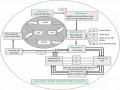
- Detect errors in the document system and actual operations of the agency, request correction.
Some typical shortcomings of rating organizations are:
- Lack of objectivity in evaluating the quality management system of established administrative agencies.
- Using incompetent assessment experts who do not fulfill their responsibilities to help administrative agencies detect errors during operations.
Maybe you are interested!
-
 Improving the Quality of Administrative Procedures and Strengthening the Direction and Management of the Heads of State Administrative Agencies at the Ministry Level
Improving the Quality of Administrative Procedures and Strengthening the Direction and Management of the Heads of State Administrative Agencies at the Ministry Level -
 High-Quality Female Human Resources Participating in Leadership and Management in the Political System Are Still Low and Unstable
High-Quality Female Human Resources Participating in Leadership and Management in the Political System Are Still Low and Unstable -
 General Assessment of the Current Situation of Public Investment Capital Management at the Ministry of Health in the Period 2016 - 2020
General Assessment of the Current Situation of Public Investment Capital Management at the Ministry of Health in the Period 2016 - 2020 -
 Occupational Safety and Health Management System According to Ohasas 18001:2007 Standard
Occupational Safety and Health Management System According to Ohasas 18001:2007 Standard -
 Approach to Quality Management System
Approach to Quality Management System
3.1.2. Recommended policy solutions
To overcome the above shortcomings, the Government needs to research and issue specific regulations and instructions on the following contents:

a) Regulations on the responsibilities for implementing, building, applying, maintaining and improving the QMS at State administrative agencies of individuals and units at the central and local levels and heads of State administrative agencies;
b) Provide guidance on how to select the scope of application of the QMS in each type of public administrative agency, such as: Departments, People's Committees of cities, districts, communes, hospitals, schools... so that units can select the scope of application appropriate to their conditions, resources and general development roadmap. At the same time, they can share and learn from each other among regions and localities across the country;
c) Specify some training contents, training duration, and training subjects necessary when building, applying, and improving the QMS at the unit to ensure full awareness of the purpose, meaning, and methods of implementing the QMS in each agency from leaders to civil servants.
d) Specific regulations on the agency responsible for inspection, supervision and the mechanism for inspection and supervision of the quality of consulting and certification activities of individuals and organizations practicing consulting and certification in Vietnam.
e) Stipulate the titles, ranks, and requirements for specific skills and knowledge that officers must have for each title and rank in the field of quality management, thereby officially recognizing quality management as a
Professionalism, like any other professional discipline, must exist in an organization. Only then can quality become culture and quality management become a regular and indispensable activity of an organization;
3.2. Support policies of the Ministry of Health
3.2.1. Existing problems of issued policies
Although the Ministry of Health has made great efforts in issuing policies to improve quality in hospitals as presented in Chapter II. However, partly due to the low level of management of hospitals, uneven understanding and awareness of quality at all levels in the hospital, poor ability to control and manage operational processes, lack of updating and learning about new management methods..., at the same time, due to the lack of appropriate support policies from hospitals as well as from higher management agencies, the application of new management technologies and quality management systems established in hospitals have not been maintained and effectively promoted after certification. This is reflected in the following specific limitations in public hospitals:
a) Lack of training and knowledge needed to build, maintain and improve the QMS
Confusion in choosing a QMS model at the initial stage. As analyzed in section 1.2.6, chapter 1, there are many approaches to QMS, the choice of approach to build a QMS according to standards or non-standards depends on each hospital. The Law on Medical Examination and Treatment passed by the National Assembly on November 23, 2009 mentioned the certification of quality improvement for medical examination and treatment facilities, applying quality management standards to improve the quality of medical examination and treatment, but there is currently no circular guiding how to implement this work in hospitals. Meanwhile, awareness as well as information about QMS models in the world are not regularly and promptly updated for hospitals.
Failure to maintain the commitment and interest of hospital leadership after the QMS has been established. During the Quality System development phase,
The leaders considered achieving ISO 9001:2008 certification as one of the hospital's goals, however, after this goal was achieved, the organization's leaders did not see the priority goal associated with maintaining and improving the QMS.
b) There are no official regulations on the function and position of quality management in hospitals.
From a management perspective, the construction and application of a Quality System according to standards is an effort by the hospital to deploy the quality management function - which has been deployed before but at a lower level. As with the deployment of other management functions such as human resources, finance, etc., the deployment of the quality management function also requires an appropriate organizational structure model. During the pre-certification System construction phase, this function is mainly performed by a non-permanent, cross-functional group - often called the ISO Steering Committee or ISO Team. However, the reality at many organizations shows that the ISO Committee or ISO Team model does not operate effectively during the post-certification Quality System maintenance and improvement phase. This leads to the fact that many hospitals after achieving ISO certification do not have a unified answer to questions such as "Who is responsible for the quality of the Quality System's operations?", "Who determines what the Quality System will be like and what is needed in 3 years, 5 years or more?"... Currently, in the Hospital Regulations issued by the Ministry of Health in 1997, there are no specific regulations on the organizational structure of general and specialized hospitals of grades I, II, III regarding the quality management function and the position of staff doing quality management work in the hospital, so this function has not been officially recognized and most of the staff doing this work are currently part-time.
Maintaining and improving the quality management system is a new task that arises after the quality management system is built. This requires staff working in quality management at hospitals (Quality Management Representative - QMR, ISO secretary/coordinator) to have knowledge and skills in improvement.
A systematic, complete and regularly updated quality management system ensures effective maintenance and improvement of the quality management system. During the process of building a quality management system, this knowledge and skills are provided by the consultant through training and implementation guidance. When the project ends, usually at the stage when the hospital has completed the ISO certification assessment, the support of the consultants is no longer available, revealing the hospital's lack of capacity in this regard. In addition, in some cases, the QMR and/or ISO secretary/coordinator resigns, changes jobs, and the organization appoints a replacement who may not have experience and training in building, implementing and controlling a quality management system, causing the system to gradually become formal and outdated with the hospital's daily operations.
c) Lack of specific inspection, evaluation and monitoring mechanisms on the application, maintenance and improvement of the QMS in hospitals
Normally, to become a competent internal auditor, in addition to the factors of general knowledge and skills, an internal auditor needs to be guided and mentored through about 4-5 assessments. However, by the time of certification, a Quality System is usually only internally assessed about 2 times, and not all internal auditors fully participate and are guided in these two assessments. In the process of building a QMS, internal audit capacity is often provided mainly by consulting/guidance organizations. In addition, the lack of internal audit capacity in many units is even more serious due to the problem of personnel changes (people leaving, people transferring to new jobs).
The transformation of an organization from a command-based management (notices, decisions, proposals, requests, etc.) to a system-based management with closely linked work processes, regulations, and instructions requires the organization to clearly identify, for each document, the "owner" and the "stakeholders", responsibilities, and methods of coordination in amending and updating documents. During the operation, when the bases for building documents change, such as regulatory documents,
In order to ensure that the hospital's document system does not hinder the general management activities and the effectiveness of the quality management system, in reality, many hospitals after certifying the quality management system often do not have an ISO committee and ISO officers, so they often transfer documents to the units without revealing how to periodically review and update documents when necessary. This leads to the situation where the document system is outdated with reality.
d) Lack of appropriate incentive and reward mechanisms for the application, maintenance and improvement of the QMS in hospitals.
Typically, when an organization develops a QMS, a new set of standards of competence, awareness and behaviour is also established. The success of the QMS depends largely on the ability to establish and reinforce the habits of implementing and complying with these new standards. This in turn depends on whether the incentives, motivation, rewards and disciplinary mechanisms are linked to and directed towards the level of implementation and compliance with the new standards. In most cases, the incentives, motivation, rewards and disciplinary provisions are established before the QMS is implemented and, therefore, are often not updated to reflect the new needs arising from the implementation, maintenance and improvement of the QMS.
e) Ability to implement strategies and focus on improving the performance of low quality systems.
Ideally, the construction of a Quality System should achieve three basic goals: implementing strategy (and measurement), standardizing operations, and improving capacity/awareness. However, in most cases, units applying a Quality Management System, especially following the ISO 9001 standard model, only focus on the goal of standardizing operations (through the development of processes, regulations, instructions/forms) and do not pay due attention to implementing the strategy through developing a system of criteria for quality activities - Key quality performance indicators (KQPIs), establishing and managing goals and targets.
quality in a consistent manner with the quality policy, and more importantly, with the organization's strategy. This leads to the fact that many units after applying the QMS (with processes, regulations, and instructions) have not been able to quantify the benefits of operational efficiency that the application of ISO 9000 brings, nor answer the question "Where needs to be improved?" or "Which objects/areas should improvement activities be directed at?".
f) Lack of full and effective use of management tools for improvement activities.
Normally, most projects to build a quality management system often bring about improvements in a short time right after the quality system is built and applied, mainly thanks to efforts to standardize quality activities with other processes, regulations and standards. However, after a few years of applying the quality management system, the level of implementation of improvement activities becomes slower and less obvious compared to other activities. The unfortunate thing behind this reality is that many units have not recognized that the quality management system according to the standard model is only a basic management framework and it needs to be supplemented with appropriate management tools to increase efficiency, or in other words, the application of the quality management system is only the first step on the path of quality management of the organization. In order to help the QMS improve continuously, the organization needs to identify and use appropriate management tools for purposes such as error prevention (FMEA, Porka Yoke, etc.), continuous improvement (5S/Kaizen), quality performance assessment and identification of improvement opportunities (usually statistical tools), evaluation and selection of improvement opportunities (quality costs and project management), implementation of improvement projects (change management, training/guidance, etc.), monitoring and analysis of improvement project results (statistical tools, quality costs). This risk, if present at the same time as the risk of not having a suitable KQPIs system and low internal assessment capacity, will completely paralyze the organization's QMS improvement activities.
g) Lack of effective linkage between quality management activities and other management activities in the organization
Quality management is a “cross-functional” activity and needs to be implemented consistently and fully at all levels and functions of the organization. One of the fundamental challenges in implementing a QMS is how to make other management departments fully perceive the relevance and value of the QMS in their operations, without overlapping or being “cumbersome” in terms of procedures. Experience in many organizations that have applied a QMS shows that after several years of implementation, the organization is still struggling with questions such as “Product quality or operational quality?”, “External customers or internal customers?”, “What is the scope of the QMS?” “How is the quality policy different from the organizational strategy?”, “What is the difference between quality objectives and production and business objectives?”. An inadequate approach to addressing this relationship often leads organizations to one of two opposing extremes. In the first case, organizations may be content with a QMS that is too narrow in terms of service provision activities. It is common in organizations using this approach that many people and departments feel indifferent to the QMS and consider themselves “outside the system”. The second case is that organizations “coldly” impose the QMS “rigidly” on all activities, ignoring the “specificities” of these areas of activity. Choosing this approach often leads to the phenomenon of “ISO officers” instructing professional staff and creating “inhibition” in departments because they feel imposed without being truly convinced by the new standards in the QMS.
3.2.2. Recommended policy solutions
To overcome the above limitations and while waiting for a Government decree regulating titles and ranks in the field of quality management, the Ministry of Health should soon issue a circular guiding quality management in hospitals, especially in public hospitals, which should disclose the following contents:
a. Principles of organizing and implementing quality management
Patient-centered. Hospitals must pay attention to patient satisfaction and needs, solicit opinions and accept patient feedback.
to provide quality management solutions that meet the needs and expectations of patients;
Hospital leaders must set the task of building, applying, maintaining and continuously improving the quality management system as the central and continuous task of the hospital;
All staff and employees in the hospital must be aware of and participate in hospital quality management activities;
Decisions related to building quality standards and hospital quality improvement activities must be based on practical, scientific grounds and have specific evidence;
Quality management must be systematic, ensuring continuous improvement.
b. Hospital quality management tasks
Develop quality management plans and programs;
Applying standards, models and quality management methods;
Establish a database on hospital quality management;
Establish a set of indicators to monitor and evaluate hospital quality;
Organize the implementation of national technical standards, regulations, rules, and professional instructions in medical examination and treatment issued by the Ministry of Health;
Implement measures to ensure patient safety;
Clinical testing;
Periodic quality assessment at the hospital.
c. Determine conditions to ensure maintenance and improvement of quality management activities
quantity
Organizational structure of quality management in hospitals;
Establish the title, responsibility and authority of each member in the organization.
quality management organization in hospital;
Ensure human resources and training in quality management;
Ensure conditions of equipment and means;