention on drug use skills and knowledge. In addition, post-training test results showed that 86.8% of pharmacists answered correctly about this information. However, in reality, the majority of H1 antihistamines sold by NDV are non-sedative H1 antihistamines (loratadine, cetirizine, fexofenadine).