Percentage for most variables in the study: age group, gender, time of disease onset, reason for examination, medical history, physical symptoms, paraclinical characteristics (tumor location, tumor characteristics on CT scan, GPB characteristics)...
+ Statistical inference algorithms: compare and test statistically significant differences, correlations and regressions between variables. The specific algorithms are as follows:
① : X² Test: Chi-square Test compares the difference between clinical characteristics
clinical and paraclinical, between factors related to treatment outcomes, reliability p < 0.05
② : Fisher test (when 2 cells corresponding to 50% of expected value < 5)
③ : Univariate logistic regression
④ : Univariate linear regression: Linear regression analyzes the relationship between clinical and paraclinical characteristics (time of disease onset and tumor size, exophthalmos and tumor size)
⑤ : Paired t-test (McNemar test), odds ratio (OR) to evaluate the relationship between clinical and paraclinical characteristics, factors related to treatment outcomes, 95% confidence interval CI
⑥ : Paired-Samples T Test
⑦ : Log rank check
⑧ : Multivariate Cox regression
- Research errors: include sampling errors (random or non-random) and information errors. The solution is to choose a large enough sample size and collect complete and accurate patient information.
2.4. Research ethics
- The patient agrees to participate in the study and to have his/her personal photo used in the study. All pre-treatment agreements are committed in writing with the patient's signature.
- Information collected is for research purposes only and ensures patient confidentiality.
- Patients are provided with full necessary information about the research as well as the rights to care and treatment when participating in the research.
- The study was conducted with the approval of the Board of Directors of the Central Eye Hospital.
- The study was approved by the hospital's scientific and technical council and the thesis evaluation board of Hanoi Medical University.
CHAPTER 3
RESEARCH RESULTS
3.1. Clinical and paraclinical characteristics of lacrimal gland tumors
We examined and treated 108 patients with lacrimal gland tumors, with a mean follow-up period of 30.7 ± 12.46 months (0.25 – 50 months). The study results are presented as follows:
3.1.1. Characteristics of patients with lacrimal gland tumors
3.1.1.1. Characteristics by age and age group
The average age of lacrimal gland tumors was 52.9 ± 15.3 (7 – 96 years old). The benign mixed lacrimal gland tumor group was 47.2 ± 14.1 (18 – 72 years old), the lacrimal gland carcinoma group was 48.4 ± 10.2 (27 – 68 years old). The lymphoma group had an older average age, specifically the lymphoid hyperplasia group was 54.3 ± 17.5 (7 – 96 years old), and the malignant lymphoma group was 56.4 ± 13.6 (14 – 81 years old).
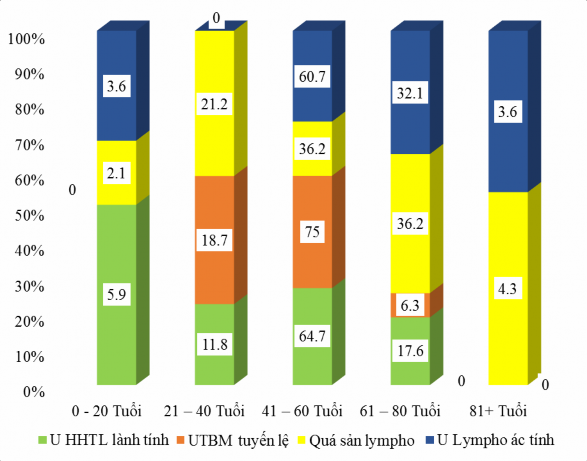
Figure 3.1. Age distribution of lacrimal gland tumors
According to chart 3.1, the most common age group for lacrimal gland tumors is (41 – 60 years old).
In general, all lacrimal gland tumor subtypes are also common in this age group.
3.1.1.2. Gender characteristics
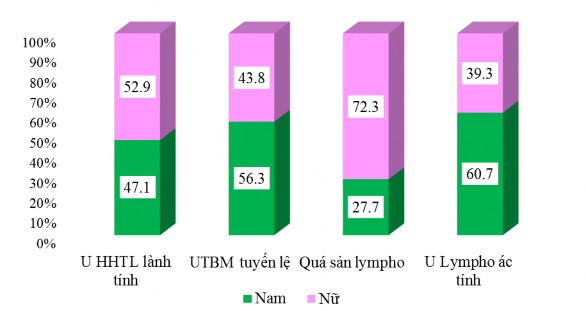
Figure 3.2. Patient characteristics by gender
In the benign mixed lacrimal gland tumor group, the female predominance was 52.9% and in the lacrimal gland carcinoma group, the male predominance was 56.3%. In the lymphoid hyperplasia group, the female predominance was 72.3% and in the malignant lymphoma group, the male predominance was 60.7%.
3.1.2. Clinical characteristics of patients with lacrimal gland tumors
3.1.2.1. Characteristics according to the affected eye
In 108 patients with lacrimal gland tumors, 36.1% of patients had bilateral disease and 63.9% of patients had unilateral disease (35.2% left eye and 28.7% right eye). The group of mixed benign lacrimal gland tumors and carcinomas had only one eye, no case of bilateral disease. The group of lymphoid hyperplasia and malignant lymphoma had the rate of bilateral disease in 61.7% and 35.7%, respectively.
3.1.2.2. Reason for medical examination
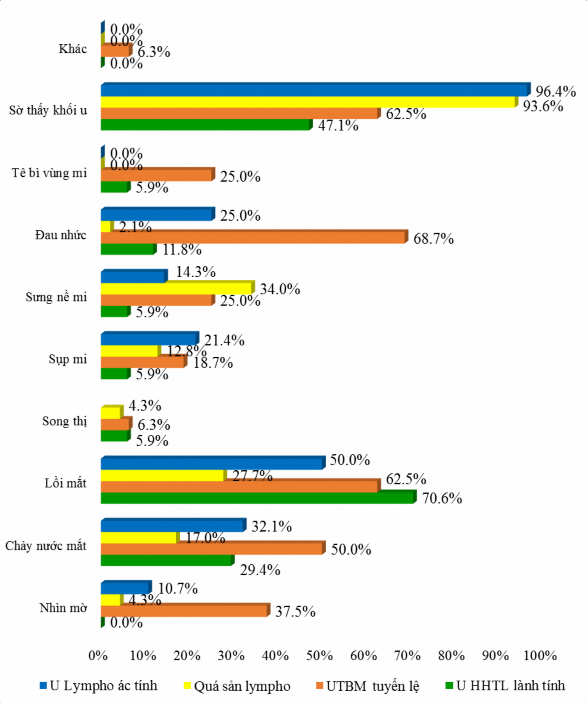
Figure 3.3. Distribution of reasons for medical examination
The most common reasons for medical examination in the benign mixed lacrimal gland tumor group were proptosis and palpable mass. Pain was most common in the carcinoma group, accounting for 68.7%. The main reason for medical examination in the lymphoid lesion group was palpable mass.
3.1.2.3. Time from onset of symptoms to medical examination
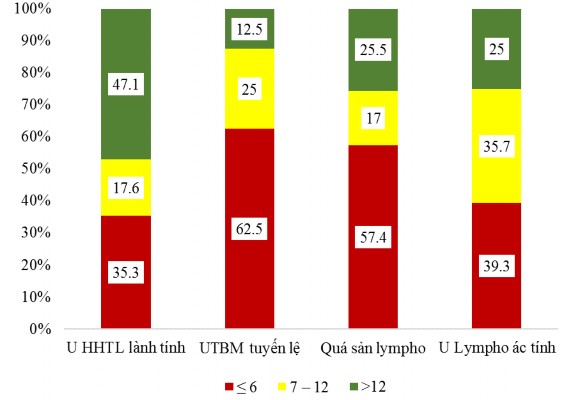
Figure 3.4. Time group from symptom onset to medical examination
The average time from the onset of symptoms to the examination of lacrimal gland tumors was 14.43 months (1 - 84 months). The time of onset of disease for the groups of benign mixed lacrimal gland tumors, lacrimal gland carcinoma, lymphoid hyperplasia, and malignant lymphoma was 16.12 months (2 - 36 months), 7.88 months (1 - 36 months), 15.83 months (1 - 84 months), 14.79 months (1 - 48 months), respectively. In particular, we saw that the lacrimal gland carcinoma group had the shortest time of onset of disease.
The benign mixed lacrimal gland tumor and lymphoid hyperplasia groups had a duration of disease symptoms >12 months, respectively 47.1% and 25.5%. The lacrimal gland carcinoma and malignant lymphoma groups had a duration of disease symptoms ≤ 6 months, respectively 62.5% and 39.3%.
3.1.2.4. Relevant medical history
Table 3.1. Relevant medical history
Lacrimal gland tumor
Medical history
U HHTL benign (n = 17) | UTBM gland (n = 16) | Lymphocytic hyperplasia (n = 47) | Malignant lymphoma (n = 28) | Total (n = 108) | |||||||
n | % | n | % | n | % | n | % | n | % | ||
Whole body manifestations | Are not | 17 | 100 | 16 | 100 | 46 | 97.9 | 24 | 85.7 | 103 | 95.4 |
Have | 0 | 0.0 | 0 | 0.0 | 1 | 2.1 | 4 | 14.3 | 5 | 4.6 | |
Relevant medical history | Are not | 15 | 88.2 | 8 | 50.0 | 34 | 72.3 | 19 | 67.9 | 76 | 70.4 |
Have | 2 | 11.8 | 8 | 50.0 | 13 | 27.7 | 9 | 32.1 | 32 | 29.6 | |
Treatment history | Are not | 14 | 82.4 | 8 | 50.0 | 34 | 72.3 | 19 | 67.9 | 75 | 69.4 |
Have | 3 | 17.6 | 8 | 50.0 | 13 | 27.7 | 9 | 32.1 | 33 | 30.6 | |
Maybe you are interested!
-
 Study on Some Clinical and Paraclinical Features of Appendiceal Abscess
Study on Some Clinical and Paraclinical Features of Appendiceal Abscess -
 Correlation Between Some Clinical and Paraclinical Factors With Asmih Reduction
Correlation Between Some Clinical and Paraclinical Factors With Asmih Reduction -
 Epidemiological, molecular biological, clinical, paraclinical characteristics and factors affecting the effectiveness of treatment of chronic hepatitis B virus with antiviral drugs - 21
Epidemiological, molecular biological, clinical, paraclinical characteristics and factors affecting the effectiveness of treatment of chronic hepatitis B virus with antiviral drugs - 21 -
 Clinical features, endoscopic images of laryngoscopy and pathological anatomy of vocal cord cysts - 7
Clinical features, endoscopic images of laryngoscopy and pathological anatomy of vocal cord cysts - 7 -
 Clinical and Paraclinical Characteristics of Pregnant Women with Placenta Previa at Hanoi Obstetrics and Gynecology Hospital
Clinical and Paraclinical Characteristics of Pregnant Women with Placenta Previa at Hanoi Obstetrics and Gynecology Hospital
With general lacrimal gland tumors, the majority have no systemic changes (95.4%), only 4.6% have systemic changes such as lymph nodes in the neck, groin, and armpits. The related medical history accounts for 29.6%, including a history of patients being diagnosed and treated for mixed lacrimal gland tumor, lacrimal gland lymphoid hyperplasia, lacrimal gland carcinoma, or malignant lymphoma. The treatment history accounts for 30.6%, including a history of patients having undergone tumor resection, tumor biopsy, chemotherapy, radiotherapy, or corticosteroid use. The lacrimal gland carcinoma group has a related medical history and a treatment history of 50%. The malignant lymphoma group has a related medical history and a treatment history of 32.1%. The common feature of the lymphoma group is that there are lymph nodes scattered throughout the body, which have been diagnosed and treated by biopsy. Some patients have systemic lymphoma.
In the benign mixed lacrimal gland tumor group, no patient had any related systemic problems. Two patients had a history of previous surgery for a lacrimal gland tumor, of which one patient was diagnosed with a right orbital lipoma and one patient had a lacrimal gland tumor removed 18 months before admission but the tumor was unknown.
No patient with adenoid cystic carcinoma had systemic changes. Eight patients had a history of related diseases and had been treated. One patient had undergone surgery to remove a tumor in the lacrimal gland area 5 years before admission at the provincial hospital, but the tumor was not clearly diagnosed. One patient was diagnosed with adenoid cystic carcinoma 3 years before admission and had received 25 radiation treatments at the provincial hospital. Three patients were diagnosed with adenoid cystic carcinoma and had undergone surgery, radiation, and chemotherapy. One patient had undergone a tumor removal in the lacrimal gland area 17 years before admission but had not been diagnosed with a tumor and had not received any treatment. One patient had a tumor removed 3 years before admission and was diagnosed with a mixed lacrimal gland tumor with malignant tendencies. One patient had angle-closure glaucoma and had undergone 5 surgeries and had frequent eye pain.
In the lymphoid hyperplasia group, 1/47 patients had systemic disease and 13/47 patients had a history of related diseases and treatments, including 1 patient with lymph nodes in the armpit and groin, 10 patients had undergone surgical biopsy to remove the tumor, diagnosed with lymphoid hyperplasia and treated with corticosteroids, 2 patients had had a tumor removed in the lacrimal gland area, unknown diagnosis and no treatment, 4 patients had a tumor removed, unknown tumor, treated with corticosteroids with relief.
The malignant lymphoma group had 4/28 patients with systemic disease and 9/28 patients with a history of related diseases and treatment, including 1 patient with left lung cancer 1 year before admission, no treatment, 2 patients were diagnosed and had lacrimal gland tumors removed 4 years before admission, no additional treatment, 1 patient was diagnosed with malignant lymphoma, received chemotherapy at the Central Hematology Hospital, 1 patient had subclavian lymph nodes, had a history of kidney cancer 6 years before admission, was being treated at the K hospital, had lymph node tuberculosis 4 years before admission, was being treated with chemotherapy and radiotherapy, 3 patients had a history of lacrimal gland tumor biopsy and were diagnosed with lymphoid hyperplasia (including 2 patients who did not receive any treatment and 1 patient who received multiple courses of corticosteroids), 1 patient had thyroid cancer and received radiotherapy.
3.1.2.5. Clinical examination characteristics
- Maximum corrected vision
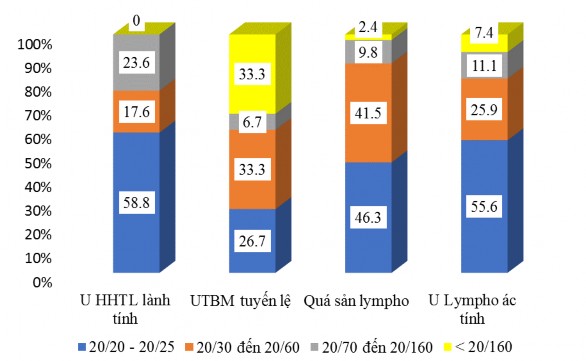
Figure 3.5. Maximum corrected visual acuity ratio in groups
The benign mixed lacrimal gland tumor group had normal vision in 58.8% of patients, and no patients had severe vision loss. The lacrimal gland carcinoma group had 33.3% severe vision loss. The malignant lymphoma hyperplasia group had 2.4% severe vision loss. The malignant lymphoma group had severe vision loss in 7.4%.
- Intraocular pressure
Table 3.2. Average intraocular pressure in patients with lacrimal gland tumors
Intraocular pressure
Lacrimal gland tumor
Mean intraocular pressure (mmHg) | |||||
n | Medium | ± SD | Minimum | Maximum | |
Benign HHTL | 17 | 17.7 | 1.3 | 16 | 22 |
Lacrimal Gland Tumor | 14 | 17.6 | 1 | 16 | 19 |
Lymphocytic hyperplasia | 47 | 17 | 1.4 | 16 | 24 |
Malignant lymphoma | 28 | 17.9 | 1.2 | 16 | 22 |
Total | 106* | 17.4 | 1.3 | 16 | 24 |
*: There were 2 patients without intraocular pressure measurement because 1 patient had previous orbital tissue dredging, 1 patient had corneal ulcer.
Patients in the lacrimal gland tumor groups did not have increased intraocular pressure.





