Recovery
Stomach-ache
VTM
Maybe you are interested!
-
 Research on the application of endoscopic ultrasound in the diagnosis of chronic pancreatitis - 2
Research on the application of endoscopic ultrasound in the diagnosis of chronic pancreatitis - 2 -
 Epidemiological, molecular biological, clinical, paraclinical characteristics and factors affecting the effectiveness of treatment of chronic hepatitis B virus with antiviral drugs - 21
Epidemiological, molecular biological, clinical, paraclinical characteristics and factors affecting the effectiveness of treatment of chronic hepatitis B virus with antiviral drugs - 21 -
 The relationship between BMI and mortality and readmission in chronic heart failure patients treated as outpatients at Vietnam Heart Institute - 2
The relationship between BMI and mortality and readmission in chronic heart failure patients treated as outpatients at Vietnam Heart Institute - 2 -
 Current Status of Mother-to-Child HBV Transmission in Pregnant Women with Chronic HBV Visiting and Managing Pregnancy at Hai Phong Obstetrics and Gynecology Hospital in 2017-
Current Status of Mother-to-Child HBV Transmission in Pregnant Women with Chronic HBV Visiting and Managing Pregnancy at Hai Phong Obstetrics and Gynecology Hospital in 2017- -
 Cost-effectiveness study of nilotinib versus imatinib in the treatment of chronic myeloid leukemia in Vietnam - 14
Cost-effectiveness study of nilotinib versus imatinib in the treatment of chronic myeloid leukemia in Vietnam - 14
early
Endocrine and exocrine function

Latent inflammation
Compensation
Forward
Decompensation
Parenchymal changes - pancreatic duct dilatation
Pancreatic stones
Dilated main pancreatic duct - atrophy
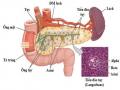
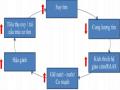
Figure 1.7. Clinical course of chronic pancreatitis
(Source: Shimosegawa T, The Tohoku Journal of Experimental Medicine, 2019) [117]
Diagnosis of early-stage chronic pancreatitis is mainly based on changes in imaging tests and tests to evaluate pancreatic exocrine function. For tests to evaluate exocrine dysfunction, indirect tests are of little value in diagnosing early-stage chronic pancreatitis. There are only direct tests based on direct assessment of pancreatic enzymes and bicarbonate in duodenal fluid after stimulating the pancreas with secretin and cholecystokinin. Direct tests are invasive, expensive and not widely used, only applicable to large centers. Direct tests have high sensitivity for moderate or severe cases of chronic pancreatitis, but for early-stage chronic pancreatitis, it is only 70-75% [45].
Japan is a pioneer in proposing the concept of diagnosing early stage chronic pancreatitis. In 1971, the Japanese Gastroenterology Society published the first diagnostic criteria for chronic pancreatitis. In 1983, the Japanese Gastroenterology Society proposed clinical diagnostic criteria for chronic pancreatitis including 5 criteria:
(1) pancreatic lesions on histopathology, (2) pancreatic calcification, (3) exocrine dysfunction, (4) main pancreatic duct stenosis on imaging, (5) epigastric pain and/or persistent elevation of pancreatic enzymes. The concept of early chronic pancreatitis has been proposed but not accepted due to lack of consensus among authors in Europe. In 1995, the Japan Pancreatic Society completed clinical diagnostic criteria based on a combination of imaging tests and pancreatic exocrine function tests. Then, the Japan Pancreatic Society continued to publish new criteria for diagnosing chronic pancreatitis in 2010, which is the first criterion for diagnosing early chronic pancreatitis in the world based on clinical symptoms, biochemical tests, risk factors and small pancreatic changes on imaging.
Japanese diagnostic criteria for early stage chronic pancreatitis:
Early stage chronic pancreatitis is diagnosed when there are at least two clinical signs and lesions on imaging studies.
Clinical and paraclinical signs
- Recurrent epigastric pain
- Abnormal pancreatic enzymes in serum or urine
- Abnormal pancreatic exocrine function
- Continuously use alcohol about 80g/day or equivalent. Image signs:
- Has two of the following seven signs but must have any of the signs from
(1) to (4), these signs were detected on endoscopic ultrasound.
(1) Honeycomb lobe lesions
(2) Non-honeycomb lesions
(3) The amplified note has no shadow.
(4) Back-noise free amplifier range
(5) Pancreatic cyst
(6) Dilated pancreatic duct
(7) Increased echogenicity of the pancreatic duct
- Dilation of more than 3 pancreatic ducts on endoscopic retrograde cholangiopancreatography [65], [116], [136].
The diagnostic criteria for early chronic pancreatitis are irregular dilatation of more than 3 pancreatic ducts, but because ERCP is an invasive procedure with many complications, EUS is recommended as the first test in the diagnosis of early chronic pancreatitis [117]. Currently, the diagnosis of early chronic pancreatitis is still controversial and needs to be based on many factors such as suggestive clinical signs, risk factors and high-resolution imaging tests [142]. The clinical symptoms of chronic pancreatitis are mainly epigastric pain, but this symptom is also not constant. Wilcox's study showed that 81 patients (15.6%) with chronic pancreatitis had obvious lesions on imaging tests and did not have abdominal pain [138]. Routine imaging tests such as transabdominal ultrasound and computed tomography have low sensitivity in diagnosing early chronic pancreatitis and are only valuable in the late stage. Computed tomography is a routine imaging test in the examination of pancreatic lesions, however, the sensitivity ranges from 60% - 95% and the sensitivity is higher for late stage chronic pancreatitis, while in early stage chronic pancreatitis, computed tomography has a relatively low sensitivity. With the advent of magnetic resonance imaging, it has been shown to be more valuable than computed tomography in the diagnosis of chronic pancreatitis, but computed tomography is still recommended in cases of monitoring complications.
Endoscopic ultrasound has the advantage of almost direct access to the pancreas, has high resolution, so it can examine small changes in the pancreatic parenchyma and pancreatic duct, so endoscopic ultrasound is valuable in the early diagnosis of chronic pancreatitis. Early diagnosis of chronic pancreatitis helps prevent progression to chronic pancreatitis. According to Sheel's retrospective study, out of 40 patients with small changes on endoscopic ultrasound who were re-examined after 3 years, 12 patients progressed to chronic pancreatitis.
Of these, 8 patients (67%) continued to drink alcohol heavily and 10 patients (83%) continued to smoke heavily. A large proportion of patients did not progress to chronic pancreatitis when they did not smoke or drink alcohol heavily [115]. Author Natalya concluded that stopping smoking and alcohol abuse would reduce the progression from early chronic pancreatitis to chronic pancreatitis [94].
Studies suggest performing endoscopic ultrasound in patients with suspected early chronic pancreatitis with the following risk factors:
- Male
- Average age 65 years old
- Smoke a lot
- Drink a lot of alcohol
- Recurrent acute pancreatitis of unknown cause
- Abdominal pain of unknown origin is thought to originate from the pancreas, especially in patients with a history of heavy alcohol consumption.
- Unexplained weight loss
- Prolonged diarrhea of unknown cause
- Abnormalities on non-invasive imaging studies (CT with dilated main pancreatic duct or suspected pancreatic stones)
- Diabetes in patients with no family history [56].
Early diagnosis of chronic pancreatitis helps limit progression to chronic pancreatitis, helps guide treatment, limits complications and controls the cause, of which alcohol is the leading cause. Therefore, endoscopic ultrasound should be indicated in cases with suggestive clinical symptoms or in patients with risk factors.
1.6. RELATED STUDIES TO THE RESEARCH TOPIC
Since 1788, chronic pancreatitis was first described by author Thomas Cawley and since then there have been thousands of studies related to it.
This disease has been reported but its pathogenesis, clinical features, diagnosis and treatment remain unclear.
1.6.1. Foreign studies
Kwon's study (2016) on 170 normal people and 150 patients with calcified chronic pancreatitis, amylase concentration was 48.1 ± 13.2 and 34.8 ± 17.2 U/L with a difference of p < 0.001 and lipase concentration was 26.4 ± 11.3 and 16.3 ± 11.2 U/L with a difference of p < 0.001. The authors concluded that low pancreatic enzyme concentration is valuable in diagnosing chronic pancreatitis [78].
In the study of Hyoung-Chul Oh (2017), the concentrations of amylase and lipase were 47.0 (39.8 - 55.3); 25.0 (18.0 - 35.0) for the control group and 34.0 (24.5 - 35.0) for the control group, respectively.
- 49.0); 19.0 (9.0 - 30.0) for non-calcified chronic pancreatitis group and 30.0 (20.0
- 40.8); 10.0 (3.0 - 19.0) for the group of chronic pancreatitis with calcification; with the amylase cut-off point of 40 U/L and lipase of 20 U/L having diagnostic value for the group of chronic pancreatitis without calcification; the amylase cut-off point of 38 U/L and lipase of 15 U/L having diagnostic value for the group of chronic pancreatitis with calcification. With the concentration of amylase < 40 and lipase < 20 U/L in the diagnosis of chronic pancreatitis without calcification, the sensitivity, specificity, positive predictive value and negative predictive value were 37.4%; 88.8%; 66.1%; 70.9%, respectively, and the author Hyoung Chul Oh concluded that the concentration of amylase or lipase below normal has high specificity in the diagnosis of chronic pancreatitis [96].
Choueiri's (2010) study showed that computed tomography has a diagnostic sensitivity of 60-95% for late-stage chronic pancreatitis, but diagnosing early-stage chronic pancreatitis is very difficult [36].
According to Busireddy's study (2014), computed tomography is only valuable in diagnosing changes in the pancreatic duct and pancreatic parenchyma in the late stages, while in the early stages, computed tomography is of little value [30].
Issa's study (2017) on 3460 patients showed that computed tomography had a sensitivity of 75% and a specificity of 91% in diagnosing chronic pancreatitis [63].
Issa's study (2017) collected statistics from 288 pancreaticobiliary specialists and agreed that the value of computed tomography in examining pancreatic head hypertrophy was 59%, pancreatic pseudocysts were 55%, pancreatic stones were 75%, and peripancreatic fat infiltration was 68% [64].
Kamat's study (2019) found that the rate of pancreatic duct dilation was 68%, pancreatic parenchymal atrophy was 54%, pancreatic duct stones/parenchymal stones were 50%, and peripancreatic fat infiltration was 16% in cases of chronic pancreatitis detected on computed tomography [72].
Wallace's (2001) study evaluated 45 cases, including 33 clinically suspected cases of chronic pancreatitis and 12 unsuspected cases, examined by 11 experienced endosonographers and found high agreement in the description of pancreatic duct dilatation and honeycomb lesions. The authors concluded that endoscopic ultrasound, despite its limitations, is a more valuable diagnostic tool than ERCP, computed tomography, and other clinical tests [130].
Kahl's study (2002) on 130 patients randomly surveyed or suspected of chronic pancreatitis had 38 normal cases on ERCP but suspicious on EUS, continued follow-up after an average of 18 months, 22 patients were diagnosed with chronic pancreatitis on ERCP, accounting for 68.8% [71].
According to Stevens (2010), the study on the combination of endoscopic-assisted functional testing and endoscopic ultrasound has high specificity and sensitivity in diagnosing early stage chronic pancreatitis. This study showed that the positive predictive value in pancreatic stone examination was 90%, found pancreatic branch ducts in 76%, pancreatic cysts in 75%, dilated main pancreatic duct, irregular main pancreatic duct wall, honeycomb lesions (58-66%) and hyperechoic nodules, hyperechoic bands, hyperechoic pancreatic duct wall (47-51%) [122].
Jimeno Ayllon's study (2011) found no difference between the Rosemont criteria and the conventional criteria when taking the cutoff of 4 criteria, but there was a difference in 27.66% of cases with less than 4 criteria diagnosed with suspected chronic pancreatitis according to the Rosemont criteria [68].
Le Blant's (2014) longitudinal study of 226 patients and 100 patients with surgical indications showed a correlation between endoscopic ultrasound and histopathology, these criteria were honeycomb lesions, hyperechoic nodules with dorsal shadowing, dilated main pancreatic duct, abnormal main pancreatic duct, dilated branch pancreatic duct. The author confirmed the value of pancreatic duct change criteria in the diagnosis of chronic pancreatitis [82].
D'Souza's study (2015) compared the conventional standard and the Rosemont standard. When choosing a cutoff point of 3 criteria, the rate of chronic pancreatitis diagnosed by the conventional standard was higher than the Rosemont standard, but when choosing a cutoff point of 5 criteria, it showed a close correlation with the Rosemont standard in diagnosing chronic pancreatitis [43].
In a retrospective study by Sheel (2018), of 40 patients with minor changes on endoscopic ultrasound who were re-examined after 3 years, 12 patients progressed to chronic pancreatitis, of which 8 patients (67%) continued to drink alcohol heavily and 10 patients (83%) continued to smoke heavily. A large proportion of patients did not progress to chronic pancreatitis when they did not smoke or drink alcohol heavily. The author concluded that stopping smoking and alcohol abuse would reduce the progression from early chronic pancreatitis to chronic pancreatitis [115].
1.6.2. Domestic research
Research by Pham Tien Dat (2004) on 68 patients from 2000 - 2004 at Viet Duc Hospital showed that the proportion of patients with chronic pancreatitis and pancreatic stones mainly related to alcoholism and alcohol abuse accounted for 60.29%. Pain in the epigastric region accounted for 98.5% and loose stools accounted for 41%, diabetes mellitus
The results of imaging diagnosis based on transabdominal ultrasound and computed tomography showed pancreatic stones in 36/68 cases (52.94%), pancreatic calcification in 68/60 (100%), and main pancreatic duct dilatation in 59/68 cases (86.76%) [4].
According to author Le Van Cuong, a study of 61 patients with chronic pancreatitis treated surgically at Binh Dan Hospital from 1994 to 2009, the male/female ratio was 46/15 and the average age was 37.05. Causes related to chronic pancreatitis due to alcohol accounted for 47.5% and due to tobacco 40.9%. Clinical symptoms of epigastric pain accounted for 100%, including 22 cases of pain with nausea and 25/61 cases of pain with anorexia. Characteristics of the pancreas on preoperative ultrasound included dilated main pancreatic duct in 45/61 cases, pancreatic stones with dilated main pancreatic duct in 32/61 cases, pancreatic stones with dilated common bile duct in 11/61 cases [3].
Nguyen Anh Tuan's study on 32 patients who were indicated for simple pancreatico-enterostomy surgery to treat chronic pancreatitis from 2006 to 2010 at Hospital 108 had an average age of 51.06 ± 11.3 (18-66 years old), a history of alcoholism accounting for 53.1% (250 - 750ml/day), 9.4% had a history of acute pancreatitis and 18.6% had diabetes. The prominent clinical symptoms were still pain accounting for 100%, of which severe pain accounted for 65.6%, dull but persistent pain 34.4%, pain radiating to the back accounted for 71.9% and up to 91.9% of patients had to use painkillers, weight loss accounted for 84.4%, loose stools 65%, jaundice accounted for 6.5%. Biochemical tests showed that 34.4% had mild elevation of serum amylase with the highest level of 680U/L and 12.5% had high blood bilirubin. Characteristics of pancreatic lesions before surgery assessed by ultrasound or computed tomography showed pancreatic duct dilation in 100% (with surgical indication), large pancreatic head in 31.2%, pancreatic stones in 87.5%, and pancreatic cysts in 12.5% [13].