149. Stout JW, Visness CM, Enright P., Lamm C. et al (2006). Classification of severity in children: the contribution of pulmonary function testing. Archives of pediatrics & adolescent medicine, 160(8), 844-850.
150. Siroux V., Basagada X., Boudier A. et al (2011). Identifying adult asthma phenotypes using a clustering approach. European Respiratory Journal, 38(2), 310-317.
151. Agache I., and Akdis CA (2016). Endotypes of allergic diseases and asthma: an important step in building blocks for the future of precision medicine. Allergology international, 65(3), 243-252.
No.:…………………. BA Code:………………
MEDICAL RECORD RESEARCH (first time)
Date ……, month….., year 20…
A. Administration
Patient's full name:……………………………………Age:.......................... Date of birth:……………………………………………………………………... Gender: male □ female □ Ethnicity: Kinh □, other ethnicities □…………....... Address:……………………………………………………………………….... Mother's full name:…………………………………………Phone number:………………….. Educational level: ……………………Occupation: ……………………………… Father's full name:………………………………………….Phone number:………………….. Educational level: ……………………Occupation: ………………………………
B. Prehistory
Personal history
Obstetrics: Second child:……… Normal delivery □, Caesarean section □, Intervention □
Full term □ Preterm □ Birth weight: ……..kg Vaccinations: Full □, No □
Exclusive breastfeeding for the first 4-6 months: yes □, no □. Exclusive formula feeding from birth: yes □, no □. Formula feeding + breast milk for the first 4-6 months: yes □, no □. Medical conditions: ………………………………………………………….. Family history
Hen | VMDU | sinus | VDCD | Medal | DU medicine | DU food | Other | |
Dad | ||||||||
Mom | ||||||||
Brothers and sisters | ||||||||
Other people |
Maybe you are interested!
-
 Study on asthma control status in children with bronchial asthma and allergic rhinitis - 18
Study on asthma control status in children with bronchial asthma and allergic rhinitis - 18 -
 Study on asthma control status in children with bronchial asthma and allergic rhinitis - 22
Study on asthma control status in children with bronchial asthma and allergic rhinitis - 22 -
 Study on asthma control status in children with bronchial asthma and allergic rhinitis - 19
Study on asthma control status in children with bronchial asthma and allergic rhinitis - 19 -
 Car body electrical practice - 8
zt2i3t4l5ee
zt2a3gs
zt2a3ge
zc2o3n4t5e6n7ts
If the voltage is out of specification, replace the wire or connector.
If the voltage is within specification, install the front fog light relay and follow step 5.
Step 5 Check the front fog light switch
- Remove the D4 connector of the fog light switch
- Use a multimeter to measure the resistance of the front fog light switch.
Measurement location
Condition
Standard
D4-3 (BFG) -D4-4 (LFG)
Light switchFront Fog OFF
>10kΩ
D4-3 (BFG) -D4-4 (LFG)
Front fog light switchON
<1 Ω
- Standard resistor
D4 connector is located on the combination switch assembly.
If the resistance is out of specification, replace the combination switch (the fog light switch is located in the combination switch).
If the resistance is within specification, follow step 6.
Step 6 Check wiring and connectors (front fog light relay-light selector switch)
- Disconnect connector D4 of the combination switch assembly
- Use a voltmeter to measure the voltage value of jack D4 on the wire side.
Measurement location
Control modecontrol
Standard
D4-3 (BFG) - (-) AQ
TAIL
11 to 14 V
D4 connector for the wiring of the combination switch assembly
If the voltage does not meet the standard, replace the wire or connector.
If the voltage is within standard, there may have been an error in the previous measurements.
Step 7 Check the front fog lights
- Remove the front fog light electrical connector.
- Supply battery voltage to the fog lamp terminals
Jack 8, B9 of front fog lamp on the electrical side
blind first.
Power supply location
Terms and Conditions
Battery positive terminal - Terminal 2Battery negative terminal - Terminal 1
Fog lightsbefore morning
- If the light does not come on, replace the bulb.
If the light is on, re-plug the jack and continue to step 8.
Step 8 Check wiring and connectors (relay and front fog lights)
- Disconnect the B8 and B9 connectors of the front fog lights.
- Use a voltmeter to measure voltage at the following locations:
Measurement location
Switch location
Terms and Conditions
B8-2 - (-) AQ
Electric lock ON TAIL size switchFog switch ON
11 to 14 V
B9-2 - (-) AQ
Electric lock ONTAIL size switch Fog switch ON
11 to 14 V
B8 and B9 connectors on the front fog lamp wiring side
Voltage is not up to standard, repair or replace the jack. If up to standard, there may have been an error in the measurement process.
2.2.4. Procedure for removing, installing and adjusting fog lights 1. Procedure for removing
- Remove the front inner ear pads
Use a screwdriver to remove the 3 screws and remove the front part of the front inner ear liner
-Remove the fog light assembly
+ Disconnect the connector.
+ Use a screwdriver to remove 3 screws to remove the fog light cover
2. Installation sequence
-Rotate the fog lamp bulb in the direction indicated by the arrow as shown in the figure and remove the fog lamp from the fog lamp assembly.
-Rotate the fog light bulb in the direction indicated by the arrow as shown in the figure and install the light into the fog light assembly.
- Use a screwdriver to install the fog light cover
-Install the electrical connector
Attention: Be careful not to damage the plastic thread on the lamp assembly.
- Install the front inner ear pads
Use a screwdriver to install the front inner bumper with 3 screws.
3. Prepare the vehicle to adjust the fog light convergence. Prepare the vehicle:
- Make sure there is no damage or deformation to the vehicle body around the fog lights.
- Add fuel to the fuel tank
- Add oil to standard level.
- Add engine coolant to standard level.
- Inflate the tire to standard pressure.
- Place spare tire, tools and jack in original design position
- Do not leave any load in the luggage compartment.
- Let a person weighing about 75 kg sit in the driver's seat.
4. Prepare to check the fog light convergence
a/ Prepare the vehicle status as follows:
- Place the car in a dark enough place to see the lines. The lines are the dividing line, below which the light from the fog lights can be seen but above which it cannot.
- Place the car perpendicular to the wall.
- Keep a distance of 7.62 m between the center of the fog lamp and the wall.
- Park the car on level ground.
- Press the car down a few times to stabilize the suspension.
Note: A distance of approximately 7.62 m is required between the vehicle (fog lamp center) and the wall to adjust the convergence correctly. If the distance of 7.62 m cannot be achieved, set the correct distance of 3 m to check and adjust the fog lamp convergence. (Since the target area varies with the distance, please follow the instructions as shown in the figure.)
b/ Prepare a piece of thick white paper about 2 m high and 4 m wide to use as a screen.
c/ Draw a vertical line through the center of the screen (line V).
d/ Set the screen as shown in the picture. Note:
- Keep the screen perpendicular to the ground.
- Align the V line on the screen with the center of the vehicle.
e/Draw the reference lines (H, V LH and V RH lines) on the screen as shown in the figure.HINT:
Mark the center of the fog lamp on the screen. If the center mark cannot be seen on the fog lamp, use the center of the fog lamp or the manufacturer's name mark on the fog lamp as the center mark.
H line (fog light height):
Draw a line across the screen so that it passes through the center mark. Line H should be at the same height as the center mark of the fog light bulb.
Line V LH, V RH (center mark position of left fog lamp LH and right fog lamp RH):
Draw two lines so that they intersect line H at the center marks.
5. Check the fog light convergence
a/ Cover the fog lamp or remove the connector of the other side fog lamp to prevent light from the unchecked fog lamp from affecting the fog lamp convergence test.
b/ Start the engine.
c/ Turn on the fog lights and make sure that the dividing line is outside the standard area as shown in the drawing.
6. Adjust the fog light convergence
Use a screwdriver to adjust the fog light to the standard area by turning the toe adjustment screw.
Note: If the screw is adjusted too far, loosen it and then tighten it again, so that the last rotation of the light adjustment screw is clockwise.
3. Self-study questions
1. Describe the operating principle of the lighting system with automatic headlight function
2. Describe the operating principle of the lighting system with the function of rotating headlights when turning
3. Draw diagram and connect lighting system on Hyundai Porter car
4. Draw diagram and connect lighting system on Honda Accord 1992
5. Draw the lighting circuit on a 1993 Toyota Lexus
LESSON 3 MAINTENANCE AND REPAIR OF SIGNAL SYSTEM
I. IMPLEMENTATION GOAL
After completing this lesson, students will be able to:
- Distinguish between types of signals on cars
- Correctly describe common symptoms and suspected areas causing damage.
- Connecting signal circuits ensures technical requirements
- Disassemble, install, check, maintain and repair the signal system to ensure technical requirements.
- Ensure safety in work and industrial hygiene
II. LESSON CONTENT
1. General description
The signal system equipped on cars aims to create signals to notify other vehicles participating in traffic about the vehicle's operating status such as: stopping, parking, braking, reversing, turning...
Signals are used either by light such as headlamps, brake lights, turn signals….. or by sound such as horns, reverse music….
Just like the lighting system. A signal system circuit usually consists of: battery, fuse, wire, relay, electrical load and control switch. Only some switches of the signal system are on the combination switch. The switches of other signals are usually located in different locations such as in the gearbox or brake pedal……
2. Maintenance and repair
2.1. Turn signals and hazard lights
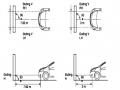
The installation location of the turn signal is shown in Figure 3.1. The turn signal control switch is located in the combination switch under the steering wheel. Turning this switch to the right or left will make the turn signal turn right or left.
The hazard light switch is used when the vehicle has a problem while participating in traffic. When the hazard light switch is turned on, all the turn signals on the vehicle will light up at a certain frequency. The hazard light switch is usually placed separately from the turn signal switch (some old cars integrate the hazard and turn signal switches on the same combination switch cluster).
Figure 3.1 Turn signal switch Figure 3.2 Hazard switch
The part that generates the flashing frequency for the lights is called a turn signal relay. The turn signal relay usually has 3 terminals: B (positive power supply); E (negative power supply); L (providing the turn signal switch to distribute to the
lamp)
2.1.1. Circuit diagram
To generate the frequency for the turn signal, a turn signal relay is used in the turn signal circuit. The current from the turn signal relay will be sent to the turn signal switch assembly to distribute the current to the turn signal lights for the driver's purpose.
Figure 3.3. Schematic diagram of a turn signal circuit without a hazard switch
1. Battery; 2. Electric lock; 3. Turn signal relay; 4. Turn signal switch; 5. Turn signal lamp; 6. Turn signal lamp; 7. Hazard switch
Figure 3.4 Schematic diagram of turn signal circuit with hazard switch
1. Battery; 2. Combination switch cluster; 3. Turn signal;
4. Turn signal light; 5. Turn signal relay
Today's cars no longer use three-pin turn signal relays (B, L, E) but use eight-pin turn signal relays (figure 3.5) (pin number 8 is used for hazard lights).
For this type, the current supplying the turn signal lights is supplied directly from the turn signal relay to the lights.
div.maincontent .p { color: black; font-family:"Times New Roman", serif; font-style: normal; font-weight: normal; text-decoration: none; font-size: 14pt; margin:0pt; } div.maincontent p { color: black; font-family:"Times New Roman", serif; font-style: normal; font-weight: normal; text-decoration: none; font-size: 14pt; margin:0pt; } div.maincontent .s1 { color: black; font-family:"Times New Roman", serif; font-style: normal; font-weight: normal; text-decoration: none; font-size: 13pt; } div.maincontent .s2 { color: black; font-family:"Times New Roman", serif; font-style: italic; font-weight: normal; text-decoration: none; font-size: 14pt; } div.maincontent .s3 { color: black; font-family:"Times New Roman", serif; font-style: normal; font-weight: normal; text-decoration: none; font-size: 14pt; } div.maincontent .s4 { color: black; font-family:"Times New Roman", serif; font-style: normal; font-weight: normal; text-decoration: none; font-size: 13pt; } div.maincontent .s5 { color: black; font-family:"Times New Roman", serif; font-style: normal; font-weight: normal; text-decoration: none; font-size: 13pt; vertical-align: 1pt; } div.maincontent .s6 { color: black; font-family:"Times New Roman", serif; font-style: normal; font-weight: normal; text-decoration: none; font-size: 11pt; } div.maincontent .s7 { color: black; font-family:"Times New Roman", serif; font-style: normal; font-weight: normal; text-decoration: none; font-size: 14pt; vertical-align: -9pt; } div.maincontent .s8 { color: black; font-family:"Times New Roman", serif; font-style: normal; font-weight: normal; text-decoration: none; font-size: 11pt; } div.maincontent .s9 { color: #008000; font-family:"Times New Roman", serif; font-style: normal; font-weight: normal; text-decoration: none; font-size: 14pt; } div.maincontent .s10 { color: black; font-family:"Times New Roman", serif; font-style: italic; font-weight: normal; te
Car body electrical practice - 8
zt2i3t4l5ee
zt2a3gs
zt2a3ge
zc2o3n4t5e6n7ts
If the voltage is out of specification, replace the wire or connector.
If the voltage is within specification, install the front fog light relay and follow step 5.
Step 5 Check the front fog light switch
- Remove the D4 connector of the fog light switch
- Use a multimeter to measure the resistance of the front fog light switch.
Measurement location
Condition
Standard
D4-3 (BFG) -D4-4 (LFG)
Light switchFront Fog OFF
>10kΩ
D4-3 (BFG) -D4-4 (LFG)
Front fog light switchON
<1 Ω
- Standard resistor
D4 connector is located on the combination switch assembly.
If the resistance is out of specification, replace the combination switch (the fog light switch is located in the combination switch).
If the resistance is within specification, follow step 6.
Step 6 Check wiring and connectors (front fog light relay-light selector switch)
- Disconnect connector D4 of the combination switch assembly
- Use a voltmeter to measure the voltage value of jack D4 on the wire side.
Measurement location
Control modecontrol
Standard
D4-3 (BFG) - (-) AQ
TAIL
11 to 14 V
D4 connector for the wiring of the combination switch assembly
If the voltage does not meet the standard, replace the wire or connector.
If the voltage is within standard, there may have been an error in the previous measurements.
Step 7 Check the front fog lights
- Remove the front fog light electrical connector.
- Supply battery voltage to the fog lamp terminals
Jack 8, B9 of front fog lamp on the electrical side
blind first.
Power supply location
Terms and Conditions
Battery positive terminal - Terminal 2Battery negative terminal - Terminal 1
Fog lightsbefore morning
- If the light does not come on, replace the bulb.
If the light is on, re-plug the jack and continue to step 8.
Step 8 Check wiring and connectors (relay and front fog lights)
- Disconnect the B8 and B9 connectors of the front fog lights.
- Use a voltmeter to measure voltage at the following locations:
Measurement location
Switch location
Terms and Conditions
B8-2 - (-) AQ
Electric lock ON TAIL size switchFog switch ON
11 to 14 V
B9-2 - (-) AQ
Electric lock ONTAIL size switch Fog switch ON
11 to 14 V
B8 and B9 connectors on the front fog lamp wiring side
Voltage is not up to standard, repair or replace the jack. If up to standard, there may have been an error in the measurement process.
2.2.4. Procedure for removing, installing and adjusting fog lights 1. Procedure for removing
- Remove the front inner ear pads
Use a screwdriver to remove the 3 screws and remove the front part of the front inner ear liner
-Remove the fog light assembly
+ Disconnect the connector.
+ Use a screwdriver to remove 3 screws to remove the fog light cover
2. Installation sequence
-Rotate the fog lamp bulb in the direction indicated by the arrow as shown in the figure and remove the fog lamp from the fog lamp assembly.
-Rotate the fog light bulb in the direction indicated by the arrow as shown in the figure and install the light into the fog light assembly.
- Use a screwdriver to install the fog light cover
-Install the electrical connector
Attention: Be careful not to damage the plastic thread on the lamp assembly.
- Install the front inner ear pads
Use a screwdriver to install the front inner bumper with 3 screws.
3. Prepare the vehicle to adjust the fog light convergence. Prepare the vehicle:
- Make sure there is no damage or deformation to the vehicle body around the fog lights.
- Add fuel to the fuel tank
- Add oil to standard level.
- Add engine coolant to standard level.
- Inflate the tire to standard pressure.
- Place spare tire, tools and jack in original design position
- Do not leave any load in the luggage compartment.
- Let a person weighing about 75 kg sit in the driver's seat.
4. Prepare to check the fog light convergence
a/ Prepare the vehicle status as follows:
- Place the car in a dark enough place to see the lines. The lines are the dividing line, below which the light from the fog lights can be seen but above which it cannot.
- Place the car perpendicular to the wall.
- Keep a distance of 7.62 m between the center of the fog lamp and the wall.
- Park the car on level ground.
- Press the car down a few times to stabilize the suspension.
Note: A distance of approximately 7.62 m is required between the vehicle (fog lamp center) and the wall to adjust the convergence correctly. If the distance of 7.62 m cannot be achieved, set the correct distance of 3 m to check and adjust the fog lamp convergence. (Since the target area varies with the distance, please follow the instructions as shown in the figure.)
b/ Prepare a piece of thick white paper about 2 m high and 4 m wide to use as a screen.
c/ Draw a vertical line through the center of the screen (line V).
d/ Set the screen as shown in the picture. Note:
- Keep the screen perpendicular to the ground.
- Align the V line on the screen with the center of the vehicle.
e/Draw the reference lines (H, V LH and V RH lines) on the screen as shown in the figure.HINT:
Mark the center of the fog lamp on the screen. If the center mark cannot be seen on the fog lamp, use the center of the fog lamp or the manufacturer's name mark on the fog lamp as the center mark.
H line (fog light height):
Draw a line across the screen so that it passes through the center mark. Line H should be at the same height as the center mark of the fog light bulb.
Line V LH, V RH (center mark position of left fog lamp LH and right fog lamp RH):
Draw two lines so that they intersect line H at the center marks.
5. Check the fog light convergence
a/ Cover the fog lamp or remove the connector of the other side fog lamp to prevent light from the unchecked fog lamp from affecting the fog lamp convergence test.
b/ Start the engine.
c/ Turn on the fog lights and make sure that the dividing line is outside the standard area as shown in the drawing.
6. Adjust the fog light convergence
Use a screwdriver to adjust the fog light to the standard area by turning the toe adjustment screw.
Note: If the screw is adjusted too far, loosen it and then tighten it again, so that the last rotation of the light adjustment screw is clockwise.
3. Self-study questions
1. Describe the operating principle of the lighting system with automatic headlight function
2. Describe the operating principle of the lighting system with the function of rotating headlights when turning
3. Draw diagram and connect lighting system on Hyundai Porter car
4. Draw diagram and connect lighting system on Honda Accord 1992
5. Draw the lighting circuit on a 1993 Toyota Lexus
LESSON 3 MAINTENANCE AND REPAIR OF SIGNAL SYSTEM
I. IMPLEMENTATION GOAL
After completing this lesson, students will be able to:
- Distinguish between types of signals on cars
- Correctly describe common symptoms and suspected areas causing damage.
- Connecting signal circuits ensures technical requirements
- Disassemble, install, check, maintain and repair the signal system to ensure technical requirements.
- Ensure safety in work and industrial hygiene
II. LESSON CONTENT
1. General description
The signal system equipped on cars aims to create signals to notify other vehicles participating in traffic about the vehicle's operating status such as: stopping, parking, braking, reversing, turning...
Signals are used either by light such as headlamps, brake lights, turn signals….. or by sound such as horns, reverse music….
Just like the lighting system. A signal system circuit usually consists of: battery, fuse, wire, relay, electrical load and control switch. Only some switches of the signal system are on the combination switch. The switches of other signals are usually located in different locations such as in the gearbox or brake pedal……
2. Maintenance and repair
2.1. Turn signals and hazard lights
The installation location of the turn signal is shown in Figure 3.1. The turn signal control switch is located in the combination switch under the steering wheel. Turning this switch to the right or left will make the turn signal turn right or left.
The hazard light switch is used when the vehicle has a problem while participating in traffic. When the hazard light switch is turned on, all the turn signals on the vehicle will light up at a certain frequency. The hazard light switch is usually placed separately from the turn signal switch (some old cars integrate the hazard and turn signal switches on the same combination switch cluster).
Figure 3.1 Turn signal switch Figure 3.2 Hazard switch
The part that generates the flashing frequency for the lights is called a turn signal relay. The turn signal relay usually has 3 terminals: B (positive power supply); E (negative power supply); L (providing the turn signal switch to distribute to the
lamp)
2.1.1. Circuit diagram
To generate the frequency for the turn signal, a turn signal relay is used in the turn signal circuit. The current from the turn signal relay will be sent to the turn signal switch assembly to distribute the current to the turn signal lights for the driver's purpose.
Figure 3.3. Schematic diagram of a turn signal circuit without a hazard switch
1. Battery; 2. Electric lock; 3. Turn signal relay; 4. Turn signal switch; 5. Turn signal lamp; 6. Turn signal lamp; 7. Hazard switch
Figure 3.4 Schematic diagram of turn signal circuit with hazard switch
1. Battery; 2. Combination switch cluster; 3. Turn signal;
4. Turn signal light; 5. Turn signal relay
Today's cars no longer use three-pin turn signal relays (B, L, E) but use eight-pin turn signal relays (figure 3.5) (pin number 8 is used for hazard lights).
For this type, the current supplying the turn signal lights is supplied directly from the turn signal relay to the lights.
div.maincontent .p { color: black; font-family:"Times New Roman", serif; font-style: normal; font-weight: normal; text-decoration: none; font-size: 14pt; margin:0pt; } div.maincontent p { color: black; font-family:"Times New Roman", serif; font-style: normal; font-weight: normal; text-decoration: none; font-size: 14pt; margin:0pt; } div.maincontent .s1 { color: black; font-family:"Times New Roman", serif; font-style: normal; font-weight: normal; text-decoration: none; font-size: 13pt; } div.maincontent .s2 { color: black; font-family:"Times New Roman", serif; font-style: italic; font-weight: normal; text-decoration: none; font-size: 14pt; } div.maincontent .s3 { color: black; font-family:"Times New Roman", serif; font-style: normal; font-weight: normal; text-decoration: none; font-size: 14pt; } div.maincontent .s4 { color: black; font-family:"Times New Roman", serif; font-style: normal; font-weight: normal; text-decoration: none; font-size: 13pt; } div.maincontent .s5 { color: black; font-family:"Times New Roman", serif; font-style: normal; font-weight: normal; text-decoration: none; font-size: 13pt; vertical-align: 1pt; } div.maincontent .s6 { color: black; font-family:"Times New Roman", serif; font-style: normal; font-weight: normal; text-decoration: none; font-size: 11pt; } div.maincontent .s7 { color: black; font-family:"Times New Roman", serif; font-style: normal; font-weight: normal; text-decoration: none; font-size: 14pt; vertical-align: -9pt; } div.maincontent .s8 { color: black; font-family:"Times New Roman", serif; font-style: normal; font-weight: normal; text-decoration: none; font-size: 11pt; } div.maincontent .s9 { color: #008000; font-family:"Times New Roman", serif; font-style: normal; font-weight: normal; text-decoration: none; font-size: 14pt; } div.maincontent .s10 { color: black; font-family:"Times New Roman", serif; font-style: italic; font-weight: normal; te -
 Internal control of revenue and expenditure activities at the National Children's Hospital - 2
Internal control of revenue and expenditure activities at the National Children's Hospital - 2

B. History of asthma and allergic rhinitis History of asthma
When did the child first cough and wheeze (months old) -----
Number of wheezing episodes in 1 year:
_year old
Diagnosis of asthma is confirmed when:
Diagnosed with asthma: Step 1 □, Step 2 □, Step 3 □, Step 4 □
In the past year: HSCC:Emergency times: _Hospitalization: _Times Hospitalization: _day
Wheezing
Night: Waking up at night
Every night 1 time/week 1 time/month 2 times/week 2 times/month
Daytime: Early morning
Daily 1 time/week 1 time/month 2 times/week 2 times/month
Chest pain Chest heaviness (older children)
Average number of days of cough/acute episode ….. Cough episode > 10 days Cough episode < 10 days
No symptoms between episodes Sometimes symptoms persist between episodes
Month of year when wheezing occurs
1
2 | 3 | 4 | 5 | 6 | 7 | 8 | 9 | 10 | 11 | 12 |
Spring Summer Fall Winter Weather changes
Wheezing and wheezing often occur when:
Asthma triggersWeather change | Yes □ | No □ |
Pollen Inhalation | Yes □ | No □ |
Children inhale cigarette smoke | Yes □ | No □ |
Inhaling other types of fumes: incense, perfume, paint | Yes □ | No □ |
Breathe polluted air when going out | Yes □ | No □ |
After the child exerts himself | Yes □ | No □ |
High fever, runny nose | Yes □ | No □ |
When children are sad, angry, scared | Yes □ | No □ |
Eat allergic food | Yes □ | No □ |
After using the medicine | Yes □ | No □ |
Drug name:………………………… | ||
Medications the child is taking before the first visit
Name of drug used
Dosage | Time of use | Daily use | Use intermittently | |
ICS | ||||
Oral corticosteroids | ||||
Corticoid TM | ||||
SABA | ||||
LABA | ||||
Leukotriene | ||||
Corticosteroid nasal spray | ||||
H1 resistance | ||||
Vasoconstrictor |
No □. | ||
Arbitrary increase in dose | Yes □ | No □. |
Reduce dose on your own | Yes □ | No □. |
Quit smoking | Yes □ | No □. |
Forgot medication | Yes □ | No □ |
Use medication as prescribed by your doctor
Does the child use other medications to treat asthma? Yes □, No □ Medication name:
…………….
Children with allergic diseases such as:
Eczema □, GERD □, Drug allergies □ Food allergies □ Aspirin intolerance □ Allergic rhinitis □
VMDU medical history
First appearance of sneezing, runny nose, itchy nose (months old): ……….. Diagnosis of VMDU year: ………. Age
Symptoms in the nose
Sneezing □ Itchy nose □ Runny nose □
Nasal voice □ Nasal congestion □ Difficulty breathing □ Decreased sense of smell □
Extranasal symptoms?
Itchy eyes □ Red eyes □ Dry cough □ Itchy throat □ Headache □
Other symptoms:
Snoring □ Sleep apnea □ Daytime sleepiness □
What factors cause VMDU symptoms in children?
Have | □ No | |
Dust inhalation | Have | □ No |
Smoke (cigarettes, incense, perfume, paint) | Have | □ No |
Pollen exposure | Have | □ No |
Dog and cat contact | Have | □ No |
Feather contact | Have | □ No |
Eat foods that cause allergies | Have | □ No |
Medication (name) □ Medication name: ………………………………..
When (month) does VMDU appear?
1
2 | 3 | 4 | 5 | 6 | 7 | 8 | 9 | 10 | 11 | 12 |
Spring Summer Fall Winter Weather changes
VMDU Classification
< 4 days/week □ | and/or | < 4 weeks/year □ | |
Persistent □ | > 4 days/week | and | > 4 weeks/year □ |
Do VMDU symptoms cause the following effects on my child?
Insomnia Yes □ No □
Learning Impact Yes □ No □
Impact on daily activities Yes □ No □ Discomfort due to nasal symptoms Yes □ No □ Grade: Mild Normal sleep and no symptoms above
Moderate - severe Has 1 or more of the above symptoms
Tobacco related issues
Child lived in same apartment with smoker under 12 months of age Yes □, No □
Smokers: father □, mother □, ……………………. Smokers often smoke indoors
Yes □, No □
Smokers who regularly smoke outside the home Yes □, No □
Does the child smoke? Yes □, No □
Child's residence:
Housing 1. Urban □ 3. Rural □ 2. Mountainous area □ Around the house there are: 1. Factory □ 2. Mining area, ore □ House has: dogs □, cats □ birds, poultry □ House uses: Mattress □ Carpet □ Stuffed animals, feather coat □ House uses honeycomb coal stove □
C. Clinical examination
Province, good contact | □ .Temperature:………..◦C | |
Skin color:…………… Mucous membrane: pink | □, pale □ | |
Peripheral lymph nodes: yes | □, no □ |
Weight:…………..kg, Height:…………cm BMI:…………
Cardiovascular: Heart rate:………..beats/minute Fast □, Slow □, Normal □ Heart sounds: normal □, abnormal □ …………………
Respiration: Chest: normal, raised □, collapsed □
Respiratory rate:………….times/minute Fast □, Slow □, normal □ RRPN: clear □, decreased□ SpO2:………………….
Pulmonary rales: moist rales □, wheezing rales □, snoring rales □, bronchial rales □
Nasopharynx: Mucosa: pale □ Red □ Normal □ Nasal turbinate: edematous □ hypertrophied □ Normal □
Nasal polyps: Yes □ No □
Deviated septum: Yes □ No □
Exudate: Clear mucus □ Cloudy mucus □ None □ Enlarged tonsils: Yes □ No □
VA: Yes □ No □
Other parts:………………………………………………………
D. Paraclinical
1. Complete blood count
Visit
BC | N | L | EO | HC | Hb | TC | |
1 |
2. Blood Ig E concentration:…………………Normal □, high □.
3. Skin prick test:
Allergen
Result | Allergen | Result | |
Positive evidence | ……………mm | Proof | ……………….mm |
D.pter | ……………mm | D.farine | ……………….mm |
Blomia | ……………mm | Cockroach | ……………….mm |
Dog | ……………mm | Cat | ……………….mm |
Aspegilus fungus | ……………mm | Pollen | ……………….mm |
4. First measurement of respiratory function and NNO, FENO
Index
Before bronchial reversibility test (2 puffs of ventolin through spacer) | After test | |
FEV1 | ||
FVC | ||
FEV1/FVC | ||
PEAK FLOW | ||
FENO nose | ||
Bronchial FENO | ||
E. Diagnosis
Assessment of asthma severity and control according to GINA at first visit
Characteristics: In the past 4 weeks, the patient has had
Reply | Full control | Partial control | No control | |
Daytime symptoms > 2 times/week? | Yes □ No □ | Do not have | There are 1- 2 characteristic | There are 3 - 4 characteristic |
Any night waking due to asthma? | Yes □ No □ | |||
Need symptom relief > 2 times/week? | Yes □ No □ |
ACT score: ……… (questionnaire attached)
Assessment of asthma control with VMDU
CARAT score: ……… (questionnaire attached)
Risk factors for poor asthma outcomes
Risk factors for an asthma attack in the next few months
Risk factors for fixed airflow limitation | Risk factors for drug side effects | |
Uncontrolled asthma symptoms Have 1 severe exacerbation/12 months had NKQ placed or was in HSCC SABA > 200 doses/month Inadequate ICS: not prescribed, poor compliance, incorrect spray technique Low FEV1 < 60% Exposure: cigarette smoke, pollution, allergens Associated diseases: sinusitis, food allergies, obesity obesity | Lack of ICS treatment Exposure to cigarette smoke, chemicals, etc. Low initial FEV1 High eosinophils in blood and sputum | System: Oral corticosteroids: No: High dose ICS: None: Topical: Gargle (or drink water) after spraying: No Yes Wipe face and eyes when using ICS spray or through mask: No Yes |
Asthma
Asthma
Symptom | |
Level 1 | Asthma symptoms or SABA requirement < 2 times/month No nighttime awakenings in the past month; No risk factors for exacerbations; No asthma attacks in the past year |
Level 2 | Asthma symptoms are few, but Have a risk factor for an exacerbation |
Asthma symptoms or SABA requirement between > 2 times/month and < 2 times/week Or waking up at night due to asthma ≥ 1 time/month | |
Level 3 | Asthma symptoms or SABA requirement > 2 times/week |
Level 4 | Daily asthma symptoms; Or waking up at night due to asthma ≥ 1 time/week |
Diagnosis of asthma
During the attack
Out of attack | B | infection | ||
No control | Partial control | K | H. control all | |
There are risk factors | No risk factors | |||
Asthma level 1 | Asthma level 2 | H | level 3 | Asthma level 4 |
Asthma severity according to GINA Mild: Well controlled with first and second line treatment | Yes □ No □ | |||
Moderate: Control with third-line treatment | Yes □ No □ | |||
Severe: Requires level 4 treatment | Yes □ No □ | |||
Not controlled by line 4 treatment | Yes □ No □ | |||
F. TREATMENT
Attack relief: Ventolin: …….puffs each time, ……times a day.
Prevention: ………………………………………………….. Comorbidities: …………………………………………….. Control of triggers:……………………………….. Asthma action plan:………………………………….. Follow-up date: ………………………………………………