had a clear reduction in FEV1. The group with FEV1 < 80% had a higher need for ICS than the other two groups, and after 6 months of treatment, this group had an average number of requests for SABA reliever medication of 1.0 ± 1.4 times, higher than the groups with mild and normal FEV1. In addition, the respiratory function and good asthma control rate according to CARATkids of the group with clearly reduced FEV1 were lower than those of the other two groups.
Stout conducted a study on a group of asthmatic children aged 8-11 years living in the city in two periods from 1992-1994 (Cohort 1) and from 1998-2001 (Cohort 2). For children diagnosed with mild intermittent asthma based on clinical symptoms, after measuring spirometry to classify the severity of asthma, 22.8% of children in cohort 1 and 27.7% of children in cohort 2 were diagnosed with moderate and severe asthma 149 . Thus, spirometry plays a role in classifying the severity of asthma in children over 5 years old more accurately and objectively than asking about the patient and clinical examination. Based on spirometry, we can distinguish the severity of asthma and classify asthma phenotypes. The concomitant decrease in FEV1 values with FeNO concentrations may suggest that clinicians can classify a group of asthmatic children with a non-allergic asthma phenotype who have reduced respiratory function, poor response to ICS treatment, or who have been diagnosed with asthma but have missed prophylaxis or used medication irregularly.
Nowadays, scientists use a new approach to determine the pathophysiological phenotype of asthma (endotype). The phenotype is determined through genetic markers on the airway, which in HPQ is often the type 2 asthma endotype. In this phenotype, Th2 cell-dependent inflammatory markers are measured by non-invasive methods through sputum samples, exhaled air, nasal lavage fluid, bronchial lavage fluid, urine, serum and blood 150 . The combination of clinical phenotype and pathophysiological phenotype helps clinicians to orient treatment drugs during the process of monitoring asthma control,
Maybe you are interested!
-
 Study on asthma control status in children with bronchial asthma and allergic rhinitis - 21
Study on asthma control status in children with bronchial asthma and allergic rhinitis - 21 -
 Study on asthma control status in children with bronchial asthma and allergic rhinitis - 22
Study on asthma control status in children with bronchial asthma and allergic rhinitis - 22 -
 Study on asthma control status in children with bronchial asthma and allergic rhinitis - 19
Study on asthma control status in children with bronchial asthma and allergic rhinitis - 19 -
 Car body electrical practice - 8
zt2i3t4l5ee
zt2a3gs
zt2a3ge
zc2o3n4t5e6n7ts
If the voltage is out of specification, replace the wire or connector.
If the voltage is within specification, install the front fog light relay and follow step 5.
Step 5 Check the front fog light switch
- Remove the D4 connector of the fog light switch
- Use a multimeter to measure the resistance of the front fog light switch.
Measurement location
Condition
Standard
D4-3 (BFG) -D4-4 (LFG)
Light switchFront Fog OFF
>10kΩ
D4-3 (BFG) -D4-4 (LFG)
Front fog light switchON
<1 Ω
- Standard resistor
D4 connector is located on the combination switch assembly.
If the resistance is out of specification, replace the combination switch (the fog light switch is located in the combination switch).
If the resistance is within specification, follow step 6.
Step 6 Check wiring and connectors (front fog light relay-light selector switch)
- Disconnect connector D4 of the combination switch assembly
- Use a voltmeter to measure the voltage value of jack D4 on the wire side.
Measurement location
Control modecontrol
Standard
D4-3 (BFG) - (-) AQ
TAIL
11 to 14 V
D4 connector for the wiring of the combination switch assembly
If the voltage does not meet the standard, replace the wire or connector.
If the voltage is within standard, there may have been an error in the previous measurements.
Step 7 Check the front fog lights
- Remove the front fog light electrical connector.
- Supply battery voltage to the fog lamp terminals
Jack 8, B9 of front fog lamp on the electrical side
blind first.
Power supply location
Terms and Conditions
Battery positive terminal - Terminal 2Battery negative terminal - Terminal 1
Fog lightsbefore morning
- If the light does not come on, replace the bulb.
If the light is on, re-plug the jack and continue to step 8.
Step 8 Check wiring and connectors (relay and front fog lights)
- Disconnect the B8 and B9 connectors of the front fog lights.
- Use a voltmeter to measure voltage at the following locations:
Measurement location
Switch location
Terms and Conditions
B8-2 - (-) AQ
Electric lock ON TAIL size switchFog switch ON
11 to 14 V
B9-2 - (-) AQ
Electric lock ONTAIL size switch Fog switch ON
11 to 14 V
B8 and B9 connectors on the front fog lamp wiring side
Voltage is not up to standard, repair or replace the jack. If up to standard, there may have been an error in the measurement process.
2.2.4. Procedure for removing, installing and adjusting fog lights 1. Procedure for removing
- Remove the front inner ear pads
Use a screwdriver to remove the 3 screws and remove the front part of the front inner ear liner
-Remove the fog light assembly
+ Disconnect the connector.
+ Use a screwdriver to remove 3 screws to remove the fog light cover
2. Installation sequence
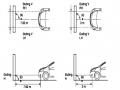
-Rotate the fog lamp bulb in the direction indicated by the arrow as shown in the figure and remove the fog lamp from the fog lamp assembly.
-Rotate the fog light bulb in the direction indicated by the arrow as shown in the figure and install the light into the fog light assembly.
- Use a screwdriver to install the fog light cover
-Install the electrical connector
Attention: Be careful not to damage the plastic thread on the lamp assembly.
- Install the front inner ear pads
Use a screwdriver to install the front inner bumper with 3 screws.
3. Prepare the vehicle to adjust the fog light convergence. Prepare the vehicle:
- Make sure there is no damage or deformation to the vehicle body around the fog lights.
- Add fuel to the fuel tank
- Add oil to standard level.
- Add engine coolant to standard level.
- Inflate the tire to standard pressure.
- Place spare tire, tools and jack in original design position
- Do not leave any load in the luggage compartment.
- Let a person weighing about 75 kg sit in the driver's seat.
4. Prepare to check the fog light convergence
a/ Prepare the vehicle status as follows:
- Place the car in a dark enough place to see the lines. The lines are the dividing line, below which the light from the fog lights can be seen but above which it cannot.
- Place the car perpendicular to the wall.
- Keep a distance of 7.62 m between the center of the fog lamp and the wall.
- Park the car on level ground.
- Press the car down a few times to stabilize the suspension.
Note: A distance of approximately 7.62 m is required between the vehicle (fog lamp center) and the wall to adjust the convergence correctly. If the distance of 7.62 m cannot be achieved, set the correct distance of 3 m to check and adjust the fog lamp convergence. (Since the target area varies with the distance, please follow the instructions as shown in the figure.)
b/ Prepare a piece of thick white paper about 2 m high and 4 m wide to use as a screen.
c/ Draw a vertical line through the center of the screen (line V).
d/ Set the screen as shown in the picture. Note:
- Keep the screen perpendicular to the ground.
- Align the V line on the screen with the center of the vehicle.
e/Draw the reference lines (H, V LH and V RH lines) on the screen as shown in the figure.HINT:
Mark the center of the fog lamp on the screen. If the center mark cannot be seen on the fog lamp, use the center of the fog lamp or the manufacturer's name mark on the fog lamp as the center mark.
H line (fog light height):
Draw a line across the screen so that it passes through the center mark. Line H should be at the same height as the center mark of the fog light bulb.
Line V LH, V RH (center mark position of left fog lamp LH and right fog lamp RH):
Draw two lines so that they intersect line H at the center marks.
5. Check the fog light convergence
a/ Cover the fog lamp or remove the connector of the other side fog lamp to prevent light from the unchecked fog lamp from affecting the fog lamp convergence test.
b/ Start the engine.
c/ Turn on the fog lights and make sure that the dividing line is outside the standard area as shown in the drawing.
6. Adjust the fog light convergence
Use a screwdriver to adjust the fog light to the standard area by turning the toe adjustment screw.
Note: If the screw is adjusted too far, loosen it and then tighten it again, so that the last rotation of the light adjustment screw is clockwise.
3. Self-study questions
1. Describe the operating principle of the lighting system with automatic headlight function
2. Describe the operating principle of the lighting system with the function of rotating headlights when turning
3. Draw diagram and connect lighting system on Hyundai Porter car
4. Draw diagram and connect lighting system on Honda Accord 1992
5. Draw the lighting circuit on a 1993 Toyota Lexus
LESSON 3 MAINTENANCE AND REPAIR OF SIGNAL SYSTEM
I. IMPLEMENTATION GOAL
After completing this lesson, students will be able to:
- Distinguish between types of signals on cars
- Correctly describe common symptoms and suspected areas causing damage.
- Connecting signal circuits ensures technical requirements
- Disassemble, install, check, maintain and repair the signal system to ensure technical requirements.
- Ensure safety in work and industrial hygiene
II. LESSON CONTENT
1. General description
The signal system equipped on cars aims to create signals to notify other vehicles participating in traffic about the vehicle's operating status such as: stopping, parking, braking, reversing, turning...
Signals are used either by light such as headlamps, brake lights, turn signals….. or by sound such as horns, reverse music….
Just like the lighting system. A signal system circuit usually consists of: battery, fuse, wire, relay, electrical load and control switch. Only some switches of the signal system are on the combination switch. The switches of other signals are usually located in different locations such as in the gearbox or brake pedal……
2. Maintenance and repair
2.1. Turn signals and hazard lights
The installation location of the turn signal is shown in Figure 3.1. The turn signal control switch is located in the combination switch under the steering wheel. Turning this switch to the right or left will make the turn signal turn right or left.
The hazard light switch is used when the vehicle has a problem while participating in traffic. When the hazard light switch is turned on, all the turn signals on the vehicle will light up at a certain frequency. The hazard light switch is usually placed separately from the turn signal switch (some old cars integrate the hazard and turn signal switches on the same combination switch cluster).
Figure 3.1 Turn signal switch Figure 3.2 Hazard switch
The part that generates the flashing frequency for the lights is called a turn signal relay. The turn signal relay usually has 3 terminals: B (positive power supply); E (negative power supply); L (providing the turn signal switch to distribute to the
lamp)
2.1.1. Circuit diagram
To generate the frequency for the turn signal, a turn signal relay is used in the turn signal circuit. The current from the turn signal relay will be sent to the turn signal switch assembly to distribute the current to the turn signal lights for the driver's purpose.
Figure 3.3. Schematic diagram of a turn signal circuit without a hazard switch
1. Battery; 2. Electric lock; 3. Turn signal relay; 4. Turn signal switch; 5. Turn signal lamp; 6. Turn signal lamp; 7. Hazard switch
Figure 3.4 Schematic diagram of turn signal circuit with hazard switch
1. Battery; 2. Combination switch cluster; 3. Turn signal;
4. Turn signal light; 5. Turn signal relay
Today's cars no longer use three-pin turn signal relays (B, L, E) but use eight-pin turn signal relays (figure 3.5) (pin number 8 is used for hazard lights).
For this type, the current supplying the turn signal lights is supplied directly from the turn signal relay to the lights.
div.maincontent .p { color: black; font-family:"Times New Roman", serif; font-style: normal; font-weight: normal; text-decoration: none; font-size: 14pt; margin:0pt; } div.maincontent p { color: black; font-family:"Times New Roman", serif; font-style: normal; font-weight: normal; text-decoration: none; font-size: 14pt; margin:0pt; } div.maincontent .s1 { color: black; font-family:"Times New Roman", serif; font-style: normal; font-weight: normal; text-decoration: none; font-size: 13pt; } div.maincontent .s2 { color: black; font-family:"Times New Roman", serif; font-style: italic; font-weight: normal; text-decoration: none; font-size: 14pt; } div.maincontent .s3 { color: black; font-family:"Times New Roman", serif; font-style: normal; font-weight: normal; text-decoration: none; font-size: 14pt; } div.maincontent .s4 { color: black; font-family:"Times New Roman", serif; font-style: normal; font-weight: normal; text-decoration: none; font-size: 13pt; } div.maincontent .s5 { color: black; font-family:"Times New Roman", serif; font-style: normal; font-weight: normal; text-decoration: none; font-size: 13pt; vertical-align: 1pt; } div.maincontent .s6 { color: black; font-family:"Times New Roman", serif; font-style: normal; font-weight: normal; text-decoration: none; font-size: 11pt; } div.maincontent .s7 { color: black; font-family:"Times New Roman", serif; font-style: normal; font-weight: normal; text-decoration: none; font-size: 14pt; vertical-align: -9pt; } div.maincontent .s8 { color: black; font-family:"Times New Roman", serif; font-style: normal; font-weight: normal; text-decoration: none; font-size: 11pt; } div.maincontent .s9 { color: #008000; font-family:"Times New Roman", serif; font-style: normal; font-weight: normal; text-decoration: none; font-size: 14pt; } div.maincontent .s10 { color: black; font-family:"Times New Roman", serif; font-style: italic; font-weight: normal; te
Car body electrical practice - 8
zt2i3t4l5ee
zt2a3gs
zt2a3ge
zc2o3n4t5e6n7ts
If the voltage is out of specification, replace the wire or connector.
If the voltage is within specification, install the front fog light relay and follow step 5.
Step 5 Check the front fog light switch
- Remove the D4 connector of the fog light switch
- Use a multimeter to measure the resistance of the front fog light switch.
Measurement location
Condition
Standard
D4-3 (BFG) -D4-4 (LFG)
Light switchFront Fog OFF
>10kΩ
D4-3 (BFG) -D4-4 (LFG)
Front fog light switchON
<1 Ω
- Standard resistor
D4 connector is located on the combination switch assembly.
If the resistance is out of specification, replace the combination switch (the fog light switch is located in the combination switch).
If the resistance is within specification, follow step 6.
Step 6 Check wiring and connectors (front fog light relay-light selector switch)
- Disconnect connector D4 of the combination switch assembly
- Use a voltmeter to measure the voltage value of jack D4 on the wire side.
Measurement location
Control modecontrol
Standard
D4-3 (BFG) - (-) AQ
TAIL
11 to 14 V
D4 connector for the wiring of the combination switch assembly
If the voltage does not meet the standard, replace the wire or connector.
If the voltage is within standard, there may have been an error in the previous measurements.
Step 7 Check the front fog lights
- Remove the front fog light electrical connector.
- Supply battery voltage to the fog lamp terminals
Jack 8, B9 of front fog lamp on the electrical side
blind first.
Power supply location
Terms and Conditions
Battery positive terminal - Terminal 2Battery negative terminal - Terminal 1
Fog lightsbefore morning
- If the light does not come on, replace the bulb.
If the light is on, re-plug the jack and continue to step 8.
Step 8 Check wiring and connectors (relay and front fog lights)
- Disconnect the B8 and B9 connectors of the front fog lights.
- Use a voltmeter to measure voltage at the following locations:
Measurement location
Switch location
Terms and Conditions
B8-2 - (-) AQ
Electric lock ON TAIL size switchFog switch ON
11 to 14 V
B9-2 - (-) AQ
Electric lock ONTAIL size switch Fog switch ON
11 to 14 V
B8 and B9 connectors on the front fog lamp wiring side
Voltage is not up to standard, repair or replace the jack. If up to standard, there may have been an error in the measurement process.
2.2.4. Procedure for removing, installing and adjusting fog lights 1. Procedure for removing
- Remove the front inner ear pads
Use a screwdriver to remove the 3 screws and remove the front part of the front inner ear liner
-Remove the fog light assembly
+ Disconnect the connector.
+ Use a screwdriver to remove 3 screws to remove the fog light cover
2. Installation sequence
-Rotate the fog lamp bulb in the direction indicated by the arrow as shown in the figure and remove the fog lamp from the fog lamp assembly.
-Rotate the fog light bulb in the direction indicated by the arrow as shown in the figure and install the light into the fog light assembly.
- Use a screwdriver to install the fog light cover
-Install the electrical connector
Attention: Be careful not to damage the plastic thread on the lamp assembly.
- Install the front inner ear pads
Use a screwdriver to install the front inner bumper with 3 screws.
3. Prepare the vehicle to adjust the fog light convergence. Prepare the vehicle:
- Make sure there is no damage or deformation to the vehicle body around the fog lights.
- Add fuel to the fuel tank
- Add oil to standard level.
- Add engine coolant to standard level.
- Inflate the tire to standard pressure.
- Place spare tire, tools and jack in original design position
- Do not leave any load in the luggage compartment.
- Let a person weighing about 75 kg sit in the driver's seat.
4. Prepare to check the fog light convergence
a/ Prepare the vehicle status as follows:
- Place the car in a dark enough place to see the lines. The lines are the dividing line, below which the light from the fog lights can be seen but above which it cannot.
- Place the car perpendicular to the wall.
- Keep a distance of 7.62 m between the center of the fog lamp and the wall.
- Park the car on level ground.
- Press the car down a few times to stabilize the suspension.
Note: A distance of approximately 7.62 m is required between the vehicle (fog lamp center) and the wall to adjust the convergence correctly. If the distance of 7.62 m cannot be achieved, set the correct distance of 3 m to check and adjust the fog lamp convergence. (Since the target area varies with the distance, please follow the instructions as shown in the figure.)
b/ Prepare a piece of thick white paper about 2 m high and 4 m wide to use as a screen.
c/ Draw a vertical line through the center of the screen (line V).
d/ Set the screen as shown in the picture. Note:
- Keep the screen perpendicular to the ground.
- Align the V line on the screen with the center of the vehicle.
e/Draw the reference lines (H, V LH and V RH lines) on the screen as shown in the figure.HINT:
Mark the center of the fog lamp on the screen. If the center mark cannot be seen on the fog lamp, use the center of the fog lamp or the manufacturer's name mark on the fog lamp as the center mark.
H line (fog light height):
Draw a line across the screen so that it passes through the center mark. Line H should be at the same height as the center mark of the fog light bulb.
Line V LH, V RH (center mark position of left fog lamp LH and right fog lamp RH):
Draw two lines so that they intersect line H at the center marks.
5. Check the fog light convergence
a/ Cover the fog lamp or remove the connector of the other side fog lamp to prevent light from the unchecked fog lamp from affecting the fog lamp convergence test.
b/ Start the engine.
c/ Turn on the fog lights and make sure that the dividing line is outside the standard area as shown in the drawing.
6. Adjust the fog light convergence
Use a screwdriver to adjust the fog light to the standard area by turning the toe adjustment screw.
Note: If the screw is adjusted too far, loosen it and then tighten it again, so that the last rotation of the light adjustment screw is clockwise.
3. Self-study questions
1. Describe the operating principle of the lighting system with automatic headlight function
2. Describe the operating principle of the lighting system with the function of rotating headlights when turning
3. Draw diagram and connect lighting system on Hyundai Porter car
4. Draw diagram and connect lighting system on Honda Accord 1992
5. Draw the lighting circuit on a 1993 Toyota Lexus
LESSON 3 MAINTENANCE AND REPAIR OF SIGNAL SYSTEM
I. IMPLEMENTATION GOAL
After completing this lesson, students will be able to:
- Distinguish between types of signals on cars
- Correctly describe common symptoms and suspected areas causing damage.
- Connecting signal circuits ensures technical requirements
- Disassemble, install, check, maintain and repair the signal system to ensure technical requirements.
- Ensure safety in work and industrial hygiene
II. LESSON CONTENT
1. General description
The signal system equipped on cars aims to create signals to notify other vehicles participating in traffic about the vehicle's operating status such as: stopping, parking, braking, reversing, turning...
Signals are used either by light such as headlamps, brake lights, turn signals….. or by sound such as horns, reverse music….
Just like the lighting system. A signal system circuit usually consists of: battery, fuse, wire, relay, electrical load and control switch. Only some switches of the signal system are on the combination switch. The switches of other signals are usually located in different locations such as in the gearbox or brake pedal……
2. Maintenance and repair
2.1. Turn signals and hazard lights
The installation location of the turn signal is shown in Figure 3.1. The turn signal control switch is located in the combination switch under the steering wheel. Turning this switch to the right or left will make the turn signal turn right or left.
The hazard light switch is used when the vehicle has a problem while participating in traffic. When the hazard light switch is turned on, all the turn signals on the vehicle will light up at a certain frequency. The hazard light switch is usually placed separately from the turn signal switch (some old cars integrate the hazard and turn signal switches on the same combination switch cluster).
Figure 3.1 Turn signal switch Figure 3.2 Hazard switch
The part that generates the flashing frequency for the lights is called a turn signal relay. The turn signal relay usually has 3 terminals: B (positive power supply); E (negative power supply); L (providing the turn signal switch to distribute to the
lamp)
2.1.1. Circuit diagram
To generate the frequency for the turn signal, a turn signal relay is used in the turn signal circuit. The current from the turn signal relay will be sent to the turn signal switch assembly to distribute the current to the turn signal lights for the driver's purpose.
Figure 3.3. Schematic diagram of a turn signal circuit without a hazard switch
1. Battery; 2. Electric lock; 3. Turn signal relay; 4. Turn signal switch; 5. Turn signal lamp; 6. Turn signal lamp; 7. Hazard switch
Figure 3.4 Schematic diagram of turn signal circuit with hazard switch
1. Battery; 2. Combination switch cluster; 3. Turn signal;
4. Turn signal light; 5. Turn signal relay
Today's cars no longer use three-pin turn signal relays (B, L, E) but use eight-pin turn signal relays (figure 3.5) (pin number 8 is used for hazard lights).
For this type, the current supplying the turn signal lights is supplied directly from the turn signal relay to the lights.
div.maincontent .p { color: black; font-family:"Times New Roman", serif; font-style: normal; font-weight: normal; text-decoration: none; font-size: 14pt; margin:0pt; } div.maincontent p { color: black; font-family:"Times New Roman", serif; font-style: normal; font-weight: normal; text-decoration: none; font-size: 14pt; margin:0pt; } div.maincontent .s1 { color: black; font-family:"Times New Roman", serif; font-style: normal; font-weight: normal; text-decoration: none; font-size: 13pt; } div.maincontent .s2 { color: black; font-family:"Times New Roman", serif; font-style: italic; font-weight: normal; text-decoration: none; font-size: 14pt; } div.maincontent .s3 { color: black; font-family:"Times New Roman", serif; font-style: normal; font-weight: normal; text-decoration: none; font-size: 14pt; } div.maincontent .s4 { color: black; font-family:"Times New Roman", serif; font-style: normal; font-weight: normal; text-decoration: none; font-size: 13pt; } div.maincontent .s5 { color: black; font-family:"Times New Roman", serif; font-style: normal; font-weight: normal; text-decoration: none; font-size: 13pt; vertical-align: 1pt; } div.maincontent .s6 { color: black; font-family:"Times New Roman", serif; font-style: normal; font-weight: normal; text-decoration: none; font-size: 11pt; } div.maincontent .s7 { color: black; font-family:"Times New Roman", serif; font-style: normal; font-weight: normal; text-decoration: none; font-size: 14pt; vertical-align: -9pt; } div.maincontent .s8 { color: black; font-family:"Times New Roman", serif; font-style: normal; font-weight: normal; text-decoration: none; font-size: 11pt; } div.maincontent .s9 { color: #008000; font-family:"Times New Roman", serif; font-style: normal; font-weight: normal; text-decoration: none; font-size: 14pt; } div.maincontent .s10 { color: black; font-family:"Times New Roman", serif; font-style: italic; font-weight: normal; te -
 Internal control of revenue and expenditure activities at the National Children's Hospital - 2
Internal control of revenue and expenditure activities at the National Children's Hospital - 2
especially in severe asthma cases, treatment with biological products is required. According to Agache et al., classifying immune responses into two main types: type 2 immune responses and non-type 2 immune responses, identifying inflammatory markers that increase at each time point and in different allergic diseases, thereby helping clinicians choose targeted drugs according to the correct pathophysiological mechanism. Increased blood eosinophil counts predict treatment response to anti-IL4/IL5 antibodies, IL-13, anti-IgE antibodies as well as CRTH2 antagonists 151 .

CONCLUDE
Through research and longitudinal monitoring of 124 children with bronchial asthma with VMDƯ from 6 to 15 years old at the Department of Immunology - Allergy - Rheumatology, National Children's Hospital from October 1, 2016 to December 31, 2019, we drew the following conclusions:
1. Nasal nitric oxide thresholds in asthmatic children with allergic rhinitis.
- The nNO concentration in children with asthma was higher than in children with asthma without asthma and healthy children. The cut-off point of nNO for diagnosing allergic rhinitis in children with asthma was 605 ppb, with a sensitivity of 85.5% and a specificity of 66.7%, the area under the curve was 0.81 with p<0.001.
- The nNO concentration was highest in the severe intermittent asthma group and lowest in the mild intermittent asthma group. The more severe the asthma and the more reduced the respiratory function, the lower the nNO concentration.
- nNO concentration is closely positively correlated with FeNO and allergic factors such as eosinophils in peripheral blood.
2. Asthma control status in children with asthma and allergic rhinitis
- After 6 months of preventive treatment, the rate of complete asthma control in children with HPQ and VMDƯ was lowest according to GINA 2016 standards at 67.5%, and highest according to ACT standards at 96.1%.
- The CARATkids score is capable of distinguishing well the levels of asthma control. With the CARATkids threshold = 4.5, the area under the ROC curve is 0.957; the sensitivity is 100%, the specificity is 79.8% to distinguish the level of asthma control with VMDƯ in children.
- The asthma control rate according to CARATkids is equivalent to the asthma control rate according to FeNO.
- Airway FeNO and nNO concentrations decreased after preventive treatment of asthma and VMDƯ.
3. Asthma phenotype in children with bronchial asthma and allergic rhinitis
- Children with moderate to severe asthma had the highest rate (62.1%) with high FeNO and nNO concentrations, poor asthma control rate and higher ICS dose requirement than the HPQ group with mild asthma.
- Children with HPQ and VMDƯ with nNO level < 605ppb had lower FeNO, IgE concentration, eosinophil count in peripheral blood and respiratory function after 6 months of treatment than the group with nNO level ≥ 605ppb.
- Children with COPD with low FEV1 have a high need for ICS. After 6 months of treatment, this group has a low rate of complete asthma control and a high need for SABA reliever medication.
- Blood eosinophil parameters, blood IgE, FeNO, nNO are inflammatory markers that help in the process of classifying asthma phenotypes, predicting the severity of asthma and predicting the ability to respond to corticosteroid treatment.
SOME LIMITATIONS OF THE STUDY
- Because the HPQ characteristics of children are mainly allergic asthma, the group of bronchial asthma without allergic rhinitis is often small. The limited sample size of the asthma group without allergic rhinitis and healthy children makes it difficult to detect differences in inflammatory factors during the research process as well as treatment prognosis.
- Due to limitations in the study design, we have not been able to design a longitudinal follow-up of the asthma group without VMDƯ in children.
- Assessment of inflammation in bronchial asthma requires assessment of the airways, however, due to technical problems, we used indirect indicators such as eosinophils in peripheral blood. At the same time, in this study, only total IgE testing was performed, not specific IgE testing, which is an important characteristic factor in bronchial asthma.
- nNO concentration is a factor affected by many factors and has a wide range of fluctuations, so the nNO concentration results in this study are different from many other studies. In fact, the world has not yet reached a consensus on the nNO threshold in the diagnosis and monitoring of VMDƯ treatment.
PROPOSAL
Measurement of exhaled nitric oxide concentration (FeNO, nNO) is a non-invasive, easy-to-perform method that objectively assesses inflammation in both the upper and lower airways in older children with asthma and allergic rhinitis. Medical facilities specializing in the field of allergy immunology should be equipped with exhaled nitric oxide concentration measuring machines to diagnose and monitor the treatment of HPQ patients.
In clinical practice, it is necessary to combine medical history, clinical examination with specific tests such as skin prick test with respiratory allergens, respiratory function test and measurement of nitric oxide concentration in the airway to help diagnose and classify asthma phenotypes, thereby choosing the appropriate treatment and dose for each asthma patient. It is necessary to individualize the treatment of bronchial asthma.
Assessment of asthma control and comorbidities should be combined with appropriate toolkits such as CARATkids during disease control monitoring, especially for children with asthma and comorbidities.
LIST OF PUBLISHED WORKS RESEARCH RESULTS OF THE THESIS TOPIC
1. Nguyen Tran Ngoc Hieu, Nguyen Thi Dieu Thuy, Luong Cao Dong (2020). Application of CARATkids questionnaire in asthma control in children with bronchial asthma and allergic rhinitis. Journal of Clinical Medicine and Pharmacy 108, 15(3), 63-67.
2. Nguyen Tran Ngoc Hieu, Luong Cao Dong and Nguyen Thi Dieu Thuy (2020). The role of airway Nitric Oxide in controlling asthma with allergic rhinitis in children. Journal of Medical Research, Hanoi Medical University, 131 (7),141 - 147.
3. H. Nguyen - Tran - Ngoc, Th. Nguyen - Thi - Dieu, D. Luong - Cao et al (2021). Study of control status in children with bronchial asthma and allergic rhinitis. J Func Vent Pulm, 37(12).13-19.
REFERENCES
1. Masoli M., Fabian D., Holt S. et al (2004). The global burden of asthma: executive summary of the GINA Dissemination Committee report. Allergy, 59(5), 469-478.
2. Bousquet J., Khaltaev N., Cruz AA et al (2008). Allergic rhinitis and its impact on asthma (ARIA) 2008. Allergy, 63, 8-160.
3. Thomas M., Kocevar V.S., Zhang Q. et al (2005). Asthma-related health care resource use among asthmatic children with and without concomitant allergic rhinitis. Pediatrics, 115(1), 129-134.
4. Schatz M., Sorkness CA, Li JT et al (2006). Asthma Control Test: reliability, validity, and responsiveness in patients not previously followed by asthma specialists. J Allergy Clin Immunol, 117(3), 549-556.
5. Borrego LM, Fonseca JA, Pereira AM e. al (2014). Development process and cognitive testing of CARATkids-Control of Allergic Rhinitis and Asthma Test for children. BMC pediatrics, 14(1), 1-9.
6. Ngo Quy Chau and Vo Thanh Quang (2016). Recommendations for diagnosis and treatment of asthma with allergic rhinitis. Medical Publishing House, Hanoi.
7. Lundberg JON, Szallasi TF, Weitzberg E. et al (1995). High nitric oxide production in human paranasal sinuses. Nature medicine, 1(4), 370-373.
8. The American Thoracic Society and The European Respiratory Society (2005). ATS/ERS recommendations for standardized procedures for the online and offline measurement of exhaled lower respiratory nitric oxide and nasal nitric oxide. Am J Respir Crit Care Med, 171(8), 912-930.
9. Krantz C., Janson C., Borres MP e. al (2014). Nasal nitric oxide is associated with exhaled NO, bronchial responsiveness and poor asthma control. Journal of breath research, 8(2), 026002.