pancreaticojejunostomy after pancreaticoduodenectomy: a prospective randomized trial. Annals of Surgery , 246 (3), 425-433.
160. Pessaux P., Sauvanet A., Mariette C., et al (2011). External pancreatic duct stent pancreatic fistula rate after pancreaticoduodenectomy: prospective multicenter randomized trial. Annals of Surgery , 253(5), 879-885.
161. Satoi S., Yamamoto T., Yanagimoto H., et al (2019). Does modified Blumgart anastomosis without intra-pancreatic ductal stenting reduce post-operative pancreatic fistula after pancreaticojejunostomy? Asian journal of surgery , 42(1), 343-349.
162. Hwang SE, Jung MJ, Cho BH, et al (2014). Clinical considerations and nutritional effects of early oral feeding after pancreaticoduodenectomy. Korean journal of hepato-biliary-pancreatic surgery , 18(3), 84-89.
163. Fujieda H., Yokoyama Y., Hirata A., et al (2017). Does Braun Anastomosis Have an Impact on the Incidence of Delayed Gastric Emptying and the Extent of Intragastric Bile Reflux Following Pancreatoduodenectomy? - A Randomized Controlled Study. Digestive Surgery , 34 (6), 462-468.
164. Cai Y., Gao P., Li Y., et al (2018). Laparoscopic pancreaticoduodenectomy with major venous resection and reconstruction: anterior superior mesenteric artery first approach. Surgical endoscopy , 32 (10), 4209-4215.
165. Hwang SE, Jung MJ, Cho BH, et al (2014). Clinical considerations and nutritional effects of early oral feeding after pancreaticoduodenectomy. Korean journal of hepato-biliary-pancreatic surgery , 18(3), 84-89.
166. Daskalaki D., Butturini G., Molinari E., et al (2011). A grading system can predict clinical and economic outcomes of pancreatic fistula posterior
pancreaticoduodenectomy: results in 755 consecutive patients.
Langenbeck's archives of surgery , 396(1), 91-98.
167. Le Huu Phuoc, Le Van Cuong, Nguyen Cao Cuong et al. (2018). Study on the results of pancreaticoduodenectomy for malignant diseases around the papilla of Vater at Binh Dan Hospital. Ho Chi Minh City Medical Journal , 22(2), 474 - 482. Ho Chi Minh City Medical Journal , 22, 2 (2018), 474 - 482.
168. Gao F., Li J., Quan S., et al (2016). Risk Factors and Treatment for Hemorrhage after Pancreaticoduodenectomy: A Case Series of 423 Patients. BioMed research international , 2016, 2815693.
169. Kim JY, Park JS, Kim JK, et al (2013). A model for predicting pancreatic leakage after pancreaticoduodenectomy based on the international study group of pancreatic surgery classification. Korean journal of hepato-biliary-pancreatic surgery , 17 (4), 166-170.
170. Panni RZ, Guerra J., Hawkins W.G., et al (2019). National Pancreatic Fistula Rates after Minimally Invasive Pancreaticoduodenectomy: A NSQIP Analysis. Journal of the American College of Surgeons .
171. Fang CH, Chen QS, Yang J., et al (2016). Body Mass Index and Stump Morphology Predict an Increased Incidence of Pancreatic Fistula After Pancreaticoduodenectomy. World journal of surgery , 40(6), 1467-1476.
172. Miyamoto R., Oshiro Y., Sano N., et al (2019). Three-Dimensional Remnant Pancreatic Volumetry Predicts Postoperative Pancreatic Fistula in Pancreatic Cancer Patients after Pancreaticoduodenectomy. Gastrointestinal tumors , 5(3-4), 90-99.
173. Morimoto M., Honjo S., Sakamoto T., et al (2019). Bacterial smear test of drainage fluid after pancreaticoduodenectomy can predict postoperative pancreatic fistula. Pancreatology , 19(2), 274-279.
174. Hackert T., Hinz U., Pausch T., et al (2016). Postoperative pancreatic fistula: We need to redefine grades B and C. Surgery , 159(3), 872-877.
175. Smits FJ, Van Santvoort HC, Besselink MG, et al (2017). Management of Severe Pancreatic Fistula After Pancreatoduodenectomy. JAMA Surgery , 152 (6), 540-548.
176. Kurnicki J., Wrzesinska N., Kabala P (2011). Meckel's diverticulum encumbered in an umbilical hernia--case report. Polski przeglad chirurgiczny , 83 (7), 386-388.
177. Zacharakis E., Papadopoulos V., Athanasiou T., et al (2008). An unusual presentation of Meckel diverticulum as strangulated femoral hernia. Southern medical journal , 101 (1), 96-98.
178. Henegouwen MI, Van Gulik TM, DeWit, LT, et al (1997). Delayed gastric emptying after standard pancreaticoduodenectomy versus pylorus-preserving pancreaticoduodenectomy: an analysis of 200 consecutive patients. Journal of the American College of Surgeons , 185 (4), 373-379.
179. Hanna MM, Gadde R., Tamariz L., et al (2015). Delayed Gastric Emptying After Pancreaticoduodenectomy: Is Subtotal Stomach Preserving Better or Pylorus Preserving? Journal of gastrointestinal surgery : official journal of the Society for Surgery of the Alimentary Tract , 19(8), 1542-1552.
180. Zhou Y., Lin J., Wu L., et al (2015). Effect of antecolic or retrocolic reconstruction of the stomach/duodenojejunostomy on delayed gastric
emptying after pancreaticoduodenectomy: a meta-analysis. BMC gastroenterology , 15 (6), 68.
181. Bu XM, Xu J., Dai XW, et al (2006). Is delayed gastric emptying so terrible after pylorus-preserving pancreaticoduodenectomy? Prevention and management. World journal of gastroenterology , 12 (39), 6382- 6385.
182. Duconseil P., Turrini O., Ewald J., et al (2014). Biliary complications after pancreaticoduodenectomy: skinny bile ducts are surgeons' enemies. World journal of surgery , 38 (11), 2946-2951.
183. Zhu J., Kou J., Dong H., et al (2018). Biliary reconstruction with a pedicled gallbladder flap in patients during pancreaticoduodenectomy. The Journal of surgical research , 225 (5), 76-81.
184. Ito T., Sugiura T., Okamura Y., et al (2018). Late benign biliary complications after pancreatoduodenectomy. Surgery , 163 (6), 1295- 1300.
185. Adam MA, Choudhury K., Dinan MA, et al (2015). A. Minimally Invasive Versus Open Pancreaticoduodenectomy for Cancer: Practice Patterns and Short-term Outcomes Among 7061 Patients. Annals of Surgery , 262 (2), 372-377.
186. Singh AN, Pal S., Kilambi R., et al (2018). Diabetes after pancreaticoduodenectomy: can we predict it? The Journal of surgical research , 227(7), 211-219.
187. Shimada K., Sakamoto Y., Sano T., et al (2006). The role of paraaortic lymph node involvement on early recurrence and survival after macroscopic curative resection with extended lymphadenectomy for pancreatic carcinoma. Journal of the American College of Surgeons , 203(3), 345-352.
188. Yamamoto Y., Ikoma H., Morimura R., et al (2014). Optimal duration of the early and late recurrence of pancreatic cancer after pancreatectomy based on the difference in the prognosis. Pancreatology , 14(6), 524-529.
189. Guerard AS, Ayav A., Busby H., et al (2017). Early liver metastases in resectable periampullary cancer: Incidence and risk factors. European journal of radiology , 93(8), 265-272.
190. Chapman BC, Gleisner A., Ibrahim-Zada I., et al (2018). Laparoscopic pancreaticoduodenectomy: changing the management of ampullary neoplasms. Surgical endoscopy , 32 (2), 915-922.
APPENDIX 1:
DEFINITION OF GROUPS OF PANCREATIC LYMPH NODES
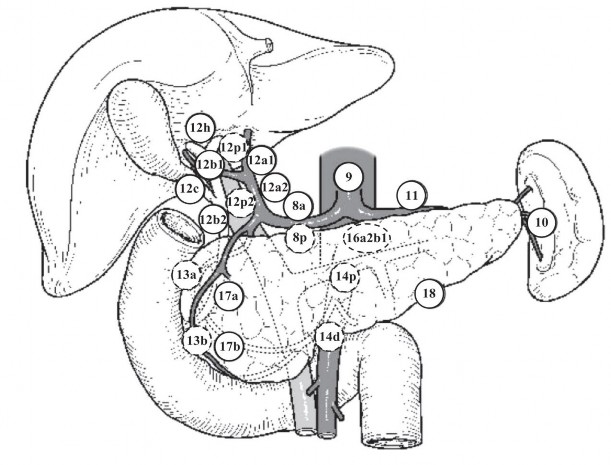
LOCATION OF LYMPH GROUPS
Source: according to Miyazaki (2015) [1]
Lymph node group Definition
1 Right paracardial lymph node group
2 Left paracardiac lymph node group
3 Groups of lymph nodes along the lesser curvature of the stomach
4 Groups of lymph nodes along the greater curvature of the stomach
5 Suprapyloric lymph nodes
APPENDIX 2
AMERICAN SOCIETY OF ANESTHESIOLOGISTS - ASA HEALTH CLASSIFICATION
(American Society of Anesthesiologists)
ASA 1
Good health | |
ASA 2 | Have a disease that does not affect health and daily life day. |
ASA 3 | Have a disease that affects daily activities (diabetes with complications) vascular disease, obstructive pulmonary disease, angina pectoris…). |
ASA 4 | Has a serious illness that threatens the patient's life (cancer, heart failure, renal failure) kidney, abdominal aortic aneurysm, severe bronchial asthma…). |
ASA 5 | The patient's condition is very serious, dying and unable to live. 24 hours with or without surgery. |
ASA 6 | Brain dead patient |
Maybe you are interested!
-
 Research on the application of laparoscopic surgery to assist in resection of pancreatic head duodenum to treat ampullary tumors - 24
Research on the application of laparoscopic surgery to assist in resection of pancreatic head duodenum to treat ampullary tumors - 24 -
 Research on the application of laparoscopic surgery in the treatment of rectal cancer - 16
Research on the application of laparoscopic surgery in the treatment of rectal cancer - 16 -
 Research on the application of laparoscopic surgery in the treatment of rectal cancer - 18
Research on the application of laparoscopic surgery in the treatment of rectal cancer - 18 -
 Research on the application of smartphone utility software to evaluate traffic noise and road surface iri index - 14
Research on the application of smartphone utility software to evaluate traffic noise and road surface iri index - 14 -
 Research on the application of smartphone utility software to evaluate traffic noise and road surface iri index - 15
Research on the application of smartphone utility software to evaluate traffic noise and road surface iri index - 15
APPENDIX 3
TNM CLASSIFICATION ACCORDING TO AJCC – 2010 (Source: AJCC – 2010 [1])
DUODENAL AND VATER'S AMPLE CANCER
T: Tumor size
Primary tumor not evaluable | |
T0 | No evidence of primary tumor |
Tis | Carcinoma in situ |
T1 | Tumor invades mucosa and submucosa with tumor size ≤ 1 cm (duodenal cancer); Tumor localized in the sphincter of Oddi (Vater tumor) |
T2 | Tumor invades the muscle layer or tumor size ≥ 1 cm (duodenal cancer); Duodenal muscle invasion or tumor size ≥ 1 cm (Vater tumor) |
T3 | Tumor invades the pancreas and the fat layer around the pancreas |
T4 | Tumor invades soft tissue around the pancreas or adjacent organs outside the pancreas |
N: Regional lymph node metastasis
No lymph nodes assessed | |
N0 | No regional lymph node metastasis |
N1 | Regional lymph node metastasis |
Regional lymph nodes include groups: 13 (a, b), 17 (a, b), 14 (p, d), 12b, 8 (a, p) and * 5, * 6 ( * optional) | |
M: Distant metastasis
Distant lymph node metastasis cannot be assessed. | |
M0 | No distant metastasis |
M1 | Distant metastasis |
Distant metastasis: lung, bone, pleura, liver, peritoneum, brain, thyroid metastasis adrenal, non-regional lymph nodes (groups 9, 10, group 16), skin… | |