Nessler solution must have a certain alkalinity. Usually adjusted as follows: 11 - 11.5 ml of Nessler solution needs 20 ml of 1N HCl to neutralize (phenolphthalein color indicator). If quantifying N outside of protein, 1 ml of 50% H 2 SO 4 needs 9 - 9.3 ml of Nessler solution to neutralize.
Standard nitrogen solution ( 1 ml contains 0.03 mgN).
Dry ammonium sulfate (AR) at 110 0 C for 30 minutes and place in a desiccator. Weigh accurately 0.1415 g of ammonium sulfate into a 1 liter flask, then add 1 ml of concentrated HCl to inhibit bacterial growth, then add distilled water to 1000 ml.
Digestive solution :
Phosphoric acid (H 3 PO 4 ) 300ml
Copper sulfate 5% (CuSO 4 ) 50ml
Mix well and add 100 ml of concentrated H2SO4. Let stand for 1 week. Take the clear water above and double it with distilled water.
Sulfuric acid 50%
V
V
Take 10 parts of 50% sulfuric acid and 1 part of the above solution and mix well to get a digestive solution. 1 ml of this solution requires 9 - 9.3 ml of Nesler's solution to neutralize, otherwise its acidity must be adjusted.
Operation steps
Mix well and heat the test tube. A few glass beads may be added. Heat until clear.
tube full of smoke, bottom of tube from black to transparent. Let cool. Mix well, compare color with blue filter or = 440 m Calculate
Test E / Standard E x 0.03 x 100 = mg% Nitrogen outside protein 0.1
Attention:
1. After adding Nessler, the cloudy solution may be due to:
+ Nessler's acid-base test is not standard.
+ Not boiled enough, the bottom of the tube is not transparent.
+ Leave too long to compare colors.
+ The concentration of protein outside the protein is too high.
Distilled water used to prepare reagents must be completely free of nitrogen .
How to make distilled water without Nitrogen: The distilled water distillation set is made entirely of glass. Add 2000 ml of distilled water, 0.25 ml of H 2 S 0 4 4 N and 2 ml of 1% potassium permanganate (KMnO 4 ) and distill, discarding the first and last part of the water.
After adding Nessler, if no color appears, it may be due to too much digestive solution or not being digested completely during boiling.
* Blood urea determination
Urea in the blood after reacting with urease enzyme will be converted into ammonium carbonate H 2N – CO – NH 2 + 2 H 2 O ( NH 4 ) 2 CO 3
( NH 4 ) 2 CO 3 + 2 NaOH Na 2 CO 3 + 2 NH 4 OH
Then react with Nessler solution to show color. Do the same with the standard solution to calculate the amount of urea to be quantified.
Test kit :
1. Standard nitrogen solution (1ml contains 0.05 mg N; prepare as for nitrogen determination outside )
protein)
2. Sodium diphosphate acid solution ( Na 2 HPO 4 ): weigh 0.89 g of sodium diphosphate acid (Na 2 HPO 4 .12 H 2 O) CP) and mix with distilled water to 100 ml.
3. Glycerin ureza extract: Take 5g of soybean powder, add 100ml of glycerin, shake for 15 minutes, leave in the incubator for 24 hours. Take the clear liquid above to use and store in the refrigerator for 2-3 months.
4. Sodium tungstate 10%; 5. H 2 SO 4 2/3 N;
6. Nessler's solution
Operation:
Using a small test tube (15 x 100mm), add 0.5 ml of whole blood, 0.5 ml of distilled water, 0.25 ml of disodium phosphate acid and 0.25 ml of urease solution. After mixing well, soak in a cup of 37 o C water for 20 minutes. Take out, add 1.5 ml of distilled water, 1 ml of 10% sodium tungstate and 1 ml of 2/3 N H 2 SO 4. Mix well and centrifuge or filter through paper, take the clear water above and send it for testing in the following order:
Steps
The | tube | (ml) | ||
white tube | standard tube | test tube | ||
Blood water | 0 | 0 | 2.0 | |
Standard solution (0.03 mg N/ml) | 0 | 1.0 | 0 | |
Distilled water | 8.0 | 7.0 | 6.0 | |
Nessler solution | 2.0 | 2.0 | 2.0 | |
Maybe you are interested!
-
 Dpcsv Curve And Standard Addition Graph For Determination Of Selenium Form In Aqueous Phase After Defatting With 5ml N-Hexane (1 Time)
Dpcsv Curve And Standard Addition Graph For Determination Of Selenium Form In Aqueous Phase After Defatting With 5ml N-Hexane (1 Time) -
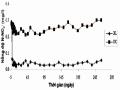
 N-No2- Concentration (Mg/l) of Treatment Area and Control Area During the Test Period: (♦) Treatment Area, (■) Control Area.
N-No2- Concentration (Mg/l) of Treatment Area and Control Area During the Test Period: (♦) Treatment Area, (■) Control Area. -
 Diagnosis of livestock diseases - Hanoi University of Agriculture - 13
Diagnosis of livestock diseases - Hanoi University of Agriculture - 13 -
 Standard Teaching Hour Norms of Lecturers at Khxhnv University - Hanoi National University According to Each Position
Standard Teaching Hour Norms of Lecturers at Khxhnv University - Hanoi National University According to Each Position -
 Solution 2: Manufacturing Enterprises Must Regularly Maintain Transaction Activities With Partners To Increase Proficiency, Create
Solution 2: Manufacturing Enterprises Must Regularly Maintain Transaction Activities With Partners To Increase Proficiency, Create

Mix well and compare the color immediately. Use a blue filter or = 440 m
Calculate: Calculate: mg% urea nitrogen =
I fall
I'm right
x 0.03 =
I fall
I'm right
x 15
Attention
- The pH of the ureza medium is best near neutral. If not neutral, use
Sodium phosphate solution to adjust.
- If using pure ureza powder, it can be added directly into the blood: 0.5 ml of blood for 1 mg
urease
- Nessler solution contains mercury and other heavy metal ions, which can inhibit
effect of urease. Therefore, the tubes used for testing must be extremely clean.
- After adding Nessler solution, if the vial is still cloudy, it is likely due to the room temperature being too high. This can be fixed by soaking the tubes in a cup of cold water during the color development step, adding Nessler solution to develop the color and comparing the color immediately.
mg% urea nitrogen x 2.143 = mg% urea
(Because the molecular weight of urea = 60, including 2 nitrogen atoms, from which we have:
- Distilled water must be nitrogen free.
7. Blood cholesterol
60
2,143 )
28
Cholesterol in the blood, in muscle and nerve tissues, especially in the brain.
Free cholesterol, cholesterol (ester) in food, through digestion in the small intestine, in fat droplets absorbed into the blood. Endogenous sources are synthesized mainly in the liver's basal cells from acetyl CoA. In addition to the liver, cholesterol is also synthesized in a number of other tissues.
The liver plays a huge role in regulating blood cholesterol levels.
In the liver, the esterification of cholesterol occurs to form cholesterol (cholesterol ester). It is the main source of cholesterol in the plasma. When liver cells are damaged, blood cholesterol
decrease, and therefore, the ratio:
Cholesterite Acidic cholesterol
decrease. The rate is decreasing.
The disease is more severe. Often seen in infectious and toxic hepatitis.
severe, cirrhosis, prolonged jaundice...
Exogenous cholesterol in fat droplets reaching the liver is hydrolyzed by the enzyme Cholesterol esterase in the liver. After hydrolysis, it is re-esterified to participate in plasma lipoprotein.
The liver plays a particularly important role in the following cases :
- Produces 7-dehydrocholesterol (pre-vitamin D3 ) which is brought to the skin and, under the influence of ultraviolet rays, turns into Vitamin D3 ( cholecalciferol).
- Cholesterol oxidation forms bile acids that are secreted into the intestine and reabsorbed.
Cholesterol is excreted in bile acids to the intestine, mixing with dietary cholesterol.
- Part of the cholesterol in the intestine that is not fully reabsorbed will be in the stool, and can be oxidized by intestinal bacteria into coprostanol. There is always little cholesterol and coprostanol in the stool.
* Determination of total cholesterol using Ferric chloride reagent
Principle : Blood water has protein removed from the solution thanks to Ferric chloride acid, there is cholesterol dissolved in it. Cholesterol in blood water reacts with concentrated sulfuric acid.
And Fe +++ will become a stable purple-red derivative. Also treat the standard Cholesterol solution in the same way and then deduce the Cholesterol concentration in the serum.
Test kit :
1. Concentrated acetic acid (AR)
2. Ferric chloride stock solution : Weigh 840 mg of Ferric chloride (FeCl 3 .6 H 2 O) into a 100ml flask. Add concentrated acetic acid, stir until dissolved, then add up to 100ml .
3. Ferric chloride solution used: Mix one part of the original Ferric chloride solution and add 9 parts of concentrated acetic acid (mix when using).
4. White Ferric chloride solution : Take 8.5 ml of the original Ferric chloride solution and add concentrated acetic acid to 100 ml.
5. 0.85 % Sodium chloride solution .
6. Standard Cholesterol solution (1ml contains 1mg). Weigh 100 mg of Cholesterol (AR) into a 100 ml volumetric flask, dissolve with concentrated acetic acid and dilute to the 100 mark .
7. Standard Cholesterol solution for use (1ml contains 0.1 mg). Take 10 ml of standard Cholesterol stock into a 100ml bottle, add 98.5 ml of standard Ferric chloride solution, then add concentrated acetic acid to 100 ml (mix when using).
8. Concentrated sulfuric acid (AR) .
Action:Action:
Add 0.05 ml of serum (or plasma) to the centrifuge tube.
Add 4 ml of Ferric chloride solution; add while shaking, stir well and let stand for 10 minutes. Centrifuge for 2 minutes. Take 3 ml of clear water above and put it in a wide-mouth test tube as a test tube (not quantitative).
In another test tube, add 0.05ml of saline, 1ml of standard cholesterol solution (1ml has 0.1 mg) and 3ml of white Ferric chloride solution. Pipette 3ml into the standard tube.
Next steps:
Steps
The | tube, | ml | ||
white tube | standard tube | test tube | ||
Blood Water (4) | 0 | 0 | 3.0 | |
Prepared standard cholesterol solution (5) | - | 3.0 | 0 | |
White Ferric Chloride Solution | 3.0 | 0 | 0 | |
Sulfuric Acid | 2.0 | 2.0 | 2.0 | |
Shake well immediately. Place green filter or = 500 m in colorimeter.
Calculation: mg% cholesterol =
I fall
I'm right
x 200
Cholesterol ester determination
Blood water has been deproteinized with acetone alcohol mixture, digitonin is added to combine with hydroxyl of free cholesterol to form a stable digitonin cholesterol complex that settles to the bottom and is separated.
After washing, the precipitate reacts with ferric chloride and sulfuric acid to develop color. Calculate the amount of free cholesterol. Total cholesterol minus free cholesterol equals the amount of cholesterol.
Test kit :
Operation:
1. Acetone alcohol: equal amounts of ethyl alcohol and acetone.
2. Digitonin 1%: 1g digitonin mixed with 50% ethyl alcohol to 100ml.
3. Other reagents are the same as for total cholesterol determination.
1. Add 0.1ml of serum to a graduated centrifuge tube.
2. Add 5ml of acetone, shake well, seal the tube, and let stand for 30 minutes.
3. Add more acetone to make the total solution 5ml, shake well and centrifuge for 5 minutes.
4. Take the 2.5 ml above and put it into another centrifuge tube, then boil it in a water bath to evaporate to 0.5 ml. While the tube is still hot, add 0.25 ml of 1% digitonin. Shake well and let stand for 20 minutes.
5. Centrifuge for 5 minutes, pour away the clear water above. Add 4ml of acetone to wash the precipitate at the bottom, then centrifuge for another 5 minutes. Discard the clear water above and turn the tube upside down to drain all the water. Use this tube as a free cholesterol test tube.
6. In another tube, test for total cholesterol. The next steps are as follows:
Steps
Tubes, ml | ||
total cholesterol tube | free cholesterol | |
Serum Ferric chloride solution used Ferric chloride solution white | 0.05 4.00 0 | 0 0 0.4 |
Use a glass rod to mix well, let stand for 10 minutes then centrifuge for 2 minutes. Take the clear liquid and follow order of each tube | ||
Clear water on top Concentrated sulfuric acid | 3.0 2.0 | 3.0 2.0 |
Mix well immediately, after 5-10 minutes compare the color. Standard tube, blank tube, colored filter, calculation formula is the same as total cholesterol quantification. The number found is the amount of free cholesterol and total cholesterol.
Cholesterol quantification according to Inc.
The principle is that cholesterol in the serum combines with concentrated acetic acid , acetic anhydride and concentrated sulfuric acid to form a green complex. The color of the complex is proportional to the amount of cholesterol in the blood. The same treatment is performed with a cholesterol solution of known concentration to then, through colorimetric comparison with a photometer, deduce the amount of cholesterol in the blood;
a. Concentrated acetic acid – 1 part;
b. Acetic anhydride – 5 parts;
c. Sulfuric acid – 1 part;
Mix the above 3 ingredients together in the order of mixing the first two ingredients (a) and (b) first, refrigerate at 4 o C, then slowly add sulfuric acid. Always keep this mixture in the refrigerator, take it out when using.
Standard cholesterol solution: 100mg Cholesterol and chloroform to exactly 100ml.
Take 10 ml of the above stock solution into a volumetric flask, then add chloroform to 100 ml. 1 ml of this solution contains 0.1 mg of cholesterol.
Making samples:
Take 5 clean, dry test tubes and add the following substances:
Substances
Test tubes | |||||
1 | 2 | 3 | 4 | 5 | |
Standard mL of Cholesterol (0.1 mg) | 0.5 | 1 | 1.5 | 2 | 2.5 |
Actual mL of Cholesterol | 0.05 | 0.10 | 0.15 | 0.20 | 0.25 |
Cholesterol in 100 | |||||
ml | 50 | 100 | 150 | 200 | 250 |
serum (mg %) | |||||
Place all 5 tubes in a water bath to evaporate completely. Note, chlorform is very flammable, so be very careful when heating. Add 2.1 ml of reagent to each tube, shake well, heat in a water bath at 30 0 C for 20 minutes and compare the color immediately afterwards. Draw a graph.
Consider the proposal
Use 2 clean , dry test tubes and add the following substances :
quiet consultation | white tube | |
Fresh serum | 0.1ml | 0 |
Reagents | 2.0 | 2.1 |
Mix well. Heat in water bath at 30 0 C for 20 minutes and compare color immediately with photometer, 0.5 cm cuvette; red filter.
Calculate Cholesterol content according to sample chart.
diagnostic meaning
Cholesterol increases and decreases with age, diet, and increases during pregnancy.
- Increased total cholesterol : jaundice due to biliary obstruction, kidney failure, arteriosclerosis, high blood pressure.
- Total cholesterol decreased : Severe cirrhosis , infectious hepatitis; Some severe and prolonged infectious diseases; thyroid cysts, adrenal insufficiency.
gravel
- Cholesterol reduction : Hepatitis , infection, cirrhosis. Chronic hepatitis, jaundice due to
To distinguish jaundice due to liver or extrahepatic causes, one can refer to the
following transformation:
Biliary obstruction :
+ Total cholesterol increased,
+ Coefficient:
Cholesterol Total cholesterol
Normal.
Liver disease :
+ Total cholesterol decreased or normal
+ Coefficient
Cholesterol Total cholesterol
reduce
8. Serum calcium
Calcium is the main component of blood plasma, absorbed into the body through the small intestinal mucosa. After entering the body, a large amount of calcium is deposited in the bones, a small part in the cartilage.
Vitamin D plays a very important role in the absorption of calcium in the intestines, the process of calcium circulation in the body and keeping the calcium concentration in the blood relatively stable; After vitamin D are the thyroid gland, kidneys and liver.
The above process follows the following mechanism: vitamin D is absorbed in the small intestine by the action of bile or synthesized in the skin and transported to the liver. In the liver, under the action of the enzyme 25-hydroxylase, vitamin D is converted into 25-hydroxy-vitamin D (25-OH-D). This process occurs in the microsomes of liver cells.
25 – OH – D is metabolized to the kidneys, and here, thanks to the enzyme 1, hydroxylase of mitochondria in the renal tubule intercellular space, it is converted into 1,25 – dihydroxy - Vitamin D (1,25 –(OH) 2 – D) which promotes calcium absorption in the intestine and mobilizes calcium from bones into the blood.
The regulation of 1,25-(OH) 2 -D synthesis depends on the concentrations of calcium, phosphorus and parathyroid hormone in the blood. When blood calcium decreases, the parathyroid gland is stimulated to secrete more parathyroxine, which strongly stimulates the activity of enzyme 1, in the kidney hydroxydaza, increasing the synthesis of 1,25-(OH) 2 -D, thereby increasing calcium absorption in the intestine and mobilizing calcium from the bones into the blood, increasing blood calcium. When blood calcium increases, parathyroxine secretion is inhibited, thereby reducing the synthesis of 1,25-(OH) 2 -D.
When cattle are pregnant, during the time when young cattle are growing, their bones are hardening and developing, requiring a lot of Calcium PO 4 -- and Vitamin D. Lack of one of these substances will cause calcium metabolism disorders.
Increased serum calcium : hyperparathyroidism, bone cancer, ...
Hypocalcemia : rickets, postpartum paralysis, calf convulsions , anemia, nephritis, hypoparathyroidism .
* Serum Calcium Quantification
Potassium permanganate titration method
Principle : Calcium in serum reacts with ammonium oxalate to precipitate calcium oxalate. Use ammonia water to wash away excess ammonium oxalate, then dissolve calcium oxalate with sulfuric acid. Finally, titrate with potassium permanganate solution to know how much calcium precipitates per ml.
From there calculate the calcium content in the serum.
Substance containing Calcium + (NH 4 ) 2 C 2 O 4 CaC 2 O 4 + ammonium salt CaC 2 O 4 + H 2 SO 4 CaSO 4 + H 2 C 2 O 4
2KMnO 4 + 3 H 2 SO 4 + 5 H 2 C 2 O 4 K 2 SO 4 + 2MnSO 4 + 10 CO 2 + 8 H 2 O
Test kit :
1. Ammonium oxalate 4%
2. 2% ammonia water
Ammonia water (d = 0.9) 2ml Distilled water to 100 ml
3. Sulfuric acid 1N
4. Sodium oxalate 0.01N
6.7 g Sodium oxalate (Na 2 C 2 O 4 CP ., dry at 110 0 C for 3 hours), add a little distilled water, stir until dissolved and put into a 1000 ml volumetric flask. Add 5 ml of pure concentrated sulfuric acid,
Then add water to 1000 ml to get 0.1N Sodium oxalate. Measure exactly 10 ml of the above solution into a 100 ml volumetric flask, then add distilled water to make 100 ml (mix when using).
5. 0.01 N potassium permanganate (1 ml precipitates 0.2 mg of calcium). Take 10 ml of 0.1 N potassium permanganate into a 100 ml volumetric flask and add distilled water to make 100 ml. This solution is easy to change concentration. Therefore, it needs to be corrected before use.
Correction method : Put into a test tube 2 ml of0.01 N Sodium oxalate, 2 ml of 1N H 2 SO 4. Boil both tubes in a water bath for one minute to let the temperature in the tube reach about 75 oC, then use 0.01N Potassium permanganate (needs correction) to titrate until a stable pink color appears.
Correction factor=
Operation
2
Number of ml of KMnO 4 used _ Number of ml of KMnO 4 used for the calibration tube for the distilled water tube
Put into a centrifuge tube 1 ml serum, 3 ml distilled water and 1 ml 4% ammonium oxalate, stir well, leave for 30 minutes, centrifuge quickly for 5-10 minutes. Turn upside down to pour out all the clear water. Leave the centrifuge tube upside down on absorbent paper to absorb all the remaining water.
Add 4 ml of 2% ammonia water, stir well, centrifuge for 5-10 minutes, pour out the clear water.
Wash like that one more time, finally turn the tube upside down on absorbent paper for 5 minutes to absorb all the remaining water. Add 2ml of 1N H2SO4 to dissolve Calcium oxalate. Put it in the tube and boil it in a water bath. When the temperature in the tube is about 75oC, use a graduated 1ml pipette, titrate with 0.01N Potassium permanganate until the color does not disappear. Record the number of ml of 0.01N KMnO4 used .
100
Calculation: mg% = Number of ml of KMnO 4 used x adjustment factor x 1
9. Serum inorganic phosphorus level
Inorganic phosphorus element has special significance for animal life. It participates in the structure of the skeleton (nearly 87% of phosphorus in the body); it is an important component of many organic compounds in the body.
Phosphorus is present in the body in two forms.
- Inorganic salts include ortho and pyrophosphate. Inorganic phosphorus is distributed equally in plasma and red blood cells.
- Organic compounds of phosphoric acid with nucleotides, carbohydrates, lipids, proteins or in the form of diphosphoglyceric acid in red blood cells.
Phosphorus is present in blood and serum, but serum phosphorus is usually measured
bar.
* Serum phosphorus quantification ( according to Brigs , Uxovit improved )
Principle : Serum protein is precipitated with trichloracetic acid. Protein-free blood with soluble phosphorus is added to ammonium molybdate , which combines with inorganic phosphorus to form phosphomolybdic acid. Phosphomolybdic acid is deoxidized by hydroquinone and in the presence of sodium sulfite to form a blue derivative. The intensity of the blue color is proportional to the amount of phosphorus in the blood.
Chemical
1. 20% acetic acid, store in refrigerator.
2. Ammonium molybdate
- 25 g Ammonium molybdate dissolved in 300 ml distilled water;
- Slowly dissolve 75 ml of concentrated H 2 SO 4 in 125 ml of distilled water. Mix the two together.
3. Hydroquinone 1% : Put 1 g of Hydroquinone into a 100 ml bottle, add a little distilled water and dissolve, then add distilled water to 100 ml. Add 1 drop of concentrated H 2 SO 4 .
4. Sulfite carbonate solution:
- Dissolve 40 g of anhydrous Na 2 CO 3 in 200 ml of water;
- 7.5 g Na 2 SO 3 (Sodium sulfite) anhydrous in 50 ml of water. If anhydrous Na 2 SO 3 is not available , it can be replaced with 15 g of crystalline Na 2 SO 3 .
5. Standard phosphorus solution :
a. Stock solution : Weigh 4.394 g KH 2 PO 4 (weigh with analytical balance) into a 1 liter volumetric flask and add distilled water up to the 1 liter mark .
b. Standard solution : Add 2 ml of the stock standard solution to a 100 ml volumetric flask, then add distilled water to 100 ml. 1 ml of this solution contains 0.02 mg P.
Conduct quantitative analysis
Put 1 ml of serum in a test tube, add 2 ml of distilled water and 1 ml of 20% trichloracetic acid, shake well, leave for a few minutes, and centrifuge to remove protein.
Take 2.5 ml of the above filtrate into another test tube, add 0.5 ml of hydroquinone solution. Leave for 5 minutes. Next, add 2 ml of carbonate sulfite drop by drop, and finally add distilled water to have a total volume of 6 ml. Leave for 10 minutes and then measure the color on a photometer. From the optical density reading on the machine and compare with the sample to calculate the phosphorus content in the serum.
Making a sample :
Take 5 test tubes and write numbers from 1 to 5. Add chemicals in the order of the following table, ml:
Substances
1 | 2 | 3 | 4 | 5 | |
1. Standard phosphorus solution (0.02 mg/ml) | 0.5 | 1.0 | 1.5 | 2.0 | 2.0 |
2. Distilled water | 2.0 | 1.5 | 1.0 | 0.5 | 0 |
3. 20% acetic trichloride acid | 0.5 | 0.5 | 0.5 | 0.5 | 0.5 |
4. Ammonium molybdate | 0.5 | 0.5 | 0.5 | 0.5 | 0.5 |
5. Hydroquinone | 0.5 | 0.5 | 0.5 | 0.5 | 0.5 |
6. Carbonate – sulfite | 2.0 | 2.0 | 2.0 | 2.0 | 2.0 |
Phosphorus content, mg% | 2.0 | 4.0 | 6.0 | 8.0 | 10.0 |
Shake the tubes well, then let stand for 10 minutes. Compare the color on the photometer.
Note: Make a blank tube by replacing the standard phosphorus solution with distilled water, and the other components are the same as the table above (from “3” to “6”).
* Determination of inorganic phosphorus ( According to Ivanov )
Test drug
1. 20% acetic trichloride acid