4.1. Limit local damage:
- Hemostatic pressure bandage
- Limit movement, immobilize the sprained limb
- Cold compresses on the affected area help reduce swelling and pain.
- Do not massage or apply heat to the sprained area.
- Pain reliever
4.2. Specific treatment according to YHHĐ:
- Grade 1 sprain:
Mild illness, quick recovery
Apply ice to the affected area for 10-15 minutes.
Avoid moving the injured joint or limb.
When the pain is gone, immediately exercise the joint.
- Grade 2 and 3 sprains:
Plaster bandage to immobilize the sprained joint area, duration # 6 weeks
Ligament suture: when grade 3 sprain is completely torn ligament
Start with light exercise, then gradually increase after 6-8 weeks.
- Severe sprain:
Novocaine block in the painful area.
Joint immobilization: plaster cast, splint, and bandage
3 - 4 weeks for ankle and knee sprains
2 weeks in case of wrist sprain.
After removing the cast, massage to prevent muscle atrophy and joint stiffness.
4.3. Treatment according to Traditional Medicine
4.3.1. Principle:
- The first stage of anti-inflammatory and pain relief follows the principle:
Apply cold compresses to the affected area
Immobilize the sprained joint
- Correct sprains and dislocations to return to normal position (repositional orthopedics)
- Apply topical medicine and oral medicine according to the following treatment methods: promoting qi, activating blood circulation, and clearing the meridians.
4.3.2. Topical medications:
4.3.2.1. Topical medications
Local remedy: Balm for sprains and dislocations
- Ingredients of the medicine: 8g of Ligusticum wallichii, 8g of Polygala tenuifolia, 8g of Dipsacus root bark, 8g of Dipsacus root bark, 8g of Rhizome of Polygala tenuifolia, 8g of Cistanche deserticola, 8g of Saposhnikovia divaricata, 8g of Saposhnikovia divaricata, 12g of Asarum sieboldii, 12g of Atractylodes macrocephala.
- How to prepare: Grind the ingredients into a fine powder, mix with sesame oil and melted wax, and beat into a paste to apply to dislocated joints or sprains.
- Uses: Reduce swelling, relieve pain.
4.3.2.2. Sprain treatment
- Ingredients: 8g of Sanh nam tinh, 8g of Xich thuoc, 4g of Sanh xuyen o, 8g of licorice, 1 handful of Sanh ma tien, 8g of cam toai, 2 handfuls of Sanh thao o, 8g of cinnamon, 1 handful of cloves, 8g of Te tan, 8g of Nhu huong, 8g of Dai rhubarb, 4g of camphor, 4g of borneol.
- Uses: Blood circulation: reduces swelling, relieves pain
- How to make: Grind all ingredients finely, stir-fry with vinegar or wine. Apply the medicine to the sprained area, change the medicine after 24 hours.
4.3.3. Oral medication:
- Prescription: Tiet cot thong mach thang : Dang quy 20g, Ha thu o 20g, Toai bo 12g, Hoang cam 8g, Lien duan 12g, Forsythia 8g, Nhu huong 8g, Moc duoc 8g, Lien gia bi 12g, Sanh dia 20g
- How to use: Mix with 500ml of water (3 cups) and cook over low heat until 150ml (1 cup) remains and drink warm.
- Uses: Clearing blood vessels, reducing inflammation, and relieving pain
DISLOCATION
TARGET:
After completing the course, students MUST:
1. Understand the general pathology of Dislocation according to modern medicine
2. Understand the concept of dislocation according to Oriental medicine
3. Understand the causes, symptoms and treatment of some traumatic dislocations.
CONTENT
1. GENERAL
1.1. Definition:
Dislocation is the partial or complete displacement of joint surfaces from each other, which can occur in all types of joints, especially joints with a wide range of motion and often have to bear force.
The cause is often due to direct or indirect trauma to the joint, due to incorrect posture, or it can also be congenital or due to joint disease.
1.2. General anatomy and physiology of joints
A joint is where bones meet together. The general structure of a joint usually consists of 5 components:
- Articular cartilage surface, subchondral bone layer, synovial membrane
- Joint capsule and ligaments
- Tendons and muscles around the joint
- Motor and sensory nerves to joints
- Blood vessels nourish the components of the joint.
The basic function of a joint unit is to both connect and move bones, thus helping to stabilize position, move parts, and move the body in space.
Based on the mobility of the joint, people divide joints into 3 types: mobile joints, semi-mobile joints and immobile joints.
- Mobile joints are the type of joints that can move easily, this type is the most common in the body. The joint surface of each bone has a layer of smooth, shiny and elastic cartilage, which reduces the friction between the two ends of the bone. In the middle of the joint is a cushion filled with mucus secreted by the wall of the sac called the synovial sac. Outside the joint layer are tough and elastic ligaments, going from one end of the bone to the other, forming a tight sac to cover the two ends of the bone. Thanks to this structure, the joint moves very easily.
- Semi-mobile joints are joints in which there is usually a cartilage disc between the two ends of the bones that limits the movement of the joint.
- Immovable joints are joints that simply connect bones, without any components of the joint socket, so they are immobile or have little movement in function. These bones fit together thanks to small saw teeth or because the edges of the bones overlap like fish scales... so when the muscles contract, the joint does not move, for example the bones of the skull and some facial bones.
1.3. Basic injury of dislocation:
When a joint is dislocated from its normal position, the components that make up the joint will be more or less damaged, manifested by:
- Joint capsule tear
- Ligament rupture
- Rupture of blood vessels causes intra-articular hematoma
- Sensory nerve damage causes pain
- Tendons are often torn, and muscle contraction causes joint deformity and abnormal movement (spring sign).
- The articular cartilage surface is usually not damaged if adjusted early, but if left for a long time it can cause damage to the articular cartilage.
1.4. Classification of dislocations: Orthopedic trauma specialists classify dislocations based on 5 aspects:
- By time: emergency dislocation (before 48 hours after injury), early dislocation (before 3 weeks) and late dislocation (after 3 weeks, old dislocation). Correction of old dislocations is often difficult and ineffective.
- According to anatomy: complete dislocation, subluxation, and dislocation with fracture (fracture and dislocation).
- According to recurrence: first dislocation, recurrent dislocation, frequent dislocation.
- According to clinical manifestations: closed dislocation, open dislocation, dislocation with neurovascular complications, locked dislocation (small broken bone fragments are inserted into the joint, making it difficult to reduce).
- According to the position of the dislocation on the bone.
Classification of dislocations is crucial for diagnosis and treatment, so it is necessary to carefully analyze all of the above aspects.
1.5. Traditional Chinese Medicine concept of dislocation:
Dislocations and fractures are commonly called Chiet thuong in TCM. To treat Chiet thuong, TCM has Thuong khoa (or Trat da khoa) in TCM surgery.
The main cause is trauma such as falling, being beaten, etc., which impacts the body and causes severe or mild damage to the organs.
It can also be due to weak blood and qi; poor nourishment of the bones and muscles, causing loose joints and easy dislocation. For example, opening the mouth wide and dislocating the lower jaw is due to weak qi not being able to hold the joints tightly.
2. DIAGNOSIS OF DISLOCATION
2.1. According to YHHĐ:
To diagnose dislocation must be based on the following 3 factors:
- Medical history , carefully asking about the mechanism of injury and the patient's age.
- Clinical signs
Pain, swelling, loss of function. May be accompanied by diffuse numbness if there is nerve compression.
Joint deformity
Empty joint socket sign: touching the joint socket, no bone head is felt, only seen in complete dislocation.
Spring sign: make passive movement in the opposite direction to the deformation, when released the limb bounces back to the deformed position.
- Image study:
X-ray of the joint taken in 2 straight and oblique positions, helps diagnose dislocation and see if there is a fracture.
MRI is useful for evaluating injuries to ligaments, tendons, and soft tissues around joints.
CT-Scan helps identify cases of dislocation with intra-articular fractures.
2.2. According to Oriental Medicine:
In the context of trauma, if the injury manifests in the joints, skin, and muscles, it is called External injury; but if the illness is severe or lasts for a long time and affects the internal organs and blood, it is called Internal injury: “If the limbs and body are injured on the outside, the blood and energy are injured on the inside, the protective and nourishing parts are not in harmony with each other, and the internal organs are therefore not in harmony…” (Weak category). Thus, to dialectically discuss treatment, TCM also relies on the four diagnoses to examine and identify symptoms, including:
2.2.1. Dialectics:
- Qi stagnation - blood stasis
- Blood deficiency
- Kidney failure
2.2.2. Treatment:
Use topical medication for each case. Oral medication: use the following methods:
- Promotes blood circulation to treat stagnant blood and qi.
- Replenish blood and qi if there is blood and qi deficiency.
- Nourish the Liver and Kidney if the Liver and Kidney are weak.
3. TREATMENT:
3.1. Principles of treatment of dislocation:
The general principles for treating dislocations are: Early reduction - Immobilization - Exercise.
- Before manipulation, it is necessary to ensure good anesthesia to avoid causing pain to the patient. The level of pain relief, anesthesia or sedation depends on the position of the joint that needs to be manipulated. For example, manipulation of a dislocated finger joint only requires local anesthesia, but manipulation of the hip joint usually requires anesthesia.
- After correction, a clinical examination and X-ray must be performed to check.
- Immobilization time depends on each joint and type of dislocation. Evaluation criteria are based on healing of large joint capsule injuries and restoration of joint function.
- For old dislocations, fractures, ligament ruptures... surgical intervention is required.
3.2. Treatment according to modern medicine:
3.2.1. Correction of dislocation: Depending on the location of the dislocation, there are different correction methods.
3.2.1.1. TEMPOROMANDIBULAR JOINT DISLOCATION
The temporomandibular joint is the only movable joint in the skull and face and is a biconvex joint. The joint is composed of the articular surface of the temporomandibular bone, the articular surface of the mandible, and an articular disc. It performs three basic movements: lowering and raising the mandible, moving the mandible to the side, and moving the mandible forward and backward.
Often encountered is the anterior dislocation: the head of the lower jaw, instead of being below the temporomandibular joint, is located in front of the joint, so it is blocked there, unable to close the mouth.
Reason:
- Direct or indirect trauma affecting the lower jaw bone.
- Open your mouth too wide (yawn, laugh…)
Clinical signs: The patient is in pain and cannot close his mouth.
Treatment:
- Hippocratic technique:
Before performing, muscle relaxants and low or medium doses of sedatives should be given to reduce pain, make it easier to perform, and keep the patient alert and cooperative.
The patient sits comfortably on a chair, knees and feet touching each other. The doctor stands in front of the patient.
Place two pieces of gauze on the chewing surfaces of the two groups of lower molars on both sides (right and left).
Press your thumb down on the chewing surface of the lower jaw on the dislocated side (or both sides if dislocated on both sides) in a downward and backward direction actively, continuously, persistently, once is best. When you feel the lower jaw loosen and move easily, the jaw bone is back in place.
Let the patient rest, limit talking and opening the mouth.
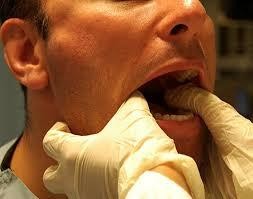
Figure 1. Hippocratic technique
- Facial correction techniques:
Based on the clinical basis that when the joint is dislocated, the parrot's beak can be easily felt just below the body of the zygomatic bone to perform this technique.
The patient sits on a chair, the doctor stands in front of the patient.
On the dislocated side, the doctor places the thumb right on the anterior edge of the coronoid process, the remaining fingers rest on the mastoid process; on the healthy side, the thumb will be placed on the body of the zygomatic bone, the remaining fingers hug the angle of the jaw. Perform correction by rotating the lower jaw to the dislocated side, by using 4 fingers to push the angle of the healthy side of the jaw forward (the thumb rests on the body of the zygomatic bone to bear the force), and at the same time on the dislocated side, the thumb pushes the coronoid process back (the remaining fingers rest on the mastoid process to bear the force).
3.2.1.2. ACROCLADULAR JOINT DISLOCATION
The acromioclavicular joint is a semi-movable joint that connects the lateral end of the clavicle to the acromion of the shoulder.
Cause: Fall or impact from behind or above the shoulder blade.
Clinical signs: Based on clinical manifestations, acromioclavicular dislocation is divided into 4 types as follows:
- Type I: swelling, soft to the touch, no palpable bone head displacement
- Type II: severe pain, early examination can see the clavicle head slide slightly upward, passive shoulder movement causes pain in the joint, grasping the middle of the clavicle to pull and push in the front-back direction while holding the shoulder still can see the clavicle head move slightly.
- Type III: complete dislocation, the arm is closed to the body and pulled up to relieve pain, the shoulder is slightly lowered, the clavicle is raised, any movement of the arm causes pain, especially the arm extension. The clavicle can move in both directions up - down and front - back.
- Type IV: has all the signs as type III, plus: the head of the clavicle is deviated backwards due to the contraction of the trapezius muscle, there is a bulge like a "button" in the trapezius muscle, and shoulder movement is very painful.
- Type V: is an amplified symptom of type III, the clavicle head is prominent and the skin is lifted (due to the arm being displaced downward). There may be neurological symptoms due to the arm being lowered too much, compressing the brachial plexus.
There is a “piano key” sign: the acromioclavicular joint is raised, when you press your finger in, the raised area disappears, when you remove your finger, it rises again, due to a rupture of the acromioclavicular ligament and coracoclavicular ligament.
Treatment:
With type I and II, the joint ligaments are intact, the bone ends are not displaced, so medical treatment is possible. Wear a splint to immobilize the arm for 10-14 days or until symptoms subside. Practice functional joint movement soon after removing the splint. Avoid strenuous movements for 8-12 weeks to allow the ligaments to fully recover.
Surgery is indicated for types III, IV, V and type II with complications (arthritis, re-dislocation...). After surgery, a brace must be worn for 1-2 weeks.
3.2.2. Drug treatment :
After joint manipulation, the patient can use regular pain relievers or oral or topical anti-inflammatory pain relievers.
3.3. According to Oriental Medicine:
Because the disease can manifest as external and internal injuries, when treating it, in addition to using manipulation and splinting techniques, attention must also be paid to internal supplements and treatment.
3.3.1. Dislocation correction:
Technique: depending on the location and type of dislocation, there are different ways to correct it. To ensure patient safety, it is necessary to make an accurate diagnosis and perform the correct technique. Traditional medicine practitioners often combine the following 8 movements:
- Palpation (diagnosis): is the first and regular step in adjustment, to see the change in position of the bone ends.
- Bone grafting: bringing bone segments together (when there is a dislocated fracture)
- Re-align: re-align the two ends of the joint as normal.
- Lift up: lift the dented bone head up to its original position.
- Grasp: is to pull back, opposite of rubbing, often combined with rubbing to clear the meridians.
- Press: press on the acupoints in the affected area to promote blood circulation, reduce swelling, and relieve pain.
- Rub: rub the stagnant area to dissolve the stagnant blood.
Orthopedic tools: The book Y Tong Kim Giam describes 10 types: cloth bandages (khoa liem), tapping sticks (chan dinh), buffalo leather splints (phi kien), handrails (phan sach), bricks for support (diet chuyen), wooden back braces (thong moc), pressing rods (yen tru), bamboo blinds for splinting (truc liem), wooden splints (sam ly), bamboo rings for knee compression (bao tat). These tools are now replaced by similar but much more convenient and effective types: slings, plaster splints, external fixators...
3.3.2. Combination drug treatment:
The use of drugs in the treatment of dislocations and trauma in general is also very diverse, especially folk experiences, including both internal and external medications. Here are some recipes based on experiences collected from books:
Topical:
- Rubbing alcohol (Nam y nghiem phuong): Sinh ma tien, Sinh aconite, Huyet giac, Dai an, Camphor, Moc duoc, Dia lien, Nhu huong, Nhu huong, Nhuc cinnamon, Can khương, each 12g, soaked in 1000ml of 90 0 alcohol using the soaking method. Effect: disperses blood stasis, reduces swelling, relieves pain. Do not apply on open wounds.
- High-grade medicine : San ling, Nga truật, Safflower, Quy vy, Dien that (San qi), Sanh quan (Dai quan), Huyet kiet (Dragon's blood), Huong phu, Su moc, each 20g. Cuong huynh 4g. Grind finely, add 200g sesame oil, 40g beeswax, cook and let cool to make a paste to rub on the outside. Effect: reduce swelling, relieve pain.
- External herbal medicine: 100g of fresh sea bean leaves, purple castor oil leaves, and mulberry leaves, crushed with vinegar, applied to the wound, changed once a day. Effect: clears heat, promotes blood circulation, reduces swelling, relieves pain, and heals bones quickly.
Oral medication:
- If there is blood stasis, use “ Phuc Nguyen Hoat Huyet thang ” (Medical invention): 20g of Safflower, 8g of Safflower, 4g of Rhubarb, 12g of Qua Lau Can, 8g of Licorice, 12g of Dao Nhan, 12g of Dang Quy, 8g of Chuan Shan Jia. Treats trauma causing blood stasis.
Drug analysis:
Medicine
Effect | |
Saffron | Heat-clearing, liver-clearing and pain-relieving |
Rose | Promotes blood circulation, removes blood stasis, and clears the meridians. |
Peach kernel | Blood stasis, antiseptic, digestive |
Rhubarb | Blood circulation, blood stasis, hemostasis |
Through the long | Throat benefits, clears up ulcers and toxins |
Angelica | Nourish blood, activate blood circulation |
Maybe you are interested!
-
 Investment Situation in Non-Credit Services at Saigon Commercial Joint Stock Bank in the Period of 2015-2019
Investment Situation in Non-Credit Services at Saigon Commercial Joint Stock Bank in the Period of 2015-2019 -
 Assessing the level of satisfaction of individual customers with savings deposit services at Saigon Commercial Joint Stock Bank SCB - Ninh Kieu Branch - 13
Assessing the level of satisfaction of individual customers with savings deposit services at Saigon Commercial Joint Stock Bank SCB - Ninh Kieu Branch - 13 -
 Classification Table of Overdue Debt Ratio by Collateral of Seabank
Classification Table of Overdue Debt Ratio by Collateral of Seabank -
 Introduction to Saigon Thuong Tin Commercial Joint Stock Bank (Sacombank)
Introduction to Saigon Thuong Tin Commercial Joint Stock Bank (Sacombank) -
 Classification of the Convenience of 3 Types of Tourism
Classification of the Convenience of 3 Types of Tourism





