The Framingham criteria and the ESC criteria are two widely used diagnostic criteria for heart failure. The Framingham criteria are often used in community surveys. The ESC criteria have clinical practical value.
Clinically, the signs/symptoms of heart failure can vary from patient to patient and can be difficult to detect due to comorbidities such as diabetes, lung diseases, endocrine diseases, etc. It is necessary to carefully assess the patient's condition and perform the necessary tests to assess whether the signs/symptoms are due to heart disease or caused by comorbidities.
Table 1.5 Sensitivity and specificity of symptoms/signs of heart failure
Clinical signs
Sensitivity (%) | Specificity (%) | |
Shortness of breath | 66 | 52 |
Difficulty breathing when lying down | 21 | 81 |
Paroxysmal nocturnal dyspnea | 33 | 76 |
History of edema | 23 | 80 |
Rapid heart rate | 7 | 99 |
Lung Rales | 13 | 91 |
Edema on clinical examination | 10 | 93 |
Heart sound T3 | 31 | 95 |
Increased jugular venous pressure | 10 | 97 |
Maybe you are interested!
-
 Clinical and paraclinical characteristics and treatment outcomes of patients with acute liver failure at the Poison Control Center of Bach Mai Hospital in 2020 - 2021 - 10
Clinical and paraclinical characteristics and treatment outcomes of patients with acute liver failure at the Poison Control Center of Bach Mai Hospital in 2020 - 2021 - 10 -
 Epidemiological, molecular biological, clinical, paraclinical characteristics and factors affecting the effectiveness of treatment of chronic hepatitis B virus with antiviral drugs - 21
Epidemiological, molecular biological, clinical, paraclinical characteristics and factors affecting the effectiveness of treatment of chronic hepatitis B virus with antiviral drugs - 21 -
 Clinical and Paraclinical Characteristics of Pregnant Women with Placenta Previa at Hanoi Obstetrics and Gynecology Hospital
Clinical and Paraclinical Characteristics of Pregnant Women with Placenta Previa at Hanoi Obstetrics and Gynecology Hospital -
 Study on clinical and paraclinical characteristics of dengue fever at E Hospital in 2021 - 1
Study on clinical and paraclinical characteristics of dengue fever at E Hospital in 2021 - 1 -
 Correlation of Some Clinical and Paraclinical Characteristics with Risk Stratification According to Who/ish Score
Correlation of Some Clinical and Paraclinical Characteristics with Risk Stratification According to Who/ish Score
Once heart failure has been diagnosed, the underlying cause of the heart failure must be determined and treated appropriately. There are a number of tests that can more accurately assess the nature of the heart dysfunction and provide potential factors for treatment planning. Some tests can also provide prognostic information that will help in the choice of invasive/noninvasive management strategies. These tests include:
1. Stress test:
- Often to check for coronary artery disease
- Exercise metabolic tests are also used to aid in prognosis and to differentiate between pulmonary and cardiac disease – Patients with pulmonary disease will have reduced saturation levels during exercise
2. Routine tests (heart failure screening):
- Blood count: anemia can be a cause or effect of heart failure.
- Electrolytes (Na + , K + ) and Urea
- Creatinine, glomerular filtration rate.
- Thyroid function tests: hypothyroidism and hyperthyroidism can cause heart failure.
- Ferritin – hemochromatosis can be a (reversible) cause of heart failure.
- Lipid – increased blood cholesterol is often associated with the main causes of heart failure and ischemic heart disease.
- Blood glucose.
3. Rarely performed tests, usually only done when there is a suspicion of underlying disease:
- Viral titer when myocarditis is suspected.
- HIV
- Genetic testing (with consultation by geneticists).
4. Pulmonary ventilation function test:
- FVC and FEV 1 are reduced in heart failure
- Bronchodilator reversibility testing is useful in determining response to beta-adrenoreceptor blockers.
5. 24-hour Holter ECG:
- Often used in patients with arrhythmia symptoms.
1.1.5. Epidemiological situation of chronic heart failure
a. In the world
According to statistics, there are currently 26 million people in the world living with heart failure. Heart failure is still a global burden (with 1-2% of the world's population suffering from heart failure - equivalent to about 26 million people with the disease); the incidence of heart failure increases with age in both sexes, and affects 6-10% of the population over 65 years old. Although the rate of heart failure in women is relatively lower than in men, the number of heart failure cases in women accounts for about half of the total number of heart failure cases due to the higher life expectancy in women than in men [2] . In addition, heart failure is a public health problem that needs attention, not only in Europe or the US but also in the Asian region. The Southeast Asian region has a high rate of heart failure due to
This is a region with a unique socio-cultural and historical diversity and a rapidly growing population of >600 million people, the majority of whom are under 65 years of age. Statistics show that the prevalence of heart failure is increasing in low- and middle-income countries due to increasing rates of ischemic heart disease and hypertension. The prevalence of heart failure in Southeast Asia is similar to the global rate, with heart failure in 20% of hospital admissions and a 30-day readmission rate of up to 15% (approximately 8% in Malaysia, Indonesia, and Vietnam, 15% in Taiwan). In addition, the prevalence of cardiovascular disease in Southeast Asian countries is increasing due to conditions such as obesity, diabetes, hypertension, as well as changes in lifestyle [20] .
For chronic heart failure, about 50% of all inpatient cases are heart failure with reduced ejection fraction[21] , [1] . The European Society of Cardiology in 2021 published the results of a study on outpatient heart failure patients, with 60% of cases being heart failure with preserved ejection fraction, 24% of patients having mildly reduced ejection fraction, and 16% of patients having heart failure with reduced ejection fraction. About 50% of patients with heart failure are female [15] .
In the United States, according to a cohort study of over 40,000 cases, the risk of developing heart failure from age 45 to 95 increased from 30% to 42% in white men, 20% to 29% in black men, 32% to 39% in white women, and 24% to 46% in black women, respectively [22] . According to a recent study in the UK, based on data collected from electronic medical records of 1.25 million patients, the probability that an adult over 30 years of age will develop heart failure during their remaining life expectancy is 5%. For patients with hypertension (systolic blood pressure > 140mmHg), the probability is 7.8% [23] .
Causes of death in patients with heart failure are also a notable factor. According to a retrospective study conducted by more than 61 cardiovascular centers in the United States, published by the AHA in 2013, patients with chronic heart failure had a mortality rate of cardiovascular diseases accounting for 65.3% of deaths, of which the mortality rate due to heart failure accounted for 40.5% [24] . Regarding the hospitalization rate of patients with chronic heart failure, 22.7% of chronic heart failure cases required hospitalization, of which 17.2% were hospitalized due to cardiovascular problems, including 8.8% of patients hospitalized due to heart failure [24] . In the United States, heart failure is the most common cause of hospitalization for patients over 65 years old. Hospitalizations due to heart failure often require a long stay, followed by re-hospitalizations with shorter stays [25] . Study
A study published in 2000 in The BMJ found that in the UK, up to one-third of patients with heart failure were readmitted to hospital within 12 months of discharge, and in the US, the corresponding rate was within six months of discharge [25] . According to the ASIAN-HF study, in the Asia-Pacific region, for patients with heart failure with reduced ejection fraction, the 1-year mortality rate was 12%, and the 1-year hospitalization rate for heart failure was 15% [26] .
Due to population explosion, aging and increasing rates of comorbidities, it is expected that the number of patients hospitalized for heart failure may increase significantly, up to 50% in the next 25 years [15] .
b. In Vietnam
In Vietnam, although there are no official figures, it is estimated that there are about
320,000 to 1.6 million people suffer from heart failure, an estimated 1-1.5% of the population. There is little published data on the epidemiology of heart failure in Vietnam. The rate of hospitalization due to heart failure at Hanoi Heart Hospital accounts for 15% of all hospitalizations. The estimated cost of inpatient treatment for heart failure patients at Hanoi Heart Hospital is about 1000 USD per patient, while the average GDP per capita in Vietnam is 2481 USD. This shows that the economic burden of heart failure on heart failure patients in Vietnam, mainly the cost of inpatient treatment, is an important issue that needs attention [20] .
1.2. Treatment compliance status
The World Health Organization (WHO) defines "adherence" as the degree to which a person's behavior (including taking medication) is consistent with the advice of a health care professional. In particular, the term "adherence to medication" (or medication adherence) is defined as the process by which a patient uses medication in accordance with the doctor's instructions based on the prescription. This process includes: (1) initiation of treatment (initiation): starting when the patient takes the first dose of the prescription; (2) implementation of treatment instructions (implementation): followed by the patient's actions in following the instructions (such as dosage, time of use...) during the period from the first dose to the last dose; (3) discontinuation of treatment (discontinuation): ending the last dose without any doses of the prescribed medication being taken by the patient afterwards [27] .
Epidemiologically, in patients with heart failure, treatment adherence is approximately 40-80%. This variation is due to various factors that may influence the population.
studies as well as possible differences in adherence measures [28] . Poor adherence to treatment regimens is an important factor that prevents effective clinical treatment in patients with heart failure. Overall rates of adherence to diet, medication, and exercise remain below those needed to reduce morbidity and mortality from heart failure [29] . Overall, the general trend in adherence to treatment in patients with heart failure is high adherence to follow-up visits, medication use, and elimination of risk factors such as alcohol and tobacco. Meanwhile, adherence to diet and exercise is low [8] , [30] . Poor adherence to treatment in patients with heart failure contributes to increased mortality, rehospitalization, and health care costs. However, good adherence to heart failure treatment is a big challenge for patients, their families and healthcare professionals [31] . Because non-adherence to treatment is a problem caused by many factors, identifying factors and issues that affect adherence to treatment in elderly heart failure patients is essential to improve the process and quality of treatment in elderly patients with chronic heart failure.
According to the study by author Jaarsma (2013) [11] describing the status of self-care and health monitoring in heart failure patients in 15 countries on 5964 heart failure patients showed that most patients took prescribed medications, however, the rate of patients controlling their weight and exercising was still low. More than 50% of cases reported that they had a low level of exercise, less than half of cases had regular weight monitoring, and this rate varied greatly between different countries. Self-care on the basis of annual influenza vaccination and low-salt diet varied greatly between countries [11] . Multinational studies on the importance of self-care behavior in heart failure patients showed that there were large differences between countries, however, the rate of poor adherence to treatment remained significantly low regardless of the country. Studies have shown similar adherence to medication and exercise across most countries, but there is large inter-country variation in adherence to weight management, low-salt diets, and annual influenza vaccination [11] .
In Vietnam, compliance with treatment in heart failure patients is still low. In Vietnam, 37% of heart failure patients do not take medication as prescribed, 10% do not monitor symptoms, do not have regular check-ups, and more than half (52.5%) continue to eat salty foods according to the normal regimen after discharge from the hospital [32] , [33] . Meanwhile, another study on 112 heart failure patients at Hospital C - City
In Da Nang in 2019, 54.5% of cases complied with the treatment regimen. In this study, the rate of patient compliance with medication and follow-up visits was high (80%), while the rate of compliance with exercise, fluid intake reduction, and daily weighing was low (43.8%, 33.8%, and 16.1%, respectively). Factors that significantly affected compliance were also shown to include gender, education level, number of hospitalizations in the previous year, comorbidities, knowledge of heart failure, and cognitive impairment [3] .
1.3.1. Factors affecting treatment compliance in patients with chronic heart failure with reduced ejection fraction
Factors contributing to poor adherence include multiple comorbidities, clinical depression, or cognitive impairment. Educating patients about self-management skills and health care monitoring can improve quality of life, but have not been shown to have a clear impact on heart failure readmissions and mortality. Telemedicine care has been shown to improve patient adherence and significantly improve clinical outcomes [29] . Several factors have been shown to contribute to poor adherence, including inappropriate treatment strategies, side effects, depression, inadequate guidance from health care professionals, and lack of education about health care. Some patients believe that they only need to take their medications when they are sick or have symptoms, and stop taking them when they feel better. Different groups of drugs also have different levels of treatment compliance [34] . A study by author Nguyen Ba Tam on chronic heart failure patients treated as outpatients at Nam Dinh General Hospital showed that treatment compliance had a significant and positive correlation with the patient's education level, medical care support and knowledge, and depression had the largest and negative correlation with treatment compliance [33] .
In general, there are five groups of factors that can influence treatment adherence in heart failure patients: (1) factors related to patient characteristics, (2) factors related to patient medical conditions, (3) treatment-related factors, (4) factors related to the health care system, and (5) socioeconomic factors.
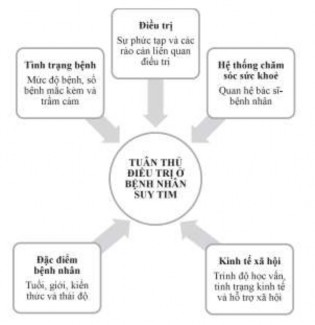
Figure 1.3 Factors that may influence treatment adherence
a. Factors related to patient characteristics
Much of the literature on adherence in heart failure patients focuses on factors related to patient characteristics. In particular, age and gender are two factors that have been examined in many studies, but the ability of these two factors to predict adherence is inconsistent across studies. In the systematic review by Oosterom-Calo et al. (2013), the number of studies indicating age as a factor in determining adherence was equal to the number of studies concluding that there was no association between age and adherence. In the group of studies that identified an association, it was shown that the older the patient, the higher the adherence [35] .
Patient knowledge may also influence treatment adherence. A study by Clark et al. (2009) demonstrated that heart failure patients with poor knowledge of drug therapy and disease progression were at high risk of mortality [36] . Many studies have shown that heart failure patients have low knowledge of their treatment. Some studies have shown that after discharge, 45% of patients did not know the names, 50% did not know the dosage, 64% did not know the number of times to use the drugs prescribed for them, and up to 82% were taking drugs that were not prescribed [10] . Because the treatment of heart failure is quite complex, patients with good knowledge will help optimize treatment adherence. However, results from two systematic reviews did not find a significant effect of knowledge level on treatment adherence in heart failure patients.
heart [35], [10] . Some studies have shown that ethnic minority patients with heart failure often have poor adherence to treatment. However, this poor adherence was not significant in some other studies [10] .
b. Factors related to the patient's medical condition
Inconsistent results have been obtained in studies examining the impact of the number of comorbidities on treatment adherence in patients with heart failure. Some studies have shown that patients with a higher number of comorbidities are less adherent to treatment; other studies have shown the opposite. Based on published data, we have not yet determined the relationship between the number of comorbidities and the level of treatment adherence in patients with heart failure [10] .
In addition, psychological barriers are also barriers to adherence. In heart failure patients, the rate of depressive symptoms is 10% in outpatients and 50% in inpatients. Heart failure patients with depressive symptoms are 3 times more likely to have poor adherence to treatment than patients without depressive symptoms [10] .
c. Factors related to treatment
Chronic heart failure with reduced ejection fraction is a public health problem with high morbidity and mortality. Despite significant advances in the treatment of heart failure with reduced ejection fraction, including SGLT2 inhibitors, Vericiguat, and percutaneous mitral valve replacement, all of which have increased the overall effectiveness of heart failure treatment. However, the morbidity and mortality of heart failure remain high, with a 5-year survival rate after hospitalization for heart failure of 25% for heart failure with reduced ejection fraction. Poor adherence to heart failure treatment regimens is an important factor in the poor treatment outcomes of patients with heart failure. In addition, nonadherence has been shown to be associated with increased all-cause mortality and hospitalization rates in patients with heart failure. In 2011, Fitzgerald and colleagues conducted a study on 557 patients with heart failure with reduced ejection fraction (Heart failure with reduced ejection fraction – EF < 50%) from many major medical centers to evaluate the impact of treatment adherence (with ACEIs/ARBs, β-blockers, and aldosterone antagonists) on the treatment effectiveness in reducing all-cause mortality and hospitalization rates in patients with heart failure. The results showed that non-adherence to treatment (defined as adherence < 80% to the treatment regimen) had statistical significance on the outcome of mortality and hospitalization rates.





