Research by Nguyen Thi Tam [6] also had similar comments: Simple root compression syndrome due to herniation into the graft foramen, simple spinal cord compression syndrome due to central disc herniation, combined root compression syndrome due to paracentral disc herniation.
Through our study, we can see the similarity between clinical and herniated location on magnetic resonance imaging, thereby showing that clinical syndromes are important in orienting the diagnosis of herniated location, however, magnetic resonance imaging is needed to accurately diagnose the herniated location, because a significant number of patients have dissimilarities between clinical syndromes and herniated location on magnetic resonance. In addition, magnetic resonance also helps to comprehensively assess the entire spine, in terms of the number of herniated levels, herniated location, herniated level, herniated type, spinal stenosis level, etc. These parameters are important in the diagnosis, treatment and prognosis of the disease. Thereby, it shows that magnetic resonance is an imaging diagnostic tool that plays a very important role in cervical disc herniation.
CONCLUDE
Through a study of 60 cases of cervical disc herniation at the Department of Neurosurgery at E Hospital, we would like to draw the following conclusions:
1. About clinical characteristics
Cervical disc herniation is not a rare disease. The disease is most common in the age group of 41 - 60 (63.4%), the average age is 54.03 +/- 14.45 years old. The disease incidence rate by gender is 1.4/1 male/female.
The disease often starts after a heavy activity that impacts the cervical spine. People who work in a heavy environment or have incorrect posture for a long time have a higher risk of getting the disease (60%).
The time from symptom onset to patient visit to the doctor is mainly less than 12 months, accounting for 70%.
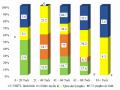
Clinical manifestations include 4 main syndromes: Spinal syndrome (66.7%), simple root compression syndrome (45%), simple spinal cord compression syndrome (13.33%), combined root-spinal cord compression syndrome (41.67%).
2. About magnetic resonance imaging characteristics
Magnetic resonance imaging is a particularly valuable diagnostic imaging method, allowing for definitive diagnosis of the location, number and extent of lesions. Our study shows that:
Single-level hernia is most common (38.3%), double-level hernia is often found at C3-C4, C4-C5 15%, triple-level hernia is mainly found at C3-C4, C4-C5, C5-C6 accounting for 13.33%.
The most common herniated location is C5 – C6 (32.23%).
Central hernia (47.11%), paracentral hernia (38.84%), hernia into the graft foramen (14.05%).
Mild spinal stenosis accounted for a high rate of 58.3%, severe spinal stenosis accounted for 21.7%.
Posterior disc herniation is clearly seen on T1 and T2 longitudinal and transverse slices.
Longitudinal images assess the entire spine, location, and number of herniated levels.
Herniated discs have decreased signal on T2, reduce disc height, compress the cerebrospinal fluid cavity at the level of herniation, and increase spinal cord signal at the level of herniation on T2. When combining longitudinal and transverse cuts, the level of herniation, compression of the spinal cord or nerve roots, and the diameter of the spinal canal and spinal cord at the level of the vertebral body and the level of herniation can be assessed.
REFERENCES
1. Nguyen Duc Hiep (2000). Research on diagnosis and surgical treatment of cervical disc herniation , Thesis of Resident Doctor of Hospital
2. Le Thi Hong Lien (1997). Clinical survey and treatment of cervical root-spinal pathology due to disc herniation and cervical spinal stenosis due to degeneration , Master's thesis in Medicine and Pharmacy
3. Ho Huu Luong (2003). Cervical spondylosis and cervical disc herniation , Medical Publishing House.
4. Ho Huu Luong (2020). "Part II. Cervical disc herniation", Cervical spondylosis and disc herniation, Medical Publishing House, Hanoi, pp. 115 - 155.
5. Vo Xuan Son, Tran Hung Phong, Tran Minh Tam (1999). Retrospective study of 64 surgical cases of cervical disc herniation at Cho Ray Hospital, Vietnam-Australia Conference on Neurosurgery , pp.30-31.
6. Nguyen Thi Tam (2002). Clinical study and magnetic resonance imaging of cervical spine herniation compared with surgery , PhD thesis in Medical Science
7. Tran Trung, Hoang Duc Kiet (1999). "Diagnosis of cervical disc herniation by magnetic resonance imaging " , Journal of Practical Medicine , pp.3-6.
8. Nguyen Vu (2004). Study on diagnosis and surgical results of lumbar and lumbosacral disc herniation , Medical Doctor's thesis.
9. A Campi, S Pontesilli, S Gerevini, et al. (2000). "Comparison of MRI pulse sequences for investigation of lesions of the cervical spinal cord " , Neuroradiology , 42(9), 669-675.
10. Dhagat PK, Jain M., Singh SN (2017). "Failed Back Surgery Syndrome: Evaluation with Magnetic Resonance Imaging " , J Clin Diagn Res , 11(5), TC06–TC09.
11. Faghih-Jouibari M., Moazzeni K., Amini-Navai A. (2016). "Anatomical considerations for insertion of pedicular screw in cervicothoracic junction " , Iran J Neurol , 15(4), pp. 228-231.
12. Jian Li, Deng-lu Yan, Zai-Heng Zhang (2008). "Percutaneous cervical nucleoplasty in the treatment of cervical disc herniation " , European Spine Journal , 17(12), 1664-1669.
13. Kazunori Takahashi, Tsunemaro Koyama, Seishi Igarashi, et al. (1987). "A classification of the herniated cervical disc based on metrizamide CT " , No Shinkei geka. Neurological Surgery , 15(2), 125-130.
14. Kelly JC, Groarke PJ, Butler JS (2012). "The natural history and clinical syndromes of degenerative cervical spondylosis " , Adv Orthop , 2012(2012).
15. Khoi DT, Shayan UR, Monique JV (2012). "Bone morphogenetic proteins and degenerative disk disease " , Neurosurgery , 70, pp. 996 - 1002.
16. Kiyoshi Mochida, Hiromichi Komori, Atsushi Okawa, et al. (1998). "Regression of cervical disc herniation observed on magnetic resonance images " , Spine , 23(9), 990-995.
17. Lewis S Sharps, Zacharias Isaac (2002). "Percutaneous disc decompression using Nucleoplasty® " , Pain Physician , 5(2), 121-126.
18. Martin MD, Boxell CM, Malone DG (2002). "Pathophysiology of lumbar disc degeneration: a review of the literature " , Neurosurg. Focus , 13(2), pp. 1-6.
19. Munusamy T., Thien A., Anthony MG (2015). "Computed tomographic morphometric analysis of cervical pedicles in a multiethnic Asian population and relevance to subaxial cervical pedicle screw fixation. " , Eur Spine J , 24(1), pp. 120 - 126.
20. Nancy E Epstein, Renee D Hollingsworth (2017). "Nursing review section of surgical neurology international: Evaluation of cervical disc disease and when surgery is warranted " , Surg Neurol Int , 8(136), pp. 15.
21. SW Spurling RG (1944). "Lateral rupture of the cervical intervertebral disc. A common cause of shoulder and arm pain " , Surg Gynecol Obtet , 78, pp 350 - 358.
22. Sarker MH (1998). "Analysis of outcome of surgically treated patiens with cervical myeloradiculopathy and factors influensing the outcome " , The 3 Asian Conference of Neurological Surgeons , pp.7.
23. Sebaaly A., Lahoud MJ, Rizkallah M. (2018). "Etiology, Evaluation, and Treatment of Failed Back Surgery Syndrome " , Asian Spine J , 12(3), pp. 574-585.
24. Shin-Yuan Chen, Chang-Ho Tseng, Wen-Ta Chiu (1997). "Anterior cervical fusion with a modified Robinson-Smith method. Retrospective study of 58 cases " , Clinical Neurology and Neurosurgery (99), S173.
25. Sureka B., Mittal A., Mittal MK (2018). "Morphometric analysis of cervical spinal canal diameter, transverse foramen, and pedicle width using computed tomography in Indian population " , Neurol India , 66(2), pp. 454-458.
26. van Uden S., Silva-Correia J., Oliveira J.M. (2017). "Current strategies for treatment of intervertebral disc degeneration: substitution and regeneration possibilities " , Biomater Res , 21(22).
27. Waxenbaum JA, Futterman B (2018). "Anatomy, Back, Intervertebral Discs " ,
StatPearls Publishing .
28. Yumashev GS (1976). "Cervical osteochondrosis " , Osteochondrosis of the Spin (101-199), pp.13-72.
MEDICAL RECORD RESEARCH
Numerical order:Medical record code:
Full name:Year old:Gender: ☐ 1. Male ☐ 2. Female Occupation:
Contact address:
Date of examination:
Cervical spine MRI date:
PART A - MEDICAL QUESTIONNAIRE
I. Reason for hospitalization:
II. Medical history:
1. Time of illness: Month
2. Onset: ☐ 1: Gradual ☐ 2: Sudden
3. Initiating circumstances:
☐ 1: Natural
☐ 2: After favorable factors:
PART B - MEDICAL EXAMINATION
I. Whole body
Height: Circuit: Temperature:
Weight: Blood Pressure:
II. Full body examination
1. Consciousness: ☐ 1: Alert ☐ 2: Coma
2. Spinal HC examination
☐ 1: Yes | ☐ 2: No | |
2.2. CSC pain points: | ☐ 1: Yes | ☐ 2: No |
2.3. Restriction of CSC movement: | ☐ 1: Yes | ☐ 2: No |
Maybe you are interested!
-
 Study on Some Clinical and Paraclinical Features of Appendiceal Abscess
Study on Some Clinical and Paraclinical Features of Appendiceal Abscess -
 Clinical features, endoscopic images of laryngoscopy and pathological anatomy of vocal cord cysts - 7
Clinical features, endoscopic images of laryngoscopy and pathological anatomy of vocal cord cysts - 7 -
 Clinical and Paraclinical Features of Lacrimal Gland Tumor
Clinical and Paraclinical Features of Lacrimal Gland Tumor -
 Study on clinical features, pathology and treatment results of non-epithelial gastrointestinal cancer at Viet Duc Hospital - 17
Study on clinical features, pathology and treatment results of non-epithelial gastrointestinal cancer at Viet Duc Hospital - 17 -
 Clinical Features of Patients with Psoriasis Vulgaris
Clinical Features of Patients with Psoriasis Vulgaris

3. Examination of cervical root (nerve) syndrome.
☐ 1: Yes | ☐ 2: No | |
3.2. Pain increases when coughing or sneezing: | ☐ 1: Yes | ☐ 2: No |
3.3. Pain relief when stretching CS: | ☐ 1: Yes | ☐ 2: No |
3.4. Numbness of upper limbs: | ☐ 1: Yes | ☐ 2: No |
3.5. Spurling's sign: | ☐ 1: Yes | ☐ 2: No |
3.6. Bell signal: | ☐ 1: Yes | ☐ 2: No |
3.7. Cervical root-type motor disorders: | ☐ 1: Yes | ☐ 2: No |
3.8. Cervical root reflex disorder: | ☐ 1: Yes | ☐ 2: No |
3.9. Upper limb muscle atrophy: | ☐ 1: Yes | ☐ 2: No |
4. Examination of cervical spinal cord syndrome: | ||
4.1. TW-type quadriplegia: | ☐ 1: Yes | ☐ 2: No |
4.2. HC Brown – Séquard: | ☐ 1: Yes | ☐ 2: No |
4.3. Increased tendon reflexes in the limbs: | ☐ 1: Yes | ☐ 2: No |
4.4. Babinsky reflex: | ☐ 1: Yes | ☐ 2: No |
4.5. Hoffmann's sign: | ☐ 1: Yes | ☐ 2: No |
4.6. Reduced sensation below the level of injury: | ☐ 1: Yes | ☐ 2: No |
4.7. TW-type sphincter disorder: | ☐ 1: Yes | ☐ 2: No |
IV. MRI images | ||
1. On T1, T2 cut vertically | ||
1.1. Changes in physiological curve: | ☐ 1: Yes | ☐ 2: No |
1.2. Vertebral body injury: | ☐ 1: Yes | ☐ 2: No |
Vertebral body collapse: | ☐ 1: Yes | ☐ 2: No |
Vertebral body slippage: | ☐ 1: Yes | ☐ 2: No |
Bone spurs, bone beaks | ☐ 1: Yes | ☐ 2: No |